Ed Friedlander, M.D., Pathologist
scalpel_blade@yahoo.com


Cyberfriends: The help you're looking for is probably here.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com Your confidentiality is completely respected.
 DoctorGeorge.com is a larger, full-time service.
There is also a fee site at myphysicians.com,
and another at www.afraidtoask.com.
DoctorGeorge.com is a larger, full-time service.
There is also a fee site at myphysicians.com,
and another at www.afraidtoask.com.
Translate this page automatically
 |
With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource. Someday you may be able to access these pictures directly from this page.
Also:
Medmark Pathology -- massive listing of pathology sites
Freely have you received, freely give. -- Matthew 10:8. My
site receives an enormous amount of traffic, and I'm
handling about 200 requests for information weekly, all
as a public service.
Pathology's modern founder,
Rudolf
Virchow M.D., left a legacy
of realism and social conscience for the discipline. I am
a mainstream Christian, a man of science, and a proponent of
common sense and common kindness. I am an outspoken enemy
of all the make-believe and bunk that interfere with
peoples' health, reasonable freedom, and happiness. I
talk and write straight, and without apology.
Throughout these notes, I am speaking only
for myself, and not for any employer, organization,
or associate.
Special thanks to my friend and colleague,
Charles Wheeler M.D.,
pathologist and former Kansas City mayor. Thanks also
to the real Patch
Adams M.D., who wrote me encouragement when we were both
beginning our unusual medical careers.
If you're a private individual who's
enjoyed this site, and want to say, "Thank you, Ed!", then
what I'd like best is a contribution to the Episcopalian home for
abandoned, neglected, and abused kids in Nevada:
My home page
Especially if you're looking for
information on a disease with a name
that you know, here are a couple of
great places for you to go right now
and use Medline, which will
allow you to find every relevant
current scientific publication.
You owe it to yourself to learn to
use this invaluable internet resource.
Not only will you find some information
immediately, but you'll have references
to journal articles that you can obtain
by interlibrary loan, plus the names of
the world's foremost experts and their
institutions.
Alternative (complementary) medicine has made real progress since my
generally-unfavorable 1983 review linked below. If you are
interested in complementary medicine, then I would urge you
to visit my new
Alternative Medicine page.
If you are looking for something on complementary
medicine, please go first to
the American
Association of Naturopathic Physicians.
And for your enjoyment... here are some of my old pathology
exams
for medical school undergraduates.
I cannot examine every claim that my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship
by suspending their own reasoning and
simply accepting a single authority that seems wise and good.
I've learned that they leave the movements when, and only when, they
discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer
answer my crank mail.
This site is my hobby, and I presently have no sponsor.
This page was last updated February 6, 2006.
During the ten years my site has been online, it's proved to be
one of the most popular of all internet sites for undergraduate
physician and allied-health education. It is so well-known
that I'm not worried about borrowers.
I never refuse requests from colleagues for permission to
adapt or duplicate it for their own courses... and many do.
So, fellow-teachers,
help yourselves. Don't sell it for a profit, don't use it for a bad purpose,
and at some time in your course, mention me as author and KCUMB as my institution. Drop me a note about
your successes. And special
thanks to everyone who's helped and encouraged me, and especially the
people at KCUMB
for making it possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it,
here or elsewhere. Health and friendship!
It is difficult to imagine the "politically correct" revision of Victor Hugo's work as The Angular
Kyphotic of Notre Dame.
-- Joe Segen
Bone and joint #'s 1-56, 107-246 (tumors begin at 132)
You know bone supports you, protects you, and stores your calcium and phosphorus. You know
osteoblasts in their rows making the super-densely-woven collagen that is osteoid, osteocytes in their
lacunes (hard to study, but not inert),
multinucleated (usually; 3-20) osteoclasts with ruffled contact surfaces in their Howship's lacunes,
compact cortical bone, spongy cancellous bone, and so forth. You know that bone perennially
remodels itself. (This is why the orthodontist can straighten teeth.) You also know that
unmineralized bone is called osteoid, which is mostly dense-woven type I collagen, with some
vitamin K dependent calcium-binding proteins mixed in.
* The great mystery of how osteoblasts and osteoclasts cooperate so that
there will be just the right amount of bone is on its way to being solved.
CBFA1 is the factor that osteoprogenitor cells
make to turn themselves into osteoblasts (Bone 25: 107-8, 1999); its levels decrease markedly with age.
Working osteoblasts make RANKL, a membrane-bound protein factor that binds to RANK
on osteoclast precursors and turns them into osteoclasts,
and also osteoprotegerin, which interferes with the interaction.
Obviously something is missing from the picture; since bone grows along
lines of stress, it may be an electrical phenomenon.
See JAMA 292: 490, 2004; NEJM 353: 918, 2005.
Remember that interleukin-6 is a strong osteoclast activator; this probably
accounts for the bone wasting seen especially in rheumatoid arthritis.
When bone is being newly-formed, collagen fibers for the osteoid are laid down.
This may be as crisscross woven bone, made rapidly and able to withstand
stress equally well in all directions, or lamellar bone, with collagen
fibers nearly parallel, which takes
longer to make but is much stronger. The osteoblasts are also
responsible for beginning the process of mineralization, but this can't be
the whole story, since a row of osteoblasts typically overlies an unmineralized
"osteoid seam".
In an adult, normal bone is entirely lamellar, and most pathological bone is woven. They are easy to
distinguish using polarized light. This is convenient.
Bone is decalcified prior to histologic sectioning,
but bone that was calcified is less homogeneously dense-pink
than bone that was never calcified ("osteoid").
Since it takes about two weeks to mineralize osteoid, wide osteoid seams beneath the
osteoblasts mean bone is being laid down fast or not being mineralized. Narrow osteoid seams mean
the osteoid is being laid down slowly.
You can label the osteoid that mineralized today by administering tetracycline. This will impart a
permanent yellow color and distinct fluorescence to the seam. (Yes, if you were on tetracycline for a
while for your acne, your skeleton is much more yellow and much more fluorescent than your
friend's.)
Diaphysis... The long shaft, remote from both growth plates
Epiphysis... Between the growth plate and the nearest joint
Metaphysis... Between the growth plate and the diaphysis. In kids, this is where most of the bone
growth is taking place, so this is where most pediatric bone disease (infections, tumors) will occur.
You remember that when osteoblasts are working (growth, healing fractres, bone disease),
they produce extra alkaline
phosphatase, which shows up in the serum. You can tell when new collagen is being laid down (i.e.,
healing bone, Paget's, others) by increased urinary hydroxyproline.
You can spot dead bone under the microscope because there are no osteocytes in the lacunes.
You remember that in scurvy, osteoid fails to form, while in rickets, osteoid fails to mineralize.
(Future radiologists: In kids, look for sawtooth rib-cartilage junctions in both
deficiencies.) You also remember the
"brown tumors" of hyperparathyroidism from any cause; these regress when the hyperparathyroidism is treated.
There's considerable bony variability among normal people. Stature, of course, is entirely the result
of bone growth (and, in age, of bone deterioration). Stature is mostly genetic; you know the effects
of poor nutrition, chronic disease, hGH excess and deficiency, and osteogenesis imperfecta;
precocious puberty will first make you taller than your peers, then your epiphyses close and you
may end up shorter in the long run. (It's actually the estrogens
that close the epiphyses: Lancet 357: 1723, 2001, which is why
we give an aromatase inhibitor when we treat boys with constitutional
delayed puberty). If you get your sex hormones late (or never), you're likely to be tall.
A missing or extra (i.e., cervical) rib is generally a mere incidental finding. A missing phalanx or
even radius isn't particularly disabling. Various anomalies of bone formation are a radiologist's and
geneticist's fascination. * Bone "cysts" are usually mis-named, since they aren't usually lined by real epithelium.
FRACTURE TERMS
Stress fracture: The bone fractures after repeated extra stress, i.e.,
there were some tiny microfractures first and the bone was already a bit sore
Greenstick fracture: The bone is cracked, but not broken into two pieces. "Incomplete" fracture.
Closed fracture: The overlying tissues are intact
Open fracture: The bacteria have a route from the surface to the bone; perhaps the bone is even
sticking out the wound.
Comminuted fracture: The bone is broken into several pieces.
Pathologic fracture: Due to intrinsic disease of the bone; the force would not have broken a normal
bone. Seen in osteoporosis, cancer, osteogenesis imperfecta, others.
Procallus: Fibrin / granulation tissue bump forming from the hematoma at the fracture site. "Provisional
callus".
Callus: Granulation tissue bump at the fracture site that is starting to turn into fibrous tissue and
cartilage, from which healed bone will arise. Eventually becomes bony callus and then remodels to
look more or less like the original bone.
Pseudarthrosis: The ends of the bone did not heal back together with bone. At best, there is fibrous
scar connecting the ends, and a "false joint" is created.
If the fracture is comminuted, if the ends of the bones are much displaced, or if infection happens,
don't expect good healing. Likewise, poorly-nourished people or osteoporotic people are likely to
get bad results.
* Future pathologists: Don't be fooled by post-mortem "heat fractures"
of bones in burned bodies. These are caused by boiling of the bone marrow.
{07029} healing fracture, histology
Four days: Periosteal new born formation beginning
Ten days: Fracture line no longer visible; soft callus present
Fourteen days: Hard callus present
Twenty-one days: Callus is all hard
Ninety days: Bone has remodelled
A family of diseases having in common defective synthesis of type I collagen.
* The molecular biology has been extensively worked out (Clin. Orth. 343: 23, 1997.
Here are the subtypes:
Type I... Make too little pro-α1(1). Normal statue, lax joints, hard of hearing (another mutation:
J. Clin. Invest. 85: 282, 1990).
Type II... Pro-α1(1) is too short, etc.
The collagen is made but poorly secreted.
Bones break in utero or during birth, killing the child (yet
another mutation: J. Clin. Invest. 83: 574, 1989)
Type III... Triple helix doesn't form well. Short, many fractures, progressive kyphosis, hard of
hearing, bad cases are lethal in childhood
Type IV... Pro-α2(2) is too short, etc. Short stature, somewhat fragile bones
And if you look hard, you find many "forme fruste" people whose bones
are just a bit more fragile (J. Clin. Invest. 97: 1035, 1996).
Most are autosomal dominant; type II are either autosomal recessive or new autosomal dominant
mutations. (Explain.) In most cases, the teeth are deformed. Except for
type IV, all feature distinctive blue sclerae. (The "blue" color results from the translucence of the
collagen. Don't rely on this, and don't go calling every relatively dark sclera "blue").
Bisphosphonate for osteogenesis imperfecta: After some early flops, new reports of
success. NEJM 339: 947, 1998; Pediatrics 111: 573 & 601, 2003, Lancet 363: 1427, 2004,
others; it is now standard.
Bone marrow transplantation: Nat Med. 5: 309, 1999.
Gene therapy and somatic cell therapy
are under investigation (Clin. Orth. 379-S: S126, 2000).
Achondrogenesis II: Lethal mutation in COL2A1
* Osteogenesis imperfecta must be ruled out in children with
fractures attributed to abuse. This isn't difficult.
I used to be asked about "temporary brittle bone disease"
and after examining the evicence, decided that I don't believe in it.
Update: The physician who "discovered" this is now
in court for making stuff up (Br. Med. J. 328: 187, 2004).
OSTEOPETROSIS ("marble bones", "Albers-Schonberg disease";
Am. Fam. Phy. 57: 1293, 1998)
This family of diseases features progressive obliteration of the marrow cavity by bone. This is bad
because (1) the bones become very brittle, and (2) the patient is likely to die of neutropenia or
anemia.
Most of these diseases are autosomal dominant (usually mild)
or autosomal recessive (usually severe). The genetics
of both have not been fully worked out (J. Clin. Endoc. Metab. 84:
1047, 1999).
Other patients lack carbonic anhydrase II, and
the osteoclasts die of too much acid (Hum. Genet. 99: 634, 1997;
Blood 97: 1947, 2001). Yet another features a faulty chloride channel, preventing
the cytoplasm from becoming sufficiently acidic to dissolve bone in the first place
(Am. J. Path. 164: 1537, 2004) In the severe, autosomal-recessive variant, the skull becomes so deformed from the disease itself and
the extramedullary hematopoiesis that the foramina for the optic and other cranial nerves are
compromised. Radiologists note a striking resemblance between skull x-rays of these kids and the
"Alien" from the Sigourney Weaver space thrillers (Radiology 183: 129, 1992).
As you would expect, the problem seems to be with the osteoclasts. If you get a chance to examine
these, they are likely to appear bizarre.
Marrow transplantation cures the underlying lesion: Blood 97: 1947, 2001.
"Osteopetrosis tarda" is a forme fruste, usually a subclinical x-ray finding
in older folks (Am. Fam. Phys. 57: 1293, 1998), and there is talk of
retroviruses causing sporadic cases by destroying osteoclasts.
ACHONDROPLASIA
The achondroplasia locus is the receptor for fibroblast growth factor 3.
* The mutation is usually the same, a substitution: Nat. Gen. 13: 233, 1996. Other, worse alleles here give
thanatophoric dwarfism, with excessively short ribs and suffocation shortly after birth (update Am. J. Path. 161: 1325, 2002).
Rat model
Nature Genetics 12: 390, 1996. Some short people have a forme fruste ("hypochondroplasia")
with mutated FGF3 (J. Ped. 133: 5, 1998). Sun Hudson,
the baby in the 2005 Texas
"life support" case, suffered from thanatophoric dwarfism.
* Advanced paternal age is one of the known risk factors for new mutations.
Apparently this mutation, and maybe the similar Apert's mutation (see below)
give a growth advantage to the sperm clone (Science 301: 606 & 643, 2003).
{25610} achondroplasia
Several of history's best-loved entertainers were achondroplastic dwarves (legendary gladiators, the
Egyptian good-luck spirit Bes, Pharaoh Pepi's Nubian dancer, Tom Thumb and his wife, the great
Renaissance fiction-writer Morgante. The "Munchkins" from the movie
version of "The Wizard of Oz" were apparently
a mix of pituitary and achondroplastic
dwarves. Some people
say that Aesop was a black
achondroplastic dwarf).
The traditional teaching is that
dachshund dogs are achondroplastics; we now know that the FGF3 genes seem
to be normal, and the gene(s) for the short legs of dachshunds, basset
hounds, and bulldogs remains unknown (Can. J. Vet. Res. 64: 243, 2000).
In fact, achondroplasia has a mystique, and has even been considered a desirable trait. See Clin.
Genet. 37: 279, 1990. Everyone's heard of the "Little People"'s organizations, and there is much
friendly rivalry between achondroplastic and pituitary dwarves as to "which is better", etc.,
etc.
There are several other dwarfism syndromes that result from defective bone growth. Those that
compromise the lengthening of the ribs are fatal shortly after birth (why?)
* Apert's (deformed face, syndactyly) is mutated fibroblast growth factor receptor 2 (Nat. Genet. 13:
48, 1996); documentary "Mary Ann" about an Apert's baby who was so ugly that everybody
assumed she was retarded, too, and they put her in a home for retarded kids; she wasn't retarded.
Apert's is usually a new mutation, and almost always on Dad's chromosome (Nat. Genet. 13: 9,
1996); this is another of the few genetic diseases that gets more common with advanced paternal age.
A milder allele causes Crouzon syndrome; the same advanced paternal age effect
has been noted (Am. J. Hum. Genet. 66: 768, 2000).
One of the "pseudoachondroplasia" diseases
results from a mutated cartilage matrix protein,
which is improperly processed and causes apoptosis of the growth cartilage
(Am. J. Path. 163:
101, 2003).
* A "midget" is a normally-proportioned miniature adult; a
"dwarf" is short because of disproportion.
{53757} Apert's
* PYCNODYSOSTOSIS
* OTHER GENETIC SYNDROMES
Camurati-Engelmann disease, or "progressive diaphyseal dysplasia",
features bone laid down under the periosteum; the gene is TGF-β1
(Nat. Genet. 26: 273, 2000;
J. Biol. Chem. 278: 7718, 2003).
PYOGENIC OSTEOMYELITIS
Common bacteria can reach the bone via the blood, during surgical or other trauma, or from
surrounding tissues (don't forget infected teeth, or the gangrenous feet of diabetics).
Osteomyelitis is especially serious, since the rise in pressure caused by the suppuration (like in a ripe
pimple, of course) is often enough to cause infarction of spongy bone and marrow, sequestering
the infection and turning it into a chronic infection refractory to all but the most aggressive
treatment.
The usual bug is staph, though most of the common bacteria can produce osteomyelitis. In sicklers,
salmonella is the usual culprit, and drug abusers who mix their works with tap water are prone to
pseudomonas. In 50% or so of cases, you'll grow nothing, probably because
somebody gave an antibiotic already.
The anatomic pathology of pyogenic osteomyelitis has many variants. Rupture through the cortex
can produce periostitis or (in a growing child) subperiosteal abscess surrounding the entire shaft.
Dead bone becomes a sequestrum (and acts like any other foreign body), while new living
bone that grows around the dead bone
is called the involucrum. Rupture through the skin produces refractory sinuses, where
squamous skin cancer is likely to arise because of the ongoing destruction-and-regeneration
of the squamous epithelium. A walled-off area full of bacteria is a Brodie's abscess,
which can keep the infection going, and perhaps spreading via the bloodstream, for many years.
In the chronic infection, the infiltrate is a mix of neutrohpils,
lymphocytes, plasma cells, and lipid-laden macrophages; sometimes the plasma cells or
macrophage are by far the most abundant.
Healed osteomyelitis is often very radio-dense.
Remember that osteomyelitis is likely to complicate bedsores and foot gangrene.
Osteomyelitis often becomes a clinician and patient's nightmare. You're already familiar with
amyloidosis A, one of the many feared outcomes.
* When there is an open wound that is being managed, pathologists are now being
asked to examine a bone biopsy to see whether osteomyelitis is present. This guides
antibiotic therapy (Am. J. Med. Sci. 321: 367, 2001).
Autopsy series of osteomyelitis in sacral decubiti: Arch. Path. Lab. Med. 127: 1599, 2003.
{05293} osteomyelitis, x-ray (see it? areas of dead bone often end up mottled-radiodense)
TUBERCULOUS OSTEOMYELITIS
This used to be common everywhere and is still common in the poor nations. While the onset is
more insidious than pyogenic osteomyelitis, the infection is extremely destructive and hard to treat.
Pott's disease is the dread tuberculosis of the spine, and TB is the common cause of the infamous
psoas abscess.
* Literature buffs: Elizabeth Barrett Browning ("Sonnets from the Portuguese", etc.) was completely
disabled by severe chronic pain from Pott's disease for over a decade. When she was given free
access to morphine, she became a productive writer and much happier person. Despite ideology,
there may be a lesson here.
OSTEOPOROSIS (Ann. Int. Med. 126: 458, 1997; Med. Clin. N.A> 87: 1039, 2003)
This is a very important process results from a slight excess of bone resorption over bone deposition,
continuing over many years. As we get older, we all get some osteoporosis.
The histology is banal (thin cortex, thin trabeculae), and the radiology equally so (there are
parameters on hand x-ray, and so forth). These belie the devastating consequences, which include
pathologic fractures (hip, compression fractures of vertebrae causing "dowager's hump" kyphosis),
and chronic pain. Osteoporosis causes 1.2 million fractures per year in the U.S. alone.
In a man, or a pre-menopausal woman, look for one of the known "causes" of "secondary
osteoporosis" (Arch. Int. Med. 149: 1069, 1989). These include, but are not limited to:
The best-known gene is
the vitamin D3 receptor (* Flk-1 gene product) that appear to account for 75% of the variation in
early adult bone density (which in turn is the major predictor of future primary osteoporosis).
Definitely watch this (Nature 367: 576, 1994; Lancet 345: 423, 1995).
Although in "pure" osteoporosis, labs will be normal, it's probably worth
spending $75 to get each of these people a serum TSH (if on thyroid replacement), serum calcium,
serum PTH, serum 25(0H)vitamin D, CBC, chem profile,
and 24 hour urine calcium (J. Clin. Endo. Metab. 87: J. Clin. Endo. Metab. 87:
4431, 2002.
X-rays will be normal until about half of the bone is gone.
Today, "proven" ways of slowing osteoporosis include estrogen replacement (after menopause,
whether natural or artificial, see Am. Fam. Phys. 40: 205, 1989) and calcitonin (J. Ped. 118: 703,
1991). Nowadays, androgens and diphosphonate are also pretty much standard (South. Med. J. 87:
S-23, 1994). Heavy calcium intake (popular with the Tums manufacturers, of course) remains
"unproven".
* Paradoxically, the amino-terminal end of parathyroid hormone
increases the formation and total mass of bone, and this is now
finding clinical use: NEJM 344: 434, 2001.
{46507} osteoporosis, gross
Egyptian mummy ladies had less osteoporosis for their ages than our ladies do; perhaps they were
more active physically than American folks today (Lancet 341: 673, 1993, no television).
OSTEOMALACIA
Failure of the bone to mineralize properly in an adult. We've already studied this under "rickets".
Adults with dietary calcium deficiency (poverty, elderly "tea and toast" eaters,
people subsisting mostly
on vegetables) or malabsorption are prone to osteomalacia, which in turn results in bone pain and
even fractures.
It's a component of renal osteodystrophy
* It's also the lesion
seen in paraneoplastic renal phosphate wasting
(NEJM 348: 1656 & 1705, 2003; "oncogenic osteomalacia", from tumor-produced
which you'll recognize
by the bone pain and the remarkably low serum phosphate levels; patients have sarcomas that
may be small, low-grade lesions
including the infamous "phosphaturic mesenchymal tumor": Arch. Path. Lab. Med. 126:
1245, 2002).
The truth is that adult vitamin D deficiency is rampant in our "civilized" society,
and accounts for many of your patients with persistent, nonspecific musculoskeletal pain
(Mayo Clin. Proc. 78: 1463, 2003). Even people "who are not at risk"
turn up with it, and curiously, the "complementary medicine community"
seems to be paying this very little attention. Before your write your "total body pain"
patient off as "having fibromyalgia" or "being mental", check vitamin D levels.
* A study out of New Zealand (J. Am. Diet. Assoc. 104: 250, 2004)
followed 50 children who had avoided drinking cow's milk for a long time
and did not use calcium-rich supplements (i.e., the vegan or faddist
parents didn't know what they were doing).
They had almost three times as many fractures as other kids, most often
following trivial injury. This does not surprise me at all.
* Hypophosphatasia, an inborn error that causes osteomalacia of
variable severity, is caused by mutations (recessive or a dominant poison-protein)
of alkaline phosphatase (J. Clin. Endo. Metab. 85: 743, 2000).
OSTEITIS FIBROSA CYSTICA and RENAL OSTEODYSTROPHY
Review these in "Big Robbins" if you need to do so. Remember that osteoclasts in
normal adult bone
are rare -- if you see even one osteoclast
in a random slide of adult bone, think of hyperparathyroidism from some cause.
Look for the cutting cones going through the centers of the trabeculae of spongy bone.
Renal osteodystrophy includes lesions of hypovitaminosis D, osteomalacia,
and hyperparathyroidism.
{46509} osteomalacia, thick unmineralized osteoid seams
* FLUOROSIS
Nerve compression and increased radio-opacity are typical. You may see the
disease if you visit certain parts of Ethiopia or India. Everybody in a particular
town will have it.
PAGET'S OSTEITIS DEFORMANS (Am. Fam. Phys. 65: 2069, 2002)
A common, usually-subclinical process seen in maybe 3% of older people, in which portions of one
or more bones become involved in abnormally rapid production and destruction of osteoid, leading
to curious, abnormally-vascular, abnormally-brittle bone that tends to deform along lines of stress.
Most often involved are the pelvis (usually quiet), femurs (bowing of the legs), humerus (usually
quiet), spine (be careful) and/or skull. The forehead can grow larger ("leontiasis ossea").
The bone thickens and will feel warm because of
hyperperfusion. Patients may experience bowing of the legs, bone pain (usually mild) and increased
hat size. Deafness can result from impingement on the VIII nerve's foramina and/or disease of the
ossicles. Even more ominous are the (uncommon) development of high-output heart failure and/or a
vicious osteogenic sarcoma (or other bone cancer; fortunately only about 1% of patients develop
this; Cancer 70: 2802, 1992) and/or compression of the brain at the foramen magnum.
The microscopic picture is distinctive. Osteoblasts and osteoclasts
are both increased. Osteoclasts may be gigantic, with
100 or more nuclei.
The trabeculae are thick, made of woven bone, and shaped
weirdly, with a mosaic pattern of seams ("geographic bone"; "crazy quilt"). The marrow space is
replaced by highly vascular fibrous tissue. A ghoulist but helpful
autopsy-table observation: Everybody seems to know that the
calvarium of a Paget's skull doesn't hold water.
Most pathologists think that Paget's is a slow-virus infection, and one current suspect is canine
distemper virus (Bone 23: 171, 1998). More than one virus may
be able to cause the disease; measles and RSV are also suspects.
* Measles virus with a trademark mutation within
osteoclast precursors in 4 of 6 Paget-disease men (J. Clin. End. Metab. 80: 2108, 1995;
J. Bone Min. Res. 17: 145, 2002).
This remains unconfirmed.
Putting together what we know about the etiology of Paget's: J. Clin. Inv. 115:
200, 2005. The fundamental lesion is that osteoclast precursors are too sensitive
to factors that transform them into osteoclasts. At the beginning, the process
is entirely lytic, but soon the osteoblasts, which remain coupled, catch up.
The fact that Paget's is
localized makes the idea of a virus even more inviting.
It is likely that Beethoven's deafness was due to Paget's. (Why do we think so? Hint: Note the
shape of his head, and read up on his later-life health problems.)
* Egil the Viking, who acquired a hideously deformed, massive face and head, and whose skull
survived a blow from an axe from another Viking (who knew how to use axes),
probably had Paget's, which was common (Sci.
Am. 272(1): 82, 1995). Great pictures.
* "Familial Paget's" features a similar histology and a mutated
osteoprotegerin, one of the TNF-receptor family (NEJM 347:
175 & 210, 2002). Two more: Arth. Rheum. 50: 1650, 2004.
The treatment of Paget's has been revolutionized by the introduction of the bisphosphonates,
osteoclast inhibitors (Br. Med. J. 312: 454, 1996; Hosp. Pract. 32(3): 63, March 15, 1997).
Don't confuse "Paget's disease of bone" with "Paget's disease of the nipple" or "Paget's disease of the
skin". Both result from growth of underlying adenocarcinomas into the epidermis.
{13384} Paget's disease, skull, gross
FIBROUS DYSPLASIA
In this condition, a portion of bone when the spongy trabeculae should be is replaced by fibrous
tissue in which poorly-formed spicules of woven bone are abundant. Simple fibrous dysplasia can
be monostotic or polyostotic.
Monostotic fibrous dysplasia is usually asymptomatic, a radiologist's curiosity.
Often one side of the jaw is involved, producing a distinctive asymmetry of the lower face.
Involvement of the shoulders and hips can produce disability. (* Ask a radiologist to show you the
"shepherd's crook" deformity of the proximal femur.)
McCune-Albright polyostotic fibrous dysplasia is a curious disease also featuring café-au-lait spots
(irregular borders, in contrast to those of neurofibromatosis), precocious puberty, and often other
endocrine dysfunctions (notably hyperthyroidism, cushingism, acromegaly, and/or vitamin D
resistance). It looks like a genetic disease, but isn't inherited in any familiar fashion.
The defect is in the gene that codes for the 5α-subunit (GNAS-1) of the G-protein (i.e., the one
that operates from the cyclic-GMP/ras system) that is in charge of stimulating adenyl cyclase. This
means that when a cell is given a signal via cyclic-GMP, it responds as if it had been stimulated by
cyclic-AMP. This probably accounts for the endocrinopathies, but what about the spots?
It turns out these patients are all mosaics for affected and normal cells, and that only the places
where the cells bear the mutation are affected. (Even one dose of the McCune-Albright must be
lethal to the fertilized egg; the mutation is post-zygotic and clones of cells bearing the mutation are
distributed segmentally throughout the body and must go back to the not-very-many-cells stage.
Ask an embryologist.)
* How it was worked out: NEJM 325: 1688, 1991. There's also a
number of alleles at the same locus ("Albright's hereditary osteodystrophy") that can be inherited;
you remember this as "pseudohypoparathyroidism" and "pseudo-pseudohypoparathyroidism": J.
Clin. End. Metab. 76: 1560, 1993.
Regardless of etiology, the common problem in fibrous dysplasia seems to be activation of adenylate
cyclase, leading to * c-fos overexpression, etc., etc. NEJM 332: 1546, 1995.
Transformation of fibrous dysplasia to cancer is rare.
While we're on the subject of scrambled bone growth: An aneurysmal bone cyst is a
rapidly-expanding lesion with wide blood vessels. There may or may not be bone and/or giant cells.
These seem to expand a bone just like an aneurysm expands a blood vessel ("blowout expansion");
curiously, these can also "spread" across a joint.
Sometimes an "aneurysmal bone cyst" can be the first sign of some other
underlying tumor. HYPERTROPHIC OSTEOARTHROPATHY
Mysterious periosteal new bone formation at the distal ends of tubular bones
throughout the body, with arthritis.
* Usually these patients also have clubbing, which
probably reflects megakaryocyte embolization in most cases. However,
something else is perhaps going on in hypertrophic osteoarthropathy.
Most of these patients have an underlying
non-oat-cell
bronchogenic carcinoma or cystic fibrosis. (Other notable causes of
clubbing, most especially right-to-left cardiac shunts, SBE, and Crohn's disease,
usually don't
cause the hypertrophic osteoarthropathy). Some cases are "primary", idiopathic,
progressing over decades.
This can be very painful and crippling, and require special treatment
(drugs, radiation). * Pamidronate in cystic fibrosis: Chest 121: 1363, 2002.
INTRODUCTION TO BONE TUMORS
Primary tumors of bone by definition arise from the mesenchymal cells (as opposed to the marrow
elements, plasma cells, and so forth). There are only about 2000 new cases yearly in the U.S., but
they are especially troublesome.
The common primary bone cancers (as opposed to metastatic and hematopoietic cancers including myeloma) are osteosarcoma
(most common), Ewing's sarcoma, chondrosarcoma, and malignant giant cell tumor.
Where do bone tumors arise?
Diaphysis: enchondromas; some chondrosarcomas; Ewing's, and eosinophilic granulomas
Epiphysis: chondroblastomas; most giant cell tumors (supposedly)
Metaphysis: all other primary bone tumors (why? because this is where a tumor
arising from the growth plate will appear)
(Osteomas arise from the cortical bone of the face. Plasma cell myeloma produces its "punched-out"
lesions throughout bone.)
Most patients with primary bone cancer are young. While any primary bone tumor can occur in a
child or adolescent, remember these general ranges:
Metastatic neuroblastoma: infants and toddlers
Ewing's sarcoma: older children and adolescents
Osteosarcoma: adolescents and young adults
Giant cell tumors: young adults and middle age
Chondrosarcoma: middle age
Metastatic cancer: middle and old age
Cancers present with pain, swelling, or a fracture. Benign tumors, if symptomatic at all, usually
present as a painless mass. (Osteoid osteomas are painful, enchondromas may cause a stress
fracture, and other benign tumors can sometimes do these things.)
The more aggressive cancers look like other cancers, and there is usually destruction of surrounding
bone.
Radiologists suspect cancer whenever a tumor lifts up the periosteum. You can tell because this
results in new bone formation (Codman's triangle; "sunburst" deeper in the bone).
Risk factors for bone sarcoma include some familial syndromes, radiation and chemotherapy
Cancer 67: 193, 1991). However, most cases occur without any of these.
In the previously irradiated patient, the commonest primary bone cancers:
Tall kids get more Ewing's sarcomas and osteosarcomas.
Most bone tumors are slightly more common in males than in females. Chondrosarcomas in
particular are a man's disease (3:1).
Making the diagnosis of a primary bone tumor poses special problems.
The pathologist will always want to see the x-rays before making the diagnosis. (Lytic or blastic?
What sort of edge? Reaction in surrounding bone?)
Most cases will go for consultation. (Few community pathologists have much experience with these
things. The tumors mostly look very similar anyway. It is easy to miss the tumor on biopsy. The
patients are kids. The treatment is horrible. What if she is pregnant?)
* Biopsying these tumors: Clin. Orthp. Rel. Res. 368:
212, 1999. Fine needle aspiration of bone: Clin. Orthop. Rel. Res. 373:
80, 2000; Cancer 90: 47, 2000, Am. J. Clin. Path.
111: 632, 1999; Am. J. Clin. Path. 115: 59, 2001. White knuckles.
Treatment for bone tumors is much better than in the old days.
Benign tumors may be treated by curettage and packing with bone chips from elsewhere.
Malignant tumors require resection, radiation, and/or chemotherapy.
If treated conservatively, the common cancers tend to recur in more malignant form. (Ewing's
sarcoma is the exception, for it is ultra-malignant from the onset.)
BONE-FORMING TUMORS
Osteoma: a lump of ordinary, dense bone jutting off a skull bone. A non-tumor; if multiple,
think of Gardner's.
Usually harmless, they may impinge on the brain, obstruct sinus drainage, or look ugly.
If multiple, suspect Gardner's disease (intestinal polyps, soft tissue sarcomas,
desmoids, epidermoid cysts).
{05842} exostosis ("osteochondroma")
Osteoid osteoma: a common benign tumor of osteoblasts.
A nidus of miniature bony trabeculae and fibrous tissue,
surrounded by very dense bone.
Occurs in the vertebrae or long bones of young adults, where it causes well-localized pain and
tenderness. The pain responds dramatically to aspirin (i.e., it must be
mediated by the very large amounts of prostaglandin E2 in these
lesions; Clin. Ortho. Rel. Res. 393: 258, 2001),
and the rim is also very heavily innervated
(Mod. Path. 11: 175, 1998).
Enucleation is curative. The patient will tell you
in the recovery room whether you got it all out.
{10830} osteoid osteoma, histology
* Osteoblastoma ("giant osteoid osteoma"): a rare non-metastasizing tumor of osteoblasts
This usually arises in the vertebral bodies of young adults.
The tumor cells make new osteoid. All osteoblastomas are by definition larger
than 1.5 cm.
Cells in the center can look nasty, but they appear to "mature" at periphery.
Osteosarcoma: the commonest primary cancer of bone (not counting
plasma cell myeloma of course). Cancer of the osteoblasts.
Review in kids: Ped. Clin. NA 44: 973, 1997.
By definition, any and all tumors in which malignant cells
themselves directly
make osteoid are osteosarcomas.
(By contrast, benign endochondral bone formation can take place in any cartilaginous tumor.
Remember also that normal bone surrounding any diseased area may show proliferative changes.)
It is also called "osteogenic sarcoma", an ambiguous term * which used to mean any sarcoma arising
from bone.
Most arise in the long bones (especially the knee; occasionally in the jaw or elsewhere; sometimes
not even in bone: Cancer 65: 2762, 1990).
As noted, most patients are adolescents or young adults, and there is a slight male preponderance.
(Of course, many teenaged males have a painful knee, hence the delays in making the diagnosis.)
People in retinoblastoma families are at much greater risk, and deletions of the Rb anti-oncogene on
long arm of chromosome 13 are the rule in osteosarcomas. Li-Fraumeni (p53) families are also at
great risk, and one writer recommends screening all families of osteosarcoma patients (J. Bone Joint.
Surg. 74: 883, 1992).
"Secondary" osteosarcomas occur in old people with Paget's disease (especially in the pelvis), or
patients of any age with familial conditions with many osteochondromas and/or enchondromas. The
prognosis for these tumors is poor.
Other "secondary" osteosarcomas follow radiation, chemotherapy, chronic osteomyelitis, bone
infarcts (caisson workers).
Osteogenic sarcomas present variable histopathology.
Tumors may be predominantly made of new bone, cartilage, fibrous tissue, or even vessels
("telangiectatic osteosarcoma", a vicious variant) or small cells.
Grading of osteosarcomas has not proved very helpful for prognosticating
outcome, but there are two subtypes with a generally good prognosis.
Periosteal osteosarcoma: a ring of mildly malignant, calcifying cartilage-and-new-bone around a bone in a young
person. It may occur remote from bone: Arch. Path. Lab. Med. 115: 906,
1991.
Parosteal ("juxtacortical") sarcoma: dense bone or "callus" at the distal femur.
These carry a good prognosis, unless there is de-differentiation (at presentation
or later) into a more aggressive sarcoma (Cancer 103: 2373, 2005).
Once almost always fatal, the five-year survival in osteogenic sarcomas treated today is running
around 50-60%, though it is not altogether clear what is causing the improvement.
{05755} osteosarcoma, x-ray
CHONDROMATOUS TUMORS (remember cartilage often undergoes dystrophic calcification)
Exostosis ("osteochondroma", "ecchondroma"): "the commonest bone tumor", actually a hamartoma
A cap of normal cartilage on a bony stalk. These grow up over time.
An incidental finding, with a slight potential for transformation into chondrosarcoma,
especially if multiple (Gardner's, or the familial exostosis syndromes).
* The gene EXT1 is known, and governs surface expression of heparan sulfate.
(Nat. Genet. 19:
158, 1998).
EXT2 has also been discovered
(Am. J. Hum. Genet. 62: 346, 1998). Both are probably
tumor suppressor genes.
This is the bone tumor that is best-linked to previous trauma.
(En-)chondroma: a common oddity; a popcorn-shaped lump of cartilage inside the shaft of a bone
Most often involves the proximal phalanges. It is an incidental finding on bone scan or x-ray, or is
discovered when a child or athlete presents with a stress fracture.
Usually enchondromas are harmless. If multiple (Ollier's, Maffucci's with
hemangiomas) or in large bones, there is about a 25% chance that
at least one will
transform into
chondrosarcoma. These must be anti-oncogene deletion syndromes.
Ollier's is usually unilateral (i.e., post-zygotic mutation);
there is a distinct bilateral hands-and-feet-only variant (J. Ped. Ortho. 6: 15, 1997).
Malignant transformation: Hum. Path. 31: 1299, 2000.
* Fibromyxoid chondroma ("chondromyxoid fibroma"): a rare, benign spindle-cell tumor that
differentiates as cartilage but without a tre hyaline cartilage matrix.
Occurs in the legs of young adults.
This one gives pathologists extra trouble, and it is often mistaken for chondrosarcoma.
* Chondroblastoma: a rare, benign tumor of cartilage
Occurs in the legs of young people.
Most are very cellular and tend to focal calcifications, and there may be a few mitoses.
They cannot
always be distinguished from chondrosarcomas.
Chondrosarcoma: the second commonest bone tumor (not counting
plasma cell myeloma); sarcoma of cartilage, with a true hyaline-cartilage matrix
Primary chondrosarcoma arises most often in the pelvis in middle-aged men.
Prognosis depends on the grade:
* Grade I: mild cellular atypia (plump nuclei, pale nuclei, binucleate cells, two cells in a lacune,
mitoses; even encasing a bone spicule on all sides helps distinguish it from an
enchondroma)
* Grade II: crowded cells, perhaps a few bizarre cells
* Grade III: nasty-looking (includes "mesenchymal chondrosarcoma")
Only the Grade III lesions are likely to metastasize,
but when the lower-grade lesions recur locally,
the grade may be higher.
{05958} chondrosarcoma, gross
TUMORS OF UNCERTAIN ORIGIN
Ewing's Sarcoma: an extremely malignant tumor of uncertain histogenesis.
Review Ped. Clin. NA 44: 991, 1997.
Almost all patients are of European ancestry.
The tumor is painful and at presentation otherwise simulates osteomyelitis.
It arises in any bone, packs the nearby marrow, disseminates widely and rapidly, and is the one bone
tumor that metastasizes readily to other bones (see for example Radiology 175: 233, 1990.
It is composed of sheets of "small blue cells" with little cytoplasm (i.e.,
almost all nucleus, hence "blue"-staining), and this is usually loaded with
glycogen. There is no stroma or reticulin between its large vessels, and the tumor is a viscous liquid,
like pus. There are mitoses, necrosis, etc.
Future radiologists: Instead of elevating the periosteum as "Codman's
triangle", the rapid growth through the cortex produces layers of calcification
("onion skinning").
* A closely-related tumor, the slightly more ominous "malignant peripheral neuroectodermal tumor",
must be distinguished from classic Ewing's sarcoma. If it makes actual Homer-Wright rosettes and/or
makes at least two neural markers, it's one of these instead. For a comparison see Arch. Path. Lab.
Med. 118: 608, 1994.
The cell of origin might be primitive mesenchyme without further differentiation
or "primitive
neuroectoderm" (perhaps the first mesoderm where it buds off the ectoderm; immunostaining; see
Am. J. Path. 135: 847, 1989). This is pretty much academic.
If caught early, the prognosis after radiation and chemotherapy is good, with 85% 5-year survival.
If it spreads, chances for a cure drop to 20%.
Today's pathologists help clinicians plan therapy by seeking the
gene that causes Ewing's (and its kin) in the peripheral tissues.
The chromosomal abnormality t(11;22); the fusion product antigen
is EWS/FLI1.
Molecules: Am. J. Path.
156: 849, 2000.
Today it is routine to look for this in marrow, even if
the disease seems localized (Cancer 100: 1053, 2004).
Most pathologists distinguish Ewing's from "primitive neurectodermal tumor"
that looks the same histologically. Both have the famous (11;22) translocation.
PNET will have neural markers (neuron-specific enolase,
chromogranin, synaptophysin, S-100, Homer-Wright rosettes)
that you'd expect in a neuroblastoma as well as CD99/013 that you'd expect in Ewing's.
Pathologists also help prognosticate these tumors (as we do osteosarcomas)
by defining how extensive necrosis is following preoperative chemotherapy.
{49496} Ewing's sarcoma, resection specimen
Giant cell tumor ("osteoclastoma"): benign or malignant, a common spindle-cell tumor packed with
non-neoplastic osteoclasts bearing many nuclei.
Arise in the long bones, usually in young adults.
The tumor is mesenchymally derived,
and the actual neoplastic cells are covered with abundant
RANKL, causing
local non-neoplastic cells to transform into very large osteoclasts (Am. J. Clin. Path.
117: 210, 2002). Since it is loaded with osteoclasts, these tumors are
entirely lytic, and you will probably see no new reactive bone formation.
Half are clinically and histologically benign, one quarter are clinically and histologically malignant,
and one quarter are histologically benign but clinically malignant.
* Future pathologists: Telling these from the brown tumors of hyperparathyroidism
is a challenge. Real giant-cell tumors have fewer spindle cells, less clustering
of giant cells, and less fibrosis.
* "Malignant giant cell tumor of bone" may may any of three things (Cancer 97: 2520, 2003):
Future pathologists: the histopathology closely resembles hyperparathyroidism or * certain
"reparative granulomas" of the facial bones.
Also remember any tumor of bone may sometimes be loaded with giant cells.
Non-ossifying fibromas ("fibrous cortical defects")
Little hamartomas in the long leg bones of children and teens.
They are made of fibroblasts, stroma, and
(often) lipid-laden macrophages. If you look, you'll find them in 1/3 of all normal kids. They rarely
cause problems, and they go away by themselves.
Malignant fibrous histiocytoma of bone (Cancer 79: 482, 1997)
is the other important bone tumor, around 1/10 as common
as osteogenic sarcoma.
Leave the diagnosis of this many-faced tumor to the pathologists.
{21123} malignant fibrous histiocytoma, trust me
Chordoma: a rare, locally destructive tumor that arises from the notochord
These arise in the sacral and spheno-occipital areas at any age.
Histology shows myxoid intercellular areas with "physaliphorous" (bubbly) cells.
Pathology update: Cancer 98: 1934, 2003.
Though they are only "low-grade" lesions and seldom metastasize,
the prognosis is generally not good just
because of the location. Today's ultra-modern surgery and radiotherapy
are producing some likely cures.
METASTASES TO BONE
By far the commonest "bone cancer" if you want to consider it to be such, presenting as pain or a fracture.
The tumors that most commonly metastasize to bone are carcinomas of the lung, breast, prostate,
kidney, and thyroid.
Most commonly the vertebral bodies are involved; the distal extremities are usually spared.
"Blastic" and "lytic" lesions are distinguished. (Any primary can produce either type; prostate
metastases are the most likely to be blastic.)
Repair of damaged bone by osteoblasts is responsible for the positive scan and elevated alkaline
phosphatase.
REMEMBER: Plasma cell myeloma, malignant lymphoma (Cancer 73: 1194, 1994), and
eosinophilic granuloma are other important causes of "bone tumors".
* Bones are a perennial symbol of human mortality, and in a larger sense, of all of human biology.
"Bone of my bone..." -- Adam. "Cursed be he who moves my bones" -- Shakespeare's epitaph.
"Them bones, them bones gonna rise..." -- Afro-American Spiritual. As a kid, I was much affected
by Yeats's ghost story The
Dreaming of the Bones, about the need for forgiveness and love ("Isn't
it time we forgave the English?"); recommended reading in any era of political hatred.
SOFT TISSUE TUMORS AND QUASI-TUMORS
A plethora of benign and malignant tumors arise from the connective tissue of the support structures
of the body. As usual, the cells normally present in a tissue determine the possible cells of origin of
tumors.
Most of these "just happen", and the cause is seldom clear.
There are a few genetic syndromes that we'll study elsewhere. Sarcomas that present a monotonous appearance have, as a rule, at least one
trademark translocation (Am. J. Surg. Path. 26: 965, 2002; assays Lab. Invest. 81:
905, 2001). Those that are very pleomorphic do not, but have instead
very elongated telomeres (Am. J. Path. 164: 1523, 2004).
For soft-tissue cancers, grade and stage are both important in determining prognosis. For now, you
may leave both of these determinations up to senior physicians.
As a rule, the more superficial the tumor in the body, the better the prognosis.
Surgery is often more limited for these tumors than for malignancies elsewhere (i.e., you can cut out
a lung clean and easy, but not half of somebody's back.) One mark of malignancy, then, is local
recurrence.
These tumors intrigue pathologists, and we love to subclassify them; today's gene-profilers
are finding patterns distinctive for the familiar entities, as you'd expect (Am. J. Path. 163: 691, 2003). Your instructor thinks it is
inappropriate for you to spend too much time studying all the differences among these tumors.
Here's what's worth knowing about the common ones.
Granular cell tumors (mostly benign)
Tumors of schwann cell origin (* S100-positive), made of polyhedral, dPAS-positive
phagolysosomes.
This tumor is notable for inducing hyperplasia in overlying stratified squamous epithelium. (This
"pseudoepitheliomatous hyperplasia" can look much more disturbing than the tumor itself.)
These were formerly misnamed "myoblastomas" for no obvious reason.
Benign fibrous histiocytoma
A tumor of cells usually showing a mix of features of fibroblasts (spindle cells, collagen production)
and macrophages (* positive for α1-PI, lysozyme, factor XIIIa, etc.)
The most familiar benign fibrous histiocytoma is the banal dermatofibroma, a hard knot in the
dermis with pigmentation of the overlying epidermis. More about this under "Skin".
Malignant fibrous histiocytoma ("MFH")
The malignant counterpart of the above, and the most common soft-tissue sarcoma. Five-year
survival is around 50%.
There will always be some areas with genuinely wicked looking nuclei.
You can read yourself about the subtypes. The "storiform" pattern is cartwheel, like ovarian stroma.
The "myxoid" pattern simply generates lots of ground substance. The "inflammatory" pattern is
chemotactic for polys (betcha it makes interleukin 8). "Dermatofibrosarcoma protuberans" is a
cartwheel variant with little malignant potential and a trademark translocation. Etc., etc.
{21146} malignant fibrous histiocytoma, gross (trust me on this and the following MFH's)
Cellulite
The histopathology is thinning of the dermis (perhaps from pressure
of increasing adiposity) and especially thickening
of the fibrous bands of the subcutaneous panniculus where the
edges of the "cellulite" form dimples. ("Scar contracts.")
See Am. J. Dermpath 22:
34, 2000; Plast. Recon. Surg. 103: 1934, 1998.
All recent controlled studies of non-surgical cellulite remedies have failed
to show any effect.
Lipomas
Benign tumors of fat, the most frequent soft-tissue tumor. Typically, a thinly-encapsulated bump of
subcutaneous fat that doesn't grow or regress with the rest of the fat.
{05810} lipoma, gross
* Most lipomas, and their benign and malignant variants, have chromosomal abnormalities involving
12q14. The genetic mutation in patients with multiple lipomas, however,
is in the mitochondria (J. Am. Acad. Derm. 44: 132, 2001).
Hibernoma ("brown fat lipoma") is a tumor of brown (primitive, mitochondrion-rich, several lipid
droplets per cell) fat. The term "hibernoma" comes from the role of brown fat in generating heat to
wake bears from hibernation. * Possible link with mutated mitochondrial
DNA: Am. J. Hum. Genet. 52: 551, 1993.
{46354} hibernoma, histology
* In adiposis dolorosa ("Dercum's disease"), which may be an anti-oncogene deletion syndrome or
mitochondrial mutation syndrome, the
patient has hundreds of lipomas that may hurt.
Whatever the cause, it remains remarkably elusive.
William Osler called this one of the three worst diseases of his time (with subluxation of the
sacroiliac joint and milk leg). Today we're treating it with liposuction (Ann. Plast. Surg. 33: 664, 1994).
At least in adiposis dolorosa (and we may conjecture, in other lipomas), the fat isn't burned very well
for energy (Clin. Sci. 81: 793, 1991).
* Angiolipomas, in contrast to generic lipomas, are often multiple and often painful. The presumed
anti-oncogene has not yet been identified (Arch. Path. 123: 946, 1999).
* "Lipoma of the spermatic cord" is a chunk of non-neoplastic fat in a man's inguinal hernia sac.
* Myelolipoma is a bone marrow choristoma in or near the adrenal glands (review and case Arch.
Path. Lab. Med. 118: 188, 1994).
{25412} adrenal myelolipoma
Angiomyolipomas are the familiar tumors which, when present in the kidney, raise the specter of
tuberous sclerosis.
Neither lipomas nor liposarcomas have any know relationship to obesity.
Liposarcoma ("liposarc")
"Cancer of the fat", though capable of arising wherever there are blood vessels (which give rise to fat
in the baby). They usually arise deep in the body, especially in the retroperitoneum.
* Distinctive for liposarcomas
is the presence
of at least a few lipoblasts. These are mesenchymal cells with fat droplets
that scallop the nuclei.
You don't see these in healthy tissue, even in
embryonic or fetal fat.
"Well-differentiated liposarcomas" show only slight atypia and maybe metaplasia into some other
kind of connective tissue. Prognosis depends on location. Retroperitoneum and groin are bad,
extremities is good. Review: Am. J. Surg. Path. 16: 1051, 1992.
* "Myxoid liposarcomas" look grossly like raw fish fillets. They feature a plexiform pattern of
vessels in a myxoid background with little lipoblasts. * "Round cell liposarcomas" usually look initially like lymphomas, except that the cells contain fat
vacuoles.
"Pleomorphic liposarcomas" blend into totally anaplastic sarcomas. The give-away is huge, ugly
cancer cells loaded with fat vacuoles.
{05804} liposarcoma, gross
Rhabdomyoma
Very, very rare. Most "rhabdomyomas" you'll see are the cardiac hamartomas typical of tuberous
sclerosis. * A pediatric rhabdomyoma type: Arch. Path. Lab. Med. 117: 43, 1993.
Rhabdomyosarcoma ("rhabdo")
Cancer with skeletal-muscle differentiation (i.e., sarcomeres on electron microscopy, maybe cross-striations on light
microscopy, positive for desmin and myoglobin, etc.) All are thoroughly
malignant. They are the most common soft tissue sarcomas of children.
Surprisingly, only a minority of these cancers arise in the muscles (probably because skeletal muscle
is pretty much post-mitotic). They can arise most anyplace else (notably the head and neck or the
GU tract).
* "Embryonal rhabdomyosarcoma" usually occurs under age 20.
Look for "tadpole cells" and "strap cells" with cross-striations, and "spider cells", with a nucleus
surrounded and distorted into a spider shape by vacuoles of glycogen.
"Botryoid sarcoma" is an "embryonal rhabdo" with a nice overlying epithelium layer and a packed
"cambium" layer beneath. This uncommon tumor occurs in the urogenital tracts of children.
* "Alveolar rhabdomyosarcoma" is very poorly differentiated. The cells have scanty cytoplasm, and
tend to be arranged in a honeycomb. This lethal, fortunately-rare cancer most often strikes
teenagers. * The NIH folks reclassify rhabdomyosarcomas, so as to put all small-blue-cell rhabdomyosarcomas
in the "alveolar" category: Arch. Path. Lab. Med. 116: 847, 1992. Both have the same poor
prognosis.
* Trademark translocations (1:13) or (2;13) bring either PAX7 or PAX3 adjacent to
FKHR (J. Clin. Onc. 20: 2672, 2002 -- the latter mutation gives a much better prognosis). * "Pleomorphic rhabdomyosarcoma" is similar to, but less well-differentiated than, an "embryonal
rhabdo". It's mostly an older adult's disease.
{24748} rhabdomyosarcoma (striations)
Leiomyoma
We have already seen plenty of leiomyomas in the uterus and GI tract. However, they occasionally
occur away from large hollow organs.
A leiomyoma in the soft tissues often has arisen from blood vessels. These leiomyomas tend to be
painful.
* Future pathologists: You'll make the diagnosis of leiomyoma/leiomyosarcoma
using α-smooth muscle actin immunostain.
Leiomyosarcomas
Uncommon in the soft tissues, but always a consideration, especially if the neoplasm is composed of
spindle cells. Look for staining with desmin and muscle actin.
Immunosuppressed transplant patients tend to develop smooth muscle tumors.
Epstein-Barr virus appears to be the cause (NEJM 332: 19, 1995).
{21122} leiomyosarcoma, gross, femur (trust me)
* Fibromas
Surprisingly, true fibromas (i.e., tumors derived from
common fibroblasts) are rare. "Neurofibromas" arise from schwann cells (again, S100-positive) while "gum fibromas"
are reactive hyperplasias. Papillomas of the skin and
"fibroadenomas" of the breast have abundant stroma that may or may not really be neoplastic.
And so forth.
Fibrosarcomas
Cancer of fibroblasts. Uncommon, and generally well-differentiated.
The familiar identifying feature is the "herringbone" pattern shown nicely in "Big Robbins".
* A variant ("congenital fibrosarcoma" -- present at birth or at least announcing
itself during the first two years of life) features
a distinctive chrosomal translocation and fusion product, ETV6-NTRK3,
which is now assayed routinely (Am. J. Surg. Path. 24: 937, 2000).
{05828} fibrosarcoma, gross
* Elastofibroma occurs only under the scapula and is probably
a hyperplasia due to unusual movement; it was originally described
as an occupational problem of jack-hammer operators. See Clin. Orthop.
Rel. Res. 387: 127, 2001.
Synovial sarcomas (* "Robert Urich's tumor")
A relatively common tumor that usually arises away from synovium, but that
usually shows
both epithelial and spindle-cell differentiation, as you would expect (why?)
* Marker fusion oncogene: SYT-SSX (NEJM 338: 153, 1998; Am. J. Clin. Path. 111:
528, 1999), resulting
from any of three trademark translocations.
{10622} synovial sarcoma
We've already mentioned the major members of the fibromatosis family (Dupuytren's, Peyronie's).
* "Fibromatosis colli" will take out a sternocleidomastoid muscle, while little "fibromas" may stud a
newborn's fingers. Riedel's struma probably belongs here as well.
* Triton tumors
Benign or malignant, these exhibit both Schwann-cell and skeletal-muscle differentiation. Named
for the salamander that regrows its limb-buds.
Desmoids are aggressively invasive but non-metastasizing growths of fibroblasts. The most familiar
variant arises in the abdominal muscles during or after pregnancy. * Not surprisingly, familial
adenomatous polyposis and Gardener's are risk factors for desmoids (Cancer 74: 1270, 1994).
* Nodular fasciitis (South. Med. J. 87: 842, 1994)
A mysterious, self-limited hyperplasia simulating a fibrosarcoma, with infiltration of soft tissue, lots
of mitoses, but no atypia. Don't try to diagnose this one yourself.
Intravascular fasciitis is nodular fasciitis growing down
a vein. It ends up looking like a sausage.
Proliferative fasciitis ("proliferative myositis" when in muscle)
looks like nodular fasciitis with lone big (but not anaplastic)
pink cells interspersed
(look like ganglion cells).
Traumatic myositis ossificans
A jock's disease, which usually follows a large bruise to a muscle. The hematoma organizes into a
tough fibrous mass that seems to infiltrate the muscle (or fat or other soft tissue) and usually exhibits
bony metaplasia.
Don't misdiagnose this as a frightfully aggressive sarcoma. Ask a lawyer whether this turns
malignant or whether injury ever really causes cancer (betcha not).
* Small round cell desmoplastic tumor is yet another sarcoma
with its own trademark translocation t(11,22). In this case, it's EWS/WT1.
Arch. Path. Lab. Med. 126: 126, 2002.
* Extraskeletal chondrosarcomas are typically myxoid, and bear translocations
involving the nuclear receptor TEC. The common one is
t(9:22), producing the EWS/NOR-1 fusion protein; several others exist
(Am. J. Path. 162: 781, 2003; Cancer Res. 60: 6832, 2000).
* Alveolar soft-part sarcoma:
As arcane as you can get.
{09873} alveolar soft part sarcoma, histology
* in some areas of longstanding pressure, where a decubitus might
ordinarily form, these fibroblasts can form a mass (Mod. Path. 6:
69, 1993). This has the name "atypical decubital fibroplasia" or
"ischemic fasciitis". Leave the diagnosis to us.
* Future pathologists: In immunocompromised people, mycobacterial infection can produce
a fibroblastic proliferation that's easy to mistake for a
fibrosarcoma with little anaplasia, especially if you don't think
to do a ZN stain. This is the infamous "inflammatory pseudotumor of
mycobacterial infection".
* Even more mysterious inflammatory pseudotumors -- big yellow masses --
can pop up in various
places around the body, notably the lung or wherever there is
urothelium. Pathologists look for spindle cells, often with
mitotic figures but without florid anaplasia. There will be a mix
of inflammatory cells, mostly lymphocytes and plasma cells; when
the latter are abundant, we talk about "plasma cell granuloma".
{11372} temporal bone and pons, normal
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
Pathology Education Instructional Resource -- U. of Alabama; includes a digital library
Houston Pathology -- loads of great pictures for student doctors
Pathopic -- Swiss site; great resource for the truly hard-core
Syracuse -- pathology cases
Walter Reed -- surgical cases
Alabama's Interactive Pathology Lab
"Companion to Big Robbins" -- very little here yet
Alberta
Pathology Images --hard-core!
Cornell
Image Collection -- great site
Bristol Biomedical
Image Archive
EMBBS Clinical
Photo Library
Chilean Image Bank -- General Pathology -- en Español
Chilean Image Bank -- Systemic Pathology -- en Español
Connecticut
Virtual Pathology Museum
Australian
Interactive Pathology Museum
Semmelweis U.,
Budapest -- enormous pathology photo collection
Iowa Skin
Pathology
Loyola
Dermatology
History of Medicine -- National Library of Medicine
KU
Pathology Home
Page -- friends of mine
The Medical Algorithms Project -- not so much pathology, but worth a visit
National Museum of Health & Medicine -- Armed Forces Institute of Pathology
Telmeds -- brilliant site by the medical students of Panama (Spanish language)
U of
Iowa Dermatology Images
U Wash
Cytogenetics Image Gallery
Urbana
Atlas of Pathology -- great site
Visible
Human Project at NLM
WebPath:
Internet Pathology
Laboratory -- great siteEd Lulo's Pathology Gallery
Bryan Lee's Pathology Museum
Dino Laporte: Pathology Museum
Tom Demark: Pathology Museum
Dan Hammoudi's Site
Claude Roofian's Site
Pathology Handout -- Korean student-generated site; I am pleased to permit their use of my cartoons
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
St.
Jude's Ranch for Children
I've spent time there and they are good. Write "Thanks
Ed" on your check.
PO Box 60100
Boulder City, NV 89006--0100
More of my notes
My medical students
Clinical
Queries -- PubMed from the National Institutes of Health.
Take your questions here first.
HealthWorld
Yahoo! Medline lists other sites that may work well for you

We comply with the
HONcode standard for health trust worthy
information:
verify
here.
QUIZBANK
Muscle & soft tissue #'s 55-61
 Bone and Joint
Bone and Joint
Introductory Pathology Course
University of Texas, Houston
 {14645} osteoblasts, normal
{14645} osteoblasts, normal
{46508} osteoclasts, normal
{14647} osteoclasts, normal
 Tulane Pathology Course
Tulane Pathology Course
Great for this unit
Exact links are always changing
 Bone and Soft Tissue
Bone and Soft Tissue
Great pathology images
Indiana Med School
 Musculoskeletal Disease
Musculoskeletal Disease
Mark W. Braun, M.D.
Photomicrographs
 Musculoskeletal Pathology
Musculoskeletal Pathology
Virginia Commonwealth U.
Great pictures
 Clinical Musculoskeletal Pathology
Clinical Musculoskeletal Pathology
Go through IMC
You need to join first.
 Bone Exhibit
Bone Exhibit
Virtual Pathology Museum
University of Connecticut
 INTRODUCING BONE
INTRODUCING BONE
 Don't worry about Haversian longitudinal systems or Volkmann's transverse / oblique
canals just now. I have no plans to review
bone physiology here. The plural of trabecula is trabeculae.
Don't worry about Haversian longitudinal systems or Volkmann's transverse / oblique
canals just now. I have no plans to review
bone physiology here. The plural of trabecula is trabeculae.
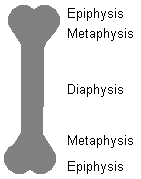 Parts of the long bone (i.e., a bone that formed from a cartilage model):
Parts of the long bone (i.e., a bone that formed from a cartilage model):
People's "bone structure" is widely variable,
and contributes (with muscle mass and body fat) to "build". (Long clavicles and narrow iliac
wings
contribute to "well-built" in a man, but muscle development
overrides these.)
 Epidermoid inclusion cyst
Epidermoid inclusion cyst
"Solitary bone cyst"
NJ Med Pathology -- Case study
 Open fracture
Open fracture
Not wearing a seat belt
WebPath Case of the Week
 Clavicular pseudarthrosis (trust me)
Clavicular pseudarthrosis (trust me)
Prize photograph
Institute of Medical Illustrators
{08994} healing fracture, histology
* Future pathologists: Here's a rough guide to the
x-ray dating of children's fractures.
Two days: Soft tissue edema is usually gone
* Orthopedic nails and screws placed into bone become separated from the
bone itself by organized connective tissue continuous with the periosteum.
* Allogenic stem cells to enhance bone healing: Impressive animal study, no immunosuppression required J. Bone. Surg. 85: 1927, 2003.
 OSTEOGENESIS IMPERFECTA ("brittle bone diseases", * fragilitas ossium; Clin. Ortho. 401: 6, 2002;
Lancet 363: 1377, 2004)
OSTEOGENESIS IMPERFECTA ("brittle bone diseases", * fragilitas ossium; Clin. Ortho. 401: 6, 2002;
Lancet 363: 1377, 2004)
{12402} osteogenesis imperfecta
{15795} osteogenesis imperfecta, blue sclera
{18255} osteogenesis imperfecta type II
{15801} osteogenesis imperfecta type II
{18256} osteogenesis imperfecta, x-ray
{15813} osteogenesis imperfecta, sutures not present


Unbreakable increased
public
awareness of
osteogenesis imperfecta
* Other alleles at collagen loci:
Stickler's syndrome: Gawky people with some degree of nerve deafness; COL2A1 (the
major type II collagen gene) or another
collagen locus: J. Med. Genet. 36: 353, 1999
The most common recessive gene is a defect in an ATPase that is
only expressed in osteoclasts (Am. J. Path. 162: 57, 2003).
{25688} achondroplasia
{49474} "achondroplasia" (looks like a thanatophoric dwarf to me, failure of rib development)

{53760} Apert's
There are a host of genetic syndromes involving bone, from
families where several members share a minor skeletal anomaly
to the horrible fibrodysplasia ossificans progressiva (formerly "bad myositis
ossificans"),
a dominant-but-variably-expressed
mutation (stay tuned; the locus remains elusive)
that causes overproduction of bone morphogenetic protein 4 in which wound
healing is accompanied by exuberant endochondral bone production.
 Fibrodysplasia ossificans progressiva
Fibrodysplasia ossificans progressiva
25 year old man
From NEJM
 Fibrodysplasia ossificans progressiva
Fibrodysplasia ossificans progressiva
Six year old girl
From Kaplan JBJSA 75A
{39505} osteomyelitis, x-ray
{40090} osteomyelitis, draining sinus
* SAPHO syndrome is a rare (and/or underdiagnosed?) illness in which
abscesses appear unpredictably in the skeleton. The acronym stands for synovitis,
acne, pustulosis, hyperostosis (bone bumps especially on the joints,
especially those of the chest), and osteitis. The cause is completely
obscure, but it's being recognized
more nowadays, and being treated effectively with anti-inflammatories
and retinoic acid derivatives.
 Syphilis
Syphilis
Skull showing old gummas
AFIP
 Pathology of Osteoporosis
Pathology of Osteoporosis
WebPath Tutorial
Another gene turns out to be the one for type I collagen, where
certain alleles cause less bone mass and increase the risk for
osteoporosis (NEJM 338: 1016, 1998); collagen mutations can also promote
fractures independent of bone mass (i.e., the bone is poorly-made). Genetics update:
J. Clin. Endo. Metab. 87: 2460, 2002).
{13844} osteoporosis, histology (thin trabeculae)
{46510} osteomalacia, von Kossa stain for calcium (calcified is black, non-calcified is orange)
{12027} renal rickets
{12734} osteitis fibrosa cystica (osteoclast city!)

Certain locales have very high concentrations of fluoride ion in the
water. This is good for preventing dental caries (the teeth are very dark-mottled), but ultimately
causes hyperostosis of the skeleton.
{18781} Paget's disease, skull
{09376} Paget's disease, bowed lower extremities
{09377} Paget's disease, bowed upper extremities
{38210} Paget's disease, histology
{18810} Paget's disease, histology
{13847} Paget's disease, histology
{13850} Paget's disease, polarized light; woven bone
* Worth mentioning here is another disease in which bone
mysteriously transforms, thankfully ultra-rare. Gorham's
essential osteolysis features replacement of bone (usually a single one,
or part of one) by cavernous hemangioma (or maybe just nothing: Virch. Arch. 442: 400, 2003). For some reason, these patients
also tend to get a chylothorax if the spine is involved.
 Fibrous dysplasia
Fibrous dysplasia
NJ Med Pathology
Case study
* An infamous trick question, "What is the most common primary bone tumor?" requires
you to ask whether plasma cell myeloma is under consideration.
* One infamous fooler in radiology is the "sports tumor" of young
people, elevated periosteum where the adductor muscles attach to the femur:
Am. J. Roent. 176: 1227, 2001.
* Osteosarcomas and Ewing's sarcomas are typically
treated with chemotherapy before resection, and the more necrosis seen
in the resected specimen, the better the prognosis.
* Adamantinoma of bone appears benign
clinically, radiographically, and histologically (it recalls tooth enamel cells),
but is locally aggressive and occasionally metastasizes. In the jaw, we call
these ameloblastomas. Otherwise, it'll be in the shaft of the tibia.
 Osteoid osteoma
Osteoid osteoma
NJ Med Pathology
Case study
 Osteoblastoma
Osteoblastoma
NJ Med Pathology
Case study
{05906} osteosarcoma, gross
{05909} osteosarcoma, gross
{05927} osteosarcoma, gross
{05930} osteosarcoma, gross
{24747} osteosarcoma, gross
{21118} osteosarcoma, with pathologic fracture
{10322} parosteal osteogenic sarcoma, gross
{05838} parosteal osteogenic sarcoma, x-ray
{05864} osteosarcoma, histology
{25613} osteosarcoma, histology
{32123} osteosarcoma, histology
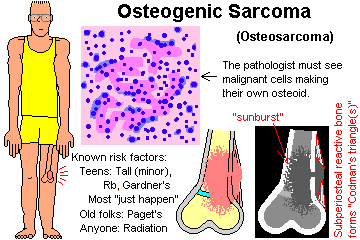
 High-grade osteosarcoma
High-grade osteosarcoma
NJ Med Pathology
Case study
 Cartilage Exhibit
Cartilage Exhibit
Virtual Pathology Museum
University of Connecticut
Future pathologists: Look for lobularity, with more cellularity at the edges than at the centers
 Chondromyxoid fibroma
Chondromyxoid fibroma
NJ Med Pathology
Case study
 Low-grade chondrosarcoma
Low-grade chondrosarcoma
Soap bubble x-ray
NJ Med Pathology -- Case study
* For some reason, chondrosarcomas of the cricoid cartilage are fairly common.
Managing them is tricky.
{09637} chondrosarcoma, gross
{46512} chondrosarcoma, gross
{49494} chondrosarcoma, gross
{09643} chondrosarcoma, lost its differentiation
{09649} chondrosarcoma, rib, gross
{10319} chondrosarcoma, pubis
{08997} chondrosarcoma, histology
{35999} chondrosarcoma, histology
{08998} chondrosarcoma, histology
* A final cartilage lesion worth learning (later) is synovial chondromatosis,
in which metaplasia of synovium into balls of cartilage produces a picturesque,
mysterious lesion easy to diagnose on x-ray.
{46408} Ewing's sarcoma, gross
{08470} Ewing's sarcoma, gross
{05812} Ewing's sarcoma
{38204} Ewing's sarcoma, histology
{40496} Ewing's sarcoma, histology (reticulin stain)
{46410} Ewing's sarcoma, small undifferentiated cells
{46411} Ewing's sarcoma, widespread necrosis
 Ewing's Sarcoma
Ewing's Sarcoma
NJ Med Pathology
Case study
 Giant Cell Tumor of Bone
Giant Cell Tumor of Bone
NJ Med Pathology
Case study
{21127} malignant fibrous histiocytoma, trust me  Paget's disease
Paget's disease
Malignant fibrous histiocytoma
NJ Med Pathology case study
 Eosinophilic granuloma
Eosinophilic granuloma
NJ Med Pathology
Case study
 Lipomatous and Myxoid Tumors
Lipomatous and Myxoid Tumors
Histopathology and essay
For pathologists
The best-known risk factor
is previous radiation (especially radiation therapy). Most often
this gives rise to malignant fibrous histiocytomas; next most common
are fibrosarcomas and angiosarcomas (Ann. Surg. 239: 903, 2004).
{09019} malignant fibrous histiocytoma, histology
{09020} malignant fibrous histiocytoma, histology
{09021} malignant fibrous histiocytoma, histology
{09119} malignant fibrous histiocytoma, electron micrograph; see the macrophage features?
 Malignant fibrous histiocytoma
Malignant fibrous histiocytoma
Tom Demark's Site
The familiar bumps on the buttocks and thighs. Women are much
more likely to be affected, nobody knows why.
{12172} lipoma, gross
{12171} lipoma, gross
{15460} lipoma, colon
{40056} lipoma, gross
 Brown fat
Brown fat
Rrelatively large vacuoles
ERF/KCUMB
 Hibernoma
Hibernoma
Tom Demark's Site
{25413} adrenal myelolipoma
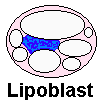
* Let us worry about "atypical lipomas", "pleomorphic lipoma with
floret cells", and so forth.
The translocation t(12;16) fusion product TLS-CHOP is well-characterized (Am. J. Clin. Path. 108: 35, 1997).
{05807} liposarcoma, gross (a big one!)
{10607} liposarcoma, gross
{09004} liposarcoma, histology
{24750} liposarcoma, fat stain
 Rhabdomyoma
Rhabdomyoma
Pittsburgh Pathology Cases
{10955} rhabdomyosarcoma (straps and tadpoles)
{16703} rhabdomyosarcoma, spindle-cell variant
{16704} ditto, electron micrograph
{09006} alveolar rhabdomyosarcoma, histology
{24858} sarcoma botryoides, gross and x-ray
{25303} embryonal rhabdomyosarcoma
{25304} embryonal rhabdomyosarcoma
{25305} sarcoma botryoides, cambium layer
 Rhabdomyoblast
Rhabdomyoblast
Nuclei at edges
ERF/KCUMB
 Leiomyoma of the hand
Leiomyoma of the hand
Ugly but benign
Loyola Med
 Leiomyoma
Leiomyoma
Electron micrographs
VCU Pathology
{05834} leiomyosarcoma, gross (trust me)
{25357} leiomyosarcoma, gross (trust me)
{09016} leiomyosarcoma, histology
{05831} fibrosarcoma, gross
{16680} synovial sarcoma, good biphasic histology
{40604} synovial sarcoma, biphasic
 Dupuytren's
Dupuytren's
Nice photos
Rockford Case of the Month
 Proliferative fasciitis
Proliferative fasciitis
Virginia
Good pictures
{09875} alveolar soft part sarcoma, PAS stain showing crystals
{09876} alveolar soft part sarcoma, PAS stain showing crystals
 Aseptic necrosis
Aseptic necrosis
Bo Jackson's disease
WebPath Tutorial
Frisky fibroblasts
Future pathologists need to be on guard against calling "sarcoma!" on
large fibroblasts with hyperchromatic nuclei that they'll sometimes
see in the craters of ulcers (gut, decubiti).
{11756} bone, normal
{11757} bone, normal
{11758} cartilage, normal
{11759} cartilage, normal
{12064} hand & wrist bones, severe joint erosion abnormal joint congruity
{12206} bone marrow, normal
{12263} bone marrow, normal
{12266} bone marrow, normal
{13619} bone marrow aspirate, normal
{14630} hyaline cartilage (lacunae)
{14631} hyaline cartilage (lacunae)
{14632} hyaline cartilage, normal
{14633} hyaline cartilage, normal
{14634} hyaline cartilage, normal
{14635} hyaline cartilage, normal
{14636} elastic cartilage, normal
{14637} elastic cartilage, normal
{14638} elastic cartilage, normal
{14639} cartilage, calcifying (electron micrograph)
{14640} cartilage, calcifying (electron micrograph)
{14641} fibrocartilage, normal
{14642} fibrocartilage, normal
{14643} fibrocartilage (polarized), normal
{14644} osteoblasts (developing bone), normal
{14645} osteoblasts (developing bone), normal
{14646} osteoclasts (howship's lacunae), howship's lacunae
{14647} osteoclasts (howship's lacunae), howship's lacunae
{14648} osteoblasts (active), normal
{14649} osteoblasts (active), normal
{14650} bone, cortical
{14651} bone, cortical
{14652} bone, adult cortical
{14653} bone, adult cortical
{14654} haversian system in formation
{14655} haversian system in formation
{14656} resorption cavity, bone
{14657} resorption cavity, bone
{14658} osteon (forming)
{14659} osteon (forming)
{14660} cortical spongy bone, normal
{14661} cortical spongy bone, normal
{14662} cortical & spongy bone (polarized), cross section with polarized light
{14663} cortical & spongy bone (polarized), cross section with polarized light
{14664} osteoblast ultrastruct., electron micrograph
{14665} osteoblast ultrastruct., electron micrograph
{14666} osteoclast, normal
{14666} osteoclast, normal
{14667} osteoclast, normal
{14668} osteoclast ruffled border (electron micrograph)
{14669} osteocyte (electron micrograph), normal
{14670} intramembranous bone formation, normal
{14671} intramembranous bone formation, normal
{14672} osteoclast ruffled border (electron micrograph)
{14673} osteoclast ruffled border (electron micrograph)
{14674} primary spongy bone formation
{14675} primary spongy bone formation, normal
{14676} bone, development of typical long bone
{14677} bone, development of typical long bone
{14678} tetracycline label of bone-forming site
{14679} tetracycline label of bone-forming site
{14680} spongy bone, modeling
{14681} spongy bone, modeling
{14682} trabecular bone resorption
{14683} trabecular bone resorption
{14684} bone lining cells
{14685} bone lining cells
{15121} cartilage, hyaline
{15123} cartilage, elastic
{15124} cartilage, elastic
{15126} cartilage, fibrous
{15130} cartilage, fibrous
{15131} cartilage, fibrous
{15132} cartilage, fibrous
{15133} bone, puppy
{15134} bone, puppy
{15135} bone, puppy
{15136} bone, puppy
{15137} osteoblast in puppy bone, #8
{15138} bone, * cartilaginous
{15139} bone, * cartilaginous
{15140} bone, * cartilaginous
{15141} cartilage, articular
{15142} cartilage, articular
{15143} bone, cement
{15144} bone, cement
{15301} bronchus, cartilage
{15918} bone growth plate, normal
{16343} temporal bone, normal
{20285} bone, normal
{20737} cartilage, hyaline
{20738} cartilage, hyaline
{20739} cartilage, elastic
{20740} cartilage, elastic
{20741} cartilage, elastic
{20742} cartilage, elastic
{20743} cartilage, fibrous
{20744} cartilage, fibrous
{20745} bone, osteocyte
{20746} bone, osteoclast
{20747} bone, intramembranous bone formation
{20748} bone, endochondral bone formation
{20749} bone, endochondral bone formation
{20750} bone, endochondral bone formation
{20751} bone, endochondral bone formation
{20752} bone, endochondral bone formation
{20753} bone, endochondral bone formation
{20754} bone, endochondral bone formation
{20755} bone, endochondral bone formation
{20901} cartilage, elastic
{20908} cartilage, hyaline
{46393} osteogenesis imperfecta, normal
{48426} skull, normal
| Visitors to www.pathguy.com reset Jan. 30, 2005: |
Ed says, "This world would be a sorry place if
people like me who call ourselves Christians
didn't try to act as good as
other
good people
."
Prayer Request
 Drop by
and meet Ed
Drop by
and meet Ed Teaching Pathology
Teaching Pathology
PathMax -- Shawn E. Cowper MD's
pathology education links
Ed's Autopsy Page
Notes for Good Lecturers
Small Group Teaching
Socratic
Teaching
Preventing "F"'s
Classroom Control
"I Hate Histology!"
Ed's Physiology Challenge
Pathology Identification
Keys ("Kansas City Field Guide to Pathology")
Ed's Basic Science
Trivia Quiz -- have a chuckle!
Rudolf
Virchow on Pathology Education -- humor
Curriculum Position Paper -- humor
The Pathology Blues
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |