


Cyberfriends: The help you're looking for is probably here.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com Your confidentiality is completely respected.
 DoctorGeorge.com is a larger, full-time service. There is also a fee site at myphysicians.com, and another at www.afraidtoask.com.
DoctorGeorge.com is a larger, full-time service. There is also a fee site at myphysicians.com, and another at www.afraidtoask.com.
Translate this page automatically
 | With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource. Someday you may be able to access these pictures directly from this page.
Also:
Medmark Pathology -- massive listing of pathology sites
Freely have you received, freely give. -- Matthew 10:8. My site receives an enormous amount of traffic, and I'm
handling about 200 requests for information weekly, all
as a public service.
Pathology's modern founder,
Rudolf Virchow M.D., left a legacy
of realism and social conscience for the discipline. I am a mainstream Christian, a man of science, and a proponent of common sense and common kindness. I am an outspoken enemy of
all the make-believe and bunk that interfere with
peoples' health, reasonable freedom, and happiness. I
talk and write straight, and without apology.
Throughout these notes, I am speaking only
for myself, and not for any employer, organization,
or associate.
Special thanks to my friend and colleague,
Charles Wheeler M.D.,
pathologist and former Kansas City mayor. Thanks also
to the real Patch
Adams M.D., who wrote me encouragement when we were both beginning our unusual medical careers.
If you're a private individual who's
enjoyed this site, and want to say, "Thank you, Ed!", then what I'd like best is a contribution to the Episcopalian home for abandoned, neglected, and abused kids in Nevada:
My home page
Especially if you're looking for
information on a disease with a name
that you know, here are a couple of
great places for you to go right now
and use Medline, which will
allow you to find every relevant
current scientific publication.
You owe it to yourself to learn to
use this invaluable internet resource.
Not only will you find some information
immediately, but you'll have references
to journal articles that you can obtain
by interlibrary loan, plus the names of
the world's foremost experts and their
institutions.
Alternative (complementary) medicine has made real progress since my generally-unfavorable 1983 review linked below. If you are interested in complementary medicine, then I would urge you to visit my new
Alternative Medicine page. If you are looking for something on complementary
medicine, please go first to
the American
Association of Naturopathic Physicians.
And for your enjoyment... here are some of my old pathology exams for medical school undergraduates.
I cannot examine every claim that my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship by suspending their own reasoning and
simply accepting a single authority that seems wise and good. I've learned that they leave the movements when, and only when, they discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer answer my crank mail.
This site is my hobby, and I presently have no sponsor.
This page was last updated February 6, 2006.
During the ten years my site has been online, it's proved to be
one of the most popular of all internet sites for undergraduate
physician and allied-health education. It is so well-known
that I'm not worried about borrowers.
I never refuse requests from colleagues for permission to
adapt or duplicate it for their own courses... and many do.
So, fellow-teachers,
help yourselves. Don't sell it for a profit, don't use it for a bad purpose,
and at some time in your course, mention me as author and KCUMB as my institution. Drop me a note about
your successes. And special
thanks to everyone who's helped and encouraged me, and especially the
people at KCUMB
for making it possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it, here or elsewhere. Health and friendship!
INTRODUCTION
You already know the basics:
Skeletal ("striated") muscle is for posture and locomotion. Its syncytial, multinucleate cells ("myocytes", "myofibers", "muscle fibers") may be as thick as 100 microns, and are as long as the muscle itself. Fewer than 3-5%
(usually much fewer) of nuclei should be centrally located, with the rest beneath the sarcolemma.
There is no need to review actin and myosin (the "myofilaments"), sarcomeres (the basic units laid end-to-end to form "myofibrils"), bands, endomysium (the connective tissue around a muscle cell), perimysium (the connective tissue
around a group of fibers, or "fascicle"), or epimysium ("fascia"). By contrast, exactly how skeletal muscle gets bigger (from strength training) and smaller (from disuse or disease) remains
mysterious (Lancet 357: 734, 2001).
One lower motor neuron and the (several) muscle cells that it innervates make up a motor unit. A muscle that is stretched too hard / fast will tear its capillaries and myofibers where it joins its tendon ("muscle injury" / "muscle strain"), since
this is where the forces are strongest (why?).
Pathologists seldom pay much attention to physical injuries to non-fatal muscle, tendon, or ligament.
Sprains are damaged ligaments. The pain is from the microbleeds and edema. Here's a grading system:
Strains result from physical stretching of muscle in opposite directions. They're most
severe at the muscle-tendon junction (where the force is greatest; why?);
Their ultrastructural correlates, which
must be interesting, have not been well-studied.
Heat cramps occur when blood volume and/or blood sodium are low because
of heat, in the muscles that have been exercised most heavily.
The muscles are painful and seem to contract on their own.
* Whiplash is probably strain-sprain of the neck from
acceleration-deceleration, with perhaps some damage to the brainstem (PET scan J. Neur. Neurosurg. Psy. 63:
373, 1997; more J. Trauma 52: 521, 2002), with an overlay from the lawyers. When you could no longer get damages for pain and suffering, patients got much better much faster (NEJM 342: 1211, 2000). If you believe that it's fundamentally a spine problem, you'll
have trouble explaining the negative results of injection therapy (NEJM 330: 1083, 1994). Strains and sprains get better in a few months at most, regardless.
New radiologic techniques have clarified what happens in the vertebrae:
the ventral
lesions result from overstretching ("tensile failure") of the joint capsule,
and the dorsal lesions from pinching the joint capsule / synovium as the
facets are smashed together (Spine 29: 1764, 2004). If something else is
happening to the brainstem, imaging has not revealed it
Muscle fibers are divided into two histochemical types: Slow-twitch ("red fibers", "type I fibers", "myoglobin-, bulky sacromere-, lipid- and mitochondrion-rich", "oxidative
muscle", "dark meat", "marathon muscle")
are responsible for maintaining posture and help with strength athletics. Fast-twitch ("white fibers", "type II fibers", "glycogen-rich", "glycolytic enzyme-rich", "glycolytic muscle", "white meat",
"sprinter muscle")
are responsible for rapid contraction and bursts of speed. The fiber type is determined by the axon that currently supplies it. Some lower motor neurons innervate type I fibers, while others innervate type II fibers. Since there are so many neurons, the arrangement of type I and type II
fibers should seem random in health. {14381} normal; NADH stain with type I fibers dark, type II fibers light
Unlike in chickens, each of our named muscles contains a mix of these two fiber types. Within broad guidelines (i.e., postural muscles like soleus are mostly slow-twitch), your genes determine the relative proportions of type I and
type II fibers in individual muscles. Communist-bloc coaches used to biopsy their prospective olympians to help them match sports to muscle fiber type predominance. Diseases that involve primarily the muscle cells typically present as weakness (look for a baby's head flopping, a child's exaggerated lumbar lordosis, or in an older person, bow legs, difficulty getting out of a chair, winging of
the scapula), and maybe atrophy.
Myotonia is characteristic of a few muscle problems; it may be "grip myotonia" (i.e., the muscles remain contracted for too long after they are used), and/or "percussion myotonia" (i.e., the muscles contract when handled).
Myotonic dystrophy people usually have both. The problem, of course, is repetitive electrical activity on the sarcolemma. While the pattern of muscle involvement may suggest a diagnosis, often muscle biopsy is required. Sore
muscles are more likely to be due to vasculitis (lupus, polyarteritis nodosa), strain, infections (remember trichinosis), or polymyositis.
REACTIONS OF MUSCLE CELLS Simple atrophy of muscle cells occurs when they are
(1) deprived of its nerve supply ("neurogenic atrophy"), or (2) deprived of its blood supply ("ischemic atrophy"), or (3) not used ("disuse atrophy") or,
(4) subjected to glucocorticoids (today, that's mostly "iatrogenic atrophy"). * (5) vitamin D deficient (more common than you think? Arch. Int. Med. 160: 1199, 2000)
Atrophic fibers lose their volume (and cross-sectional area) but keep their nuclei. If surrounding fibers are more normal, atrophic fibers will appear angulated due to compression. If a group of fibers atrophies together, as in
ischemia or very severe disease, the fibers will be round instead. Very atrophic fibers become "nuclear graveyards".
Disuse atrophy and glucocorticoid atrophy involve primarily type II fibers.
{14430} disuse or glucocorticoid atrophy, type II fibers Degeneration of muscle fibers usually means "focal coagulation necrosis", or something very much like it.
Fibers shrivel, lose good cross-striations, become hypereosinophilic ("Zenker's hyaline change"), exhibit local nuclear pyknosis, and get entered and
eaten by visiting macrophages. (Rule: Macrophages eating dead muscle do not indicate inflammation. A significant number of lymphocytes or neutrophils does indicate inflammation.) Typically segmental, the fiber can regenerate itself
as long as the endomysial tubule is intact.
{14414} degenerating fibers, early Duchenne's
Regeneration of muscle fibers is a common finding.
Reserve cells ("satellite cells"; nice pictures in Anat. Rec. 222: 6, 1988) in the endomysium proliferate as myoblasts, until the tube is re-filled. The fiber then regenerates. Of course, regenerating fibers have
basophilic cytoplasm, and centrally-located nuclei with lots of euchromatin and obvious nucleoli (i.e., they're busy).
Increased fiber size variation is a nonspecific finding, and may be seen in most muscle diseases, in prolonged neuropathic disease, or in any cause of type II fiber atrophy. Increased numbers of central nuclei is nonspecific but
indicates muscle fiber disease. * Hypercontraction is hypereosinophilia of segments of fibers, where the sarcomeres are clamped shut. This is common in severe muscular dystrophy (i.e., Duchenne's). It's not clear how this differs
from degeneration (if it always does).
Sometimes it is an artifact, i.e., you see it (with no surrounding tissue reaction) in muscle that's not obtained using a isometric clamp to keep the fibers from contracting on their own. Target fibers: curious fibers with centrally-located
masses of scrambled muscle filaments without mitochondria, lots of mitochondria and few sarcomeres in their intermediate areas, and normal sarcoplasm under their sarcolemmal membranes. When you see a target fiber, it almost always
means denervation-reinnervation.
{14393} several target fibers
Angular fibers are isolated atrophic fibers; they are typically compressed by surrounding larger fibers. As noted above, think of any process that makes one fiber smaller than others (denervation is most typical * but also
polymyositis, dystrophy, type II atrophy, etc.) {14421} several angular fibers
NOTE: Markedly variable sizes among neighboring fibers, without angularity or grouping, is more suggestive of muscular dystrophy.
NOTE: A cluster of atrophic cells, all of one type? Neurogenic atrophy (why?) Ring fibers exhibit peripheral myofilaments that run circumferentially (* really spirals). While not specific (they may be an artifact of over-contraction), think of myotonic dystrophy.
{25526} split fiber in early muscular dystrophy Fibrosis (endomysium, perimysium) often follows inflammation and/or atrophy. Fatty ingrowth ("fatty infiltration", not to be confused with "fatty change") is often common in end-stage muscle. With a few exceptions, neither change
is very helpful diagnostically. Future clinicians: When doing a muscle biopsy, remember: (1) Muscle biopsies hurt. Don't do muscle biopsies for "academic" curiosity. If you decide to do the biopsy, warn your patient.
(2) A muscle biopsy in Duchenne's will result in fibrosis and contracture of the muscle; suspected Duchenne's is a relative contraindication to the procedure. (3) Select a muscle that is mildly, but definitely, involved. The
pathology will show best here. (If a muscle isn't weak, the histology won't be abnormal. If the muscle is mostly fibrous tissue and fat, giving a specific diagnosis is probably impossible.
* (4) Don't biopsy near a tendon, or the pathologist may not know how to interpret the "fibrosis", uneven fiber size, and increased nuclei.
(5) Don't biopsy recent sites of injections or electromyography needle insertions.
* (6) The deltoid has an unusual connective tissue pattern, so let the pathologist know if this is your biopsy site.
(7) Keep the muscle fragment from contracting after biopsy. We'll give you a clamp. (8) Today, the diagnosis of each of the common genetic muscle diseases is made on immunohistochemistry, usually on frozen sections, though with
newer antibodies, paraffin-embedded tissue can be used (J. Clin. Path. 54: 517, 2001; fiber typing J. Clin. Path. 55: 375, 2002).
MYASTHENIA GRAVIS
In this disease, which is fairly common
especially
among young women, polyclonal antibodies attack the
acetylcholine receptor (* bungarotoxin binding site) of the post-synaptic membrane of the neuromuscular junction. This is unwholesome, since binding of acetylcholine is blocked, and receptors are degraded too rapidly.
Interestingly, about 30% of these patients have a thymoma, and most of the rest have thymic hyperplasia (i.e., germinal follicles in the thymus gland). Most thymomas
express acetylcholine receptor epitopes on the surfaces of the neoplastic cells (Lancet 339: 707, 1992; Am. J. Path. 148: 1359 & 1839, 1996). We can suppose for now that this is what triggers the disease. The occasional
seronegative myasthenia gravis victim does not have a thymoma: Neurology 42: 586, 1992. * Several other anti-muscle
autoantibodies (anti-titin, anti-ryanodine-receptor, anti-striational)
also commonly turn up in these people (Muscle & Nerve 21: 329, 1998; Arch. Neuro. 62: 442, 2005).
Again, it's supposed to be molecular mimicry.
Occasional patients lack autoantibodies against the acetyl-choline receptor;
these people usually have antibodies against muscle-specific kinase (anti-MuSK) instead,
and do not benefit from thymectomy (Brain 126: 2304, 2003).
As with other autoimmune diseases, patients often have a second serious autoimmune disease. Look for Hashimoto's, lupus, rheumatoid arthritis, autoimmune thyroid disease. * Of course the antibody can cross the placenta, and
weaken the unborn child.
* The myasthenic mouse has T-cells that attack its NMJ's, and since it's a single epitope under attack, there's talk about therapeutic peptides. I hope it works (J. Imm. 152: 4526, 1994). Extended thymectomy (i.e., be
sure you get the little bits of thymus a few cm away from where the gland is supposed to be located) seems to be the procedure of choice nowadays (Ann. Thoracic Surg. 62: 853, 1996).
Patients suffer from weakness, and tire easily. The disease usually begins in the eyes (droopy "ptotic" eyelids, double vision). You'll learn about the "Tensilon test" on rotations. Like most autoimmune diseases, myasthenia
gravis is a disease of exacerbations and remissions, and thanks to the "ICU", today's patients usually die of something else.
This is not an anatomic pathologist's disease. In a minority of patients
clusters of lymphocytes (* "lymphorrhages") appear around the motor end plates (Arch. Path. Lab. Med. 112: 934, 1988; Neurology 41: 1497, 1991; Neurology 38: 1173, 1988). * Aristotle Onassis, who married Jack
Kennedy's widow Jackie, died of myasthenia gravis. Other myasthenic syndromes: In addition to some genetic NMJ problems
(Arch. Neuro. 56: 163, 1999), you need to remember the Eaton-Lambert syndrome, a weakness syndrome typically seen with oat cell carcinoma of the lung, though sometimes alone. These patients
make an autoantibody against calcium channels (NEJM 332: 1467, 1995 review) that blocks release of acetylcholine itself.
Denervation (i.e., lower motor neuron) changes in muscle occur only if the axon itself is damaged. (Contrast "demyelinating disease" of peripheral nerves, which leaves muscle unchanged.) Partially damaged nerve is the site of
axonal sprouting, with axons from surviving neurons growing into the empty spaces once occupied by other axons. Since the current axon supplying a muscle cell determines whether it is a type I or a type II fiber, the redistribution
of a diminished number of axons will result in type grouping of fibers, pathognomonic (in humans) of denervation-reinnervation.
If the disease process continues, and the ability of axons to be replenished is reduced, look for group atrophy of muscle fibers. Sometimes you may see target fibers. Late in the disease, expect to see some myopathic changes,
too.
{14353} neurogenic atrophy
Noteworthy causes of neurogenic atrophy include amyotrophic lateral sclerosis and a variety of other diseases. If denervation is rapid, muscle cells may twitch repetitively due to increased sensitization to acetylcholine,
producing fasciculations.
Werdnig-Hoffman disease ("infantile spinal muscle atrophy") is an autosomal recessive disease of anterior horn cells that produces extremely floppy babies, progressing to death in the first year (there are variants with longer
survival). Histology shows atrophic groups of type I and type II fibers and occasional clusters of huge type I fibers. It results from loss of the SMN ("survival motor neuron") genes;
other alleles produce other spinal muscle atrophy diseases.
{14372} Werdnig-Hoffman disease
* Sodium butyrate for SMA... well, it works in the knockout mouse (Proc. Nat. Acad. Sci. 98: 9808, 2001).
Kugelberg-Welander disease ("the mild counterpart of Werdnig-Hoffman", SMA III) is caused by another allele at the Werdnig-Hoffman locus.
It is a milder disease. All you'll see on muscle biopsy is type-grouping and atrophy.
{14380} Kugelberg-Welander disease (note poor muscular development) Charcot-Marie-Tooth disease features neurogenic-type atrophy of the leg muscles, especially the calves ("champagne-bottle legs").
{14413} Charcot-Marie-Tooth disease, adult In upper motor neuron disease, of course, all you will see is widespread fiber atrophy, mostly of type II cells.
MUSCULAR DYSTROPHY
This is a group of hereditary myopathies, considered together by custom. ("Dystrophy" is a hallowed, basically meaningless word.) Short review Lancet 359: 687, 2002. Common to these diseases is atrophy and loss of muscle
fibers in the absence of nerve disease. Exactly how this happens is only now becoming clear, as the various proteins involved prove to form a membrane complex that gives strength and structure to the muscle cell. Review Science
270: 755, 1995.
Duchenne's muscular dystrophy ("Jerry Lewis's kids") This is a common (one male in 3500), sex-linked recessive trait. One third of cases are new mutations, and no population group is without these people. The fundamental lesion is a lack of dystrophin, an inner-sarcolemmal
cytoskeletal component homologous to spectrin and actin, which appears to strengthen muscle cells and keep them from popping when overworked (Nature 349: 69 & 243, 1991; Proc. Nat. Acad. Sci. 90: 3710, 1993). The gene's
on Xp21. Although the children appear normal at birth,
the muscle is already abnormal, and the problem becomes obvious in early childhood. These boys have symmetric weakness, and must resort to unusual methods to stand up ("Gower's sign"). Fatty ingrowth produces the characteristic
"pseudohypertrophy of the calves". Boys become wheelchair-bound by their early teens.
About 1/3 of these boys are mentally retarded as a result of involvement of a portion of the
locus that also involves a brain protein. Although results are conflicting, the allele seems to be the determining factor
(Neurology 55: 559, 2000),
Cardiomyopathy is also common (cardiomyopathy-only allele Circulation 87: 1854, 1993), and is a problem even for female carriers (JAMA 275: 1335, 1996).
The pathologist sees various myopathic changes, notably degeneration with phagocytosis and regeneration attempts along the muscle fibers. Even in muscles that are not yet weak, each fiber is usually ringed by fibrous tissue. As
the necrosis predominates, the fibers are replaced by fat and scar tissue. The healthier fibers undergo hypertrophy, producing striking variability in the sizes of fibers. Myofiber types are poorly defined.
{14443} Duchenne's, kid
For some reason, affected boys and their carrier mothers have markedly elevated creatine kinase. Electron microscopists see breaks in the sarcolemma and the CK is probably leaking out here.
A woman carrying Duchenne's may be affected due to unfortunate lyonization. By contrast, fortunate lyonization may produce a normal creatine kinase, obscuring the carrier state. Of course, normally-lyonized
carriers show immunostaining for dystrophin around about half of their myofibers (NEJM 321: 398, 1989). A Turner's woman or testicular-feminization "woman" can have the disease. * Autosomal recessive syndromes
indistinguishable clinically from Duchenne's are rare, but do occur (Am. J. Hum. Genet. 45: 63, 1989; Neurology 45: 768, 1995; Arch. Dis. Child. 64: 1501, 1989; adhalin deficiency J. Clin. Invest. 96: 1202,
1995). Caring for the whole person with Duchenne's requires knowledge, skill, and wisdom: Neurology 39: 475, 1989. Gene therapy for Duchenne's has been a challenge because the molecule is so large (Nat. Med. 8: 253,
2002; Nat. Med. 9: 997, 2003). Manipulating circulating stem
cells works in mice: J. Clin. Inv. 114: 192, 2004. Duchenne's patients have been maintained on respirators for as long
as 30 years (Chest 123: 1307, 2003; don't do something like this to me).
* Myoblast transfer for Duchenne's, which works in an animal model, isn't working in people yet. For some reason, the myoblasts simply decide to die when introduced into the human body. NEJM 333: 838, 1995 was the last major
review, but stay tuned.
Becker's muscular dystrophy
"Another sex-linked muscular dystrophy", caused by milder abnormal alleles at the Duchenne's locus. "Becker's" is defined to be "Duchenne's" in which patients can still walk by their 16th birthday. It's less common than
Duchenne's: Lancet 337: 1022, 1991; the cardiomyopathy Am. Heart J. 132: 642, 1996. The problem in most cases is that dystrophin, though present, is mutated into a less-effective form. Dystrophin has several domains
that do different things, and Becker's is very heterogeneous. For a recent review, see Brain 125: 4, 2002.
{14473} Becker's (I think; pseudohypertrophy of calves)
* Tunisian autosomal recessive muscular dystrophy resulting from dystrophin-binding glycoprotein deficiency: Nature 359: 320, 1992. Animal models for Duchenne-Becker's: Ped. Neurol. 6: 265, 1990 (dogs, cats, "mdx"
mice). * Emery-Dreifuss muscular dystrophy is a
mild disease cause by lack of a protein called "emerin" on
the nuclear (rather than the sarcoplasmic)
membrane (gene Nat. Gen. 12: 252 & 264, 1996). The worst problem is the cardiomyopathy.
{27271} Emery-Dreifuss
Myotonic dystrophy
This is an autosomal dominant (* chromosome 19: q13.2-13.3, cloned: Science 255: 1253 & 1256, 1992; protein is "myotonin" Science 260: 235, 1993), variably expressed because of other genes, affecting several systems.
In some communities, it is as common as Duchenne's. Patients have:
{53755} myotonic dystrophy
On muscle biopsy, the pathologist sees:
Myotonic dystrophy is an example of a gene whose bad alleles typically become worse and worse with each generation, through progressive amplification of CTG-repeats. Each generation has the diseases worse. This is "Sherman's paradox
/ genetic anticipation". (More about this under "Huntington's chorea".)
Facioscapulohumeral dystrophy
An autosomal dominant (* locus 4q35: Am. J. Hum. Genet. Aug. 1992) with varying expressivity, and not lethal. Patients' shoulders and upper arms waste away, beginning in their teens or twenties.
Staining muscle with NADH reveals "moth-eaten" or "mottled" myofibers. Other changes are not usually striking.
{14515} facioscapulohumeral dystrophy, patient
Limb-girdle dystrophies
Either the hips or the shoulders are involved,
and weakness leads to progressive disability sometime during adult life. Muscle biopsy often shows central nuclei, but there are no specific findings. * Genes:
Nat. Genet. 11: 257 & 1266, 1995 (the "sarcoglycan" family;
"adhalin" etc.) Over a dozen are known, including calpain-3, gamma-sarcoglycan, caveolin-3, dysferlin (update Neurology 56: 1472, 2001),
myotelin,
and even collagen VI (several eponymous phenotypes depending on the mutation;
as you'd expect, double-jointedness is common;
Neurology 58: 593, 2002; Neurology 59: 920, 2002);
some are dominant, others recessive (Brain 122: 1403, 1999).
Dominant one with anticipation: Neurology 56: 450, 2001.
* Some caveolin-3 mutations produce the rare but picturesque "rippling muscle
disease", with wiggly waves on percussion; Neurol. 57: 2273, 2001.
{14521} limb-girdle dystrophy, patient Congenital muscular dystrophy:
Weak from birth. Several biochemical problems
(update Arch. Neuro. 61: 189, 2004). The deficiency is most often in merosin,
a laminin-like protein; you can diagnose these on skin biopsy instead of going after muscle (Lancet
347: 582, 1996).
in "fiber type disproportion", type I fibers are much smaller than type 2 fibers. This is a feature of several known congenital myopathies, and others that are presently unclassified.
Many other forms of muscular dystrophy exist (laminin deficiency: Neurology 55: 1120, 2000; lots more).
OTHER HEREDITARY MUSCLE DISEASES ("the other congenital myopathies"; floppy babies or lousy athletes)
You have already studied the glycogen storage diseases. For review: Pompe's glycogenosis II (acid maltase deficiency / glucosidase) produces floppy babies, big hearts, and often early death from cardiac failure; milder forms exist.
{15334} teen with mild acid maltase deficiency; looks okay but tires easily at sports McArdle's glycogenosis V (myophosphorylase deficiency) is a mild disease. Glycogen bumps lie beneath the sarcolemma. Patients are poor athletes, and if they try, they get bad cramps and rhabdomyolysis. Genes: NEJM 329:
241, 1993.
Mitochondrial myopathies are inborn errors of metabolism that seem to primarily involve mitochondria. They feature defects in the pyruvate dehydrogenase complex, tRNA synthetases (probably most common, for example
Neurology 44: 975, 1994), ATPase production, and the cytochromes (mitochondrial or autosomal inheritance, see Neurol. 44: 721, 1994). Some also involve the brain ("encephalomyopathies").
They include the mitochondrial-inherited Kearns-Sayre syndrome, with ophthalmoplegia, retinal pigmentation, cerebellar ataxia, and heart block.
By now, dozens of distinct mitochondrially-inherited diseases affecting
muscle
are known, and drugs such as AZT and suramin produce acquired lesions
that look similar.
The histologic hallmark of most of these illnesses is ragged red fibers. These are ragged because there are too many mitochondria, often abnormal ones, clustered around their edges under the
sarcolemma. (* Future pathologists: See them best using
Gomori trichrome stain.)
On electron microscopy, the damaged mitochondria contain "parking-lot crystals" of abnormal * creatine kinase (Proc. Nat. Acad. Sci. 91: 5089, 1994). {14435} mitochondrial myopathy; mitochondrial clusters are dark purple
* A mitochondrial myopathy that'll look normal on biopsy is mutated cytochrome C disease (NEJM 341: 1077, 1999). These patients have severe exercise intolerance and are likely to have lactic acidosis even at rest.
* Defects in carnitine metabolism include several obscure diseases (Pediatrics 84: 312, 1989; Am. J. Ob. Gyn. 170: 1390, 1994). Depending on the problem, muscle cells may be fat-laden or appear normal. There are no
"ragged red fibers".
* Hereditary coenzyme Q deficiency features
ragged red fibers, and
responds dramatically to generous doses of
supplemental
coenzyme Q: Neurology 57: 515, 2001. Rod myopathy ("rod body myopathy", "nemaline myopathy"; "nema"- means "thread") is a family of autosomal-dominant (usually), non- progressive (usually) disorders with widely variable penetrance. The "nemaline rods" are
masses of Z-band material (* notably actinin, where the problem seems to be. Chemistry: J. Neurol. Sci. 93: 199, 1989.
{14376} rod body ("nemaline") myopathy
* Lipid myopathy features fatty change as the major finding. Most of these people have a deficiency in carnitine palmitoyltransferase, and have weakness and rhabdomyolysis if they over-exercise (J. Neuro. Neurosurg. Psych. 62;
169, 1997.) * Central core disease is actually a group of
variably-inherited, variably-severe, often non-progressive diseases that
produce a great preponderance of type I fibers, many with a full-length "central core" where there are no
organelles and even the sarcomeres may be scrambled. (Future pathologists: See it with the NADH tetrazolium reductase stain, or even PAS.)
The most common gene is the ryanodine receptor, the intracellular calcium release channel (Neurology 59: 284, 2002).
* Myotubular myopathies, variously inherited and variably severe, form another plethora of diseases. The deadly X-linked recessive form
is caused by lack of good myotubularin, an ancient membrane protein (Nat. Genet. 18: 303, 1998, Nat. Genet. 13: 175, 1996. * Desmin myopathy (desmin gene mutated): NEJM 342: 770, 2000.
* Myofibrillar myopathies are genetic diseases with dissolution of the sarcomeres beginning at
the Z-disk. Several are known (Neurology 62: 1363, 2004; Brain 127: 439, 2004).
{27319} central core disease; patient (no really diagnostic features visible)
Inclusion body myositis (Am. J. Path. 156: 1835, 2000; Am. J. Path. 164:
1, 2004): A fairly common hereditary or sporadic
inflammatory-necrotizing myopathy. The sporadic form is
common in older adults; it involves especially the grip muscles. The histopathology is distinctive. There are vacuoles containing (surprise!) phosphorylated tau twisted as paired helical filaments, just like the tangles in
Alzheimer's, along with some other Alzheimer proteins. A big deal right now (Am. J. Path. 144: 177, 1994); there's also prion precursor protein and apoprotein E. It stains as amyloid.
* It is basically not treatable, and is notoriously unresponsive to anti-inflammatory medicines. See Neurology 45: 1302, 1995.
* The hereditary form results from lack of one of the carbohydrate-processing enzymes (Neurology 59: 451, 2002).
RHABDOMYOLYSIS (N.Y. State Med. J. 88: 582, 1988) Sometimes myoglobin leaks out of skeletal muscle. This may be acute or chronic.
Some normal
people get rhabdomyolysis after exercise. If you're out of shape and overdo it, you'll probably experience mild rhabdomyolysis (ouch!). If severe, you might have glycogen storage disease (V or VII), or some other unusual problem. We
might hypothesize pH-related cell injury, but details are obscure. Other causes of rhabdomyolysis include crush injury, electrical injury, heat stroke, motor seizures, cocaine abuse,
malignant hyperthermia (see below), long-term glue sniffing (J. Tox. 38: 679, 2000),
or acute systemic viral illness. Alcoholic rhabdomyolysis / myopathy is a minor mystery of medicine when it occurs apart from obvious trauma (Minn. Med. 71: 769, 1988). Some (but
probably not all) of the explanation is that alcoholics (and dopesters) get ischemia of skeletal muscle by not shifting their weight (i.e., people who are passed out don't fidget, toss, and turn like we do.)
Statin myopathy: JAMA 289: 1681, 2003.
Markers for rhabdomyolysis are the same as for any other disease that releases the contents of myofibers. Myoglobin appears in the urine, and the "muscle enzymes" (creatine kinase, aldolase, SGOT, others) rise in the serum.
Large amounts of myoglobin in the glomerular filtrate tend to precipitate in the kidney tubules. Pigment nephropathy is troublesome but seldom lethal.
Regardless of cause, muscle biopsy in "rhabdomyolysis" shows degenerating and regenerating fibers, with macrophages around them, but no lymphocytes or other inflammatory cells.
This might be a good place to mention myositis ossificans, in which endochondral bone formation occurs within the muscular
connective tissue.
Localized myositis ossificans follows trauma and probably represents
bony metaplasia of scar ("myositis ossificans traumatica"). Pathology of the
developing lesions: Clin. Ortho. Rel. Res. 403-S: S-110, 2002.
Progressive fibrodysplasia ossificnas
(formerly "generalized myositis ossificans")
is a dreadful disease in which new cross-links form across the joints, rendering them immobile. These
patients' skeletons end up in pathology museums.
* The cause is some mutation that produces excessive production of bone morphogenetic protein 4 (NEJM 335: 555, 1996). The "noggin"
gene as one locus: Am. J. Med. Genet. 102: 314, 2001. {27349} myositis ossificans; bumps are bone
On your surgical rotations, you'll learn about the various compartment syndromes, in which swelling (especially from reperfusion of muscle ischemic for some other reason) within one of the deep compartments of an extremity
interferes with venous drainage and causes infarction. INVOLVEMENT OF MUSCLE IN SYSTEMIC DISEASE
Probably the most common myopathy you will see (and probably ignore) is alcoholic myopathy. Biopsy that scrawny drunkard's muscle, and you'll find fibrosis between the fibers, and hypertrophy of the remaining fibers (i.e., many
fibers are long- gone). We now know that these are the pretty much the same patients that have the alcoholic cardiomyopathy (Ann. Int. Med. 120: 529, 1994). You are already familiar with the catastrophic clostridial
infection gas gangrene, in which muscle is
prominently involved.
You are also familiar with trichinosis, in which worms encyst and die in the muscles (they seek the busiest and best-perfused, i.e., the diaphragm and external eye muscles).
Lots of
granulomas in the muscle probably indicates sarcoidosis. Twice I've picked up polyarteritis nodosa
(surprise!) on muscle biopsy.
The virus that attacks muscle most aggressively is probably coxsackie virus; also remember dengue. Myositis contributes to the agony of typhus.
"White muscle disease", from selenium deficiency, is mostly a veterinary problem, but is seen
occasionally in malnourished people (Neuro. Neurosurg. Psych. 67: 829, 1999).
You'll need to decide for yourself about "macrophagic myofasciitis",
supposedly a persistent local reaction to aluminum adjuvants in vaccines
though it also occurs where there has been no vaccination (Scand. J. Rheum. 34: 65, 2005);
the anti-immunization community considers it to be the cause of
chronic fatigue syndrome and multiple sclerosis
(Brain 124: 974, 2001).
By contrast, there is a hereditary illness in which these lesions are widespread
and the macrophages are loaded with aluminum (Neuromusc. Dis. 14: 246, 2004).
{46215} pus in necrotic muscle infected with bacteria; this is unusual We hope you are already acquainted with the miserable polymyositis-dermatomyositis ("idiopathic inflammatory myositis",
review Lancet 335 53, 2000). Worth
reiterating:
The problem seems to be that muscle cells start expressing MCH-I antigens, and T-cells then become angry with them.
Selective atrophy of the muscle fibers at the edges of the fascicles is very characteristic, even if there is no inflammation or necrosis. In more severe cases, patches of chronic inflammation are typical, and you may see injured
or dying fibers.
HIV infection at any stage can simulate polymyositis (Arth. Rheum. 49:
172, 2003).
{29501} polymyositis, histology
The most characteristic autoantibodies are directed against several of t-RNA synthetases (J. Immunol. 144: 1737, 1990). Anti-Jo-1 (anti-histidyl-tRNA synthetase) was the first of these antibodies, which are considered
markers for polymyositis & perhaps pulmonary fibrosis. However, these occur only in a minority of cases.
In a large minority of cases, the disease is the first sign of an internal malignancy, especially ovarian cancer.
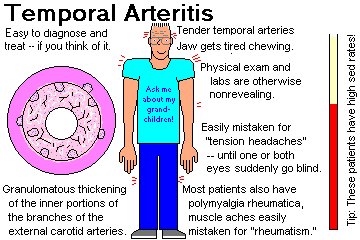
POLYMYALGIA RHEUMATICA (Med. Clin. N.A. 81: 195, 1997; Lancet 350: 36, 1997) A poorly understood but important disease. Almost all patients are older adults, and the
majority are women. Many, if not most, have temporal arteritis (if you ask and/or palpate). There is pain and morning-stiffness in the
neck, shoulders, and hips. Physical exam and routine labs are singularly un-diagnostic. Erythrocyte sedimentation rate is always high. The treatment is tiny doses of systemic glucocorticoids, and patients are grateful.
CRITICAL ILLNESS MYOPATHY ("acute quadriplegic myopathy",
Crit. Care Med. 27: 2544, 1999) Recently recognized as more-than-just-atrophy. Systemic glucocorticoids for emphysema (yeah) or severe asthma or other illnesses is likely to produce profound weakness and pain, of relatively abrupt onset (Am. J. Resp. Crit. Care
Med. 153: 1958, 1996). On biopsy, you'll see: This can land you on the respirator, or ironically, administration of paralyzing agents to steroid-treated people already on the respirator seems to precipitate the disease
(Am. J. Resp. Crit. Care Med. 153: 1686, 1996; Neurology
46: 600, 1996). Don't expect ever to fully recover. * Clinically similar, but different pathologically, are:
Necrotizing myopathy: Vacuolization, necrosis, and phagocytosis of muscle fibers. Yet another illness that seems to be precipitated by glucocorticoids and/or NMJ blockers.
Confusing: "Steroids" in the muscle literature as elsewhere means either glucocorticoids or androgens (see below).
Chloroquine is notorious for producing a myopathy with vacuoles in muscle cells (no marvel; chloroquine exerts its major effects on lysosomes).
THE MUSCLE MEMBRANE DISEASES: Electrical troubles! All about the myotonias: NEJM 328: 482, 1993.
Chloride channel disease -- Myotonia congenita: several inherited diseases with excessive muscle tone. Patients often have considerable muscle hypertrophy and strength, excelling at sports where strength is more important than speed; some (not all) forms eventually cause atrophy. The histology is usually normal or nearly so.
{14500} myotonia congenita with hypertrophy The usual gene for both the common dominant (Thomsen's mild disease * Thomsen had it) and recessive (Becker's more serious disease, not to be confused with Becker's dystrophy) have been found at the CLC-1 ("chloride channel 1")
locus on chromosome 7q (Science 257: 797, 1992). Stay tuned for the discovery of several more alleles here that determine why some guys "naturally" have much bigger muscles than other guys (i.e., it's not just your
testosterone or your "bone structure", dudes). Myotonic dystrophy, of course, also features an electrical disturbance; the gene involves a membrane component.
Several hereditary (usually autosomal dominant) diseases, which feature striking episodes of paralysis without clouding of consciousness. Precipitated respectively with low, normal, and high serum potassium, all seem to respond
to carbonic anhydrase inhibitors, and pathologists seldom see them. Probably some of them go into the SIDS "we don't know exactly why"
category.
Hyperkalemic periodic paralysis shares a locus with paramyotonia congenita (a cold-sensitive myotonia) and potassium-aggravated myotonia,
at a sodium channel on chromosome 17q (SCN4A: J. Neurosci. 19: 4762, 1999). More mutations Neurology 44: 1500, 1994. Yet another allele: Arch. Neur. 51: 1095, 1994 ("myotonia fluctuans").
Hypokalemic periodic
paralysis type I is a dominant calcium channel
mutation (Am. J. Hum. Genet. 56: 374, 1995).
Type II is a dominant sodium channel (CACNA1S: Brain 125: 835, 2002; Neurology 53: 1932, 1999; Neurology 57:
1323, 2001).
There is also a dominant potassium channel (KCNE3) disease that expresses
itself best in the presence of hyperthyrodism; don't ask why (J. Clin. Endo. Metab. 87: 4881, 2002).
* Anderson's (periodic paralysis, sudden death)
is a potassium channel (KCNJ2) mutation: Circulation 105: 2592, 2002. Malignant hyperthermia susceptibility
Some people (around 1 in 5000), when they go under a general anesthetic, develop rhabdomyolysis, acidosis, elevated core temperature, and/or serious heart rhythm problems. The ability to get this is hereditary, usually autosomal
dominant. The mutations are in the voltage-gated calcium channels in skeletal muscle; * most common locus is RYR1, ryanodine receptor; Lancet 352: 1131, 1998; recessive Neurology 59: 284, 2002)
Not skeletal muscle, but worth mentioning again: Sodium channel N5a mutation causes "Brugada's ventricular fibrillation" (Nature 392: 293, 1998).
Stay tuned for more membrane-channel diseases (* for example, hereditary epilepsy from defective potassium channels: Nat. Genet. 18: 53, 1998).
OTHER MUSCLE PROBLEMS
Myofascial pain syndromes
(Arch. Phys. Med. Rehab. 83 (3S1): S40, 2002; Am. Fam. Phys. 65: 653, 2002)
are presently a major mystery of medicine. The problem is electrophysiological
(Am. J. Phys. Med. 81: 212, 2002).
The connection between these nodules, TMJ syndrome, fibromyalgia,
interstitial cystitis, and so forth will be clarified someday.
No one knows
the anatomic pathology.
Acupuncture fails totally: Arch. Phys. Med. Rehab. 82: 986, 2001;
botox offers some hope Arch. Phys. Med. Rehab. 84 3S1: S69, 2003;
electronic muscle stimulation helps Am. J. Phys. Med. Rehab. 76: 471, 1997.
Eosinophilia-myalgia syndrome
This was a myositis (etc., primarily a vasculitis, and with scleroderma-like skin changes), with severe pain and weakness, seen in people who took L-tryptophan tablets from the "health-food" industry. Circulating levels of
eosinophils were very high, and eosinophils and their debris were abundant in the damaged tissues.
The cause was the impurity 1,1'-ethylidenebis[tryptophan]. Review: Mayo Clin. Proc. 66: 535, 1991). See also South. Med. J. 83: 675, 1990; Chest 97: 1032, 1990; NEJM 322: 869, 1990; Hosp. Pract.
27(4A): 65, April 30, 1992.
* Don't worry about similar, rare diseases (eosinophilic fasciitis, the
controversial "human adjuvant disease" following implants, etc.)
* Rhabdomyosarcoma {24748} rhabdomyosarcoma (striations)
HERE'S A SELECTION OF MUSCLE PATHOLOGY
ATHLETICS
Muscles are fun. Athletes push their bodies to extremes seldom seen even in disease. * At Northwestern, we had a histotechnologist who ran 16 miles to and from work daily. It was fun introducing him to clinicians and having them "check out his heart". The pediatric athlete: Orthop. Clin. N.A. 26: 453,
1995. You measure aerobic fitness by how much oxygen you can use, for your size, in a minute. Aerobic training changes a number of parameters. Perhaps the most important is an increase mitochondrial activity in both type I and type II
fibers (Am J. Physio. 278:E-153, 2000). Glycolytic enzymes are increased, and there is also talk of increased numbers of capillaries. Unless the muscle is working against resistance, don't expect to see a significant gain in
muscle mass or strength.
Of course, the changes of the aerobically-trained person are not confined to voluntary muscles. The
muscle that is most affected by aerobic training is the heart. It undergoes hypertrophy (which is good in this instance; it can also beat slower).
Claims of "improved lung function" are hard to demonstrate,
but the shapes of marathon runners' chests do change to
improve air supply. Ask a trainer about carbohydrate-loading to increase muscle
glycogen stores (and thereby endurance) before the big race.
Being aerobically fit clearly is a powerful way of forestalling the onset of type II
diabetes (Ann. Int. Med. 143: 251 & 323, 2005); the studies are getting more and more impressive. * How does exercise help your lipoproteins? This year, the explanation goes like so: (1) exercising muscle's lipoprotein lipase
selectively removes triglyceride from VLDL's; (2) this shrinks them and cholesterol molecules fall off the surfaces; (3) and the cholesterol ends up on HDL. * Being fit helps older folks sleep better, etc., etc., etc., JAMA
277: 32, 1997. We're still reading studies that "show" the benefits of exercise to be tremendous (for example, JAMA
273: 1093, 1995 measured aerobic fitness and found an 8x reduction in coronary mortality, and an overall mortality reduction in 44%; similar Lancet 352: 759, 1998). Before you embark on your own aerobic fitness program,
reflect that (1) being sick lowers your aerobic fitness, and (2) being sick in the first place makes it less likely that you will exercise, and
(3) people who exercise have other healthier habits.
Of course you cannot control for these in a prospective study.... The retrospective review in JAMA 276: 205, 1996 struck me as more credible, and the benefits are almost certainly real. NIH consensus statement about
physical-fitness and cardiovascular health: Am. Fam. Phys. 54: 763, 1996, JAMA 276: 241, 1996. The Surgeon General: JAMA 276: 522, 1996. * Uncle Sam spends megabucks on "the primary prevention
of heart disease" at the grammar school level, including extensive indoctrination of the kids, and ends up proclaiming triumphantly that kids in the study group (i.e., who'd been told at length what Uncle Sam wanted them to say)
reported reducing their percentage of fat calories by a whopping 2%, and reported exercising 12 more minutes a day than controls. Uncle Sam also compared body size and cholesterol levels (no difference) but not adiposity or
muscularity. JAMA 275: 768, 1996. Your tax dollars at work. More from Uncle Sam: He spent more money in 1996 and discovered that most fat people do not exercise much during their leisure time (JAMA 275: 905, 1996),
wow. In 1998, more of your tax money went to show that kids who watch more TV exercise less and are fatter! The authors wanted more money so they could spend it on health promotion (JAMA 279: 938, 1998), uh huh.
Muscle strength training ("getting bulked up") involves overcoming resistance, typically "pumping iron".
Muscle strength is proportionate to muscle mass. A large limb muscle can lift about 3 kg/cm2 of its maximum cross-sectional area. The amount of load that a muscle can hold steady is around 40% greater than the amount
it can lift, and for very strong men, this exceeds the force holding the tendons to the bone. Ruptures of the biceps and other tendons are not uncommon. A person's muscle mass ("muscle bulk") is determined by a combination of
heredity (* probably including differences in base muscle tone and the genetic markers listed below), personal average androgen levels (widely variable even among people of the same gender), and the strength demands placed on the
muscle. By contrast, "muscle definition" ("getting trimmed / ripped / cut") results from both muscle bulk and (more important) lack of subcutaneous fat. Much sought-after, bodybuilders diet and do even aerobic exercise before shows or
photos. It is probably not possible to "spot-reduce" fat from one portion of your body, and be skeptical when someone tells you a particular exercise is "particularly good for definition". As noted above, an aerobically-trained
adult also has about one liter more blood, which helps a "cut" person look "vascular" too. Again, much sought-after (contrast anorectics and zero-bodyfat "heroin chic" addicts).
As I predicted in 2001, the study of the serum autocrine factor "myostatin" has become
central to the field of muscle physiology (Science 296:1486, 2004).
The hormone enables fat production and muscle atrophy.
Belgian Blue cattle, which are lean and grotesquely muscled,
lack myostatin (Nat. Genet. 17: 71, 1997).
So are knockout mice lacking this protein (Proc. Nat. Acad. Sci. 98: 9306, 2001),
and there's now a homozygous baby (NEJM 350: 2682, 2004 -- Mom won't say
who Dad is, but she
and her family are strength athletes, surely heterozygotes).
"Supraphysiological doses of testosterone" (NEJM 335: 1, 1996) and resistance training both (and especially together) cause hypertrophy of the fibers (type II fibers in every sport, type I's when endurance is a factor), with
increases in the numbers of myofilaments and even sarcomeres. We now know that, despite traditional teaching, a weight-lifter's muscle fibers may divide, or (more important) new fibers form from satellite cells. ("Muscles have a memory" after all. See Anat. Rec. 233: 178, 1992;
Med. Sci. Sport 31: 1528, 1999.)
The key to building bulk is (1) lifting heavy weights (today's trainers recommend 3 sets of 6-10 repetitions of your maximum weight, three times a week), and (2) anabolic steroids (your own male hormones, or see below.) A man who
lifts weights several times a week is likely to increase his muscle mass by around 30% after eight weeks. This will impress his male buddies and perhaps even a few women.
Some men bulk up much more easily than others do.
Gym types talk about "easy gainers" and "hard
gainers". The genetics of this isn't understood.
Another
locus is the angiotensin-converting-enzyme gene (where the allele seems to determine how much muscle you build
in response to strength training): Lancet 353: 541, 1999; J. Clin. Endo. Metab. 86:
2200, 2001). Watch for
variations in the myogenic proteins (such as "herculin"/Myf6/MRF4) to explain differences from person to person.
You can read on your own about changes in myosin heavy chain subtypes in resistance-trained muscle, and so forth.
Far more men work out with weights today than in past decades. This is
probably healthy, and it has also changed the image of what a fit man is expected to look like
(Am. J. Psych. 162: 263, 2005).
Compare yesterday's action-hero macho-man actors
with today's gentle-ordinary-guy actors; the old pictures of Superman with the new ones; and even GI Joe's from the 1960's with today's models. {18664} "pumped"
The
politically-correct view in the medical literature for decades has been to emphasize the health-benefits of aerobic training, and to dismiss the idea that strength training has benefits beyond sports.
This all changed in the 1990's.
The academicians finally got around to seeing whether having post-polio patients pump some light iron helped, and of course it did (Am. J. Phys. Med. Rehab. 75: 50, 1996). Strength training helps old folks walk
farther (Ann. Int. Med. 124: 568, 1996), re-muscles the elderly so they can do more ("reversing sarcopenia", Geriatrics 51: 46, 1996), strengthens rheumatoid arthritis patients and causes them to report less pain and
less fatigue (Arth. Rheum. 39: 415, 1996),
reduces (!) osteoarthritis activity in the knee (Nsg. Res. 45: 68, 1996), etc., etc.
Even the fibromyalgia patients benefit significantly (Arth. Rheum. 47: 22, 2002).
Nobody's looked at the effects of strength training on lipids. What's more, resistance
training bulks the heart (Cardiology 90: 145, 1998) as aerobic exercise does. This was so politically incorrect that at first all the big-hearted bodybuilders in the study were wrongly accused just on this
evidence of taking anabolic steroids.
Science is now winning out over politics,
at least here.
Lifting is safe, even for younger kids if you supervise them properly (Sports Med. 15: 389, 1993), the emphysema folks (it makes them feel better! Thorax 47: 70, 1992), and the coronary-disease guys (Am. J. Card.
71: 287, 1993; Am. J. Card. 67: 939, 1991). The skeletal muscle mass of a distance runner is around 38% of body weight; for a bodybuilder, it's around 59% (J. Sports Sci. 11: 3, 1993). Bodybuilders will ask you for your opinions about various nutritional supplements to enhance their performance. Despite the advertisements, the ones that have been tested lately have been total flops (animo acids: Int. J. Sport.
Nutr. 3: 290, 298 & 306, 1993; boron: Int. J. Sport. Nutr. 3: 140, 1993; chromium picolinate Int. J. Sport. Nutr. 2: 343, 1992; growth hormone J. Appl. Phys. 74: 3073, 1993; I could only get these as
abstracts). So what works?
The value of both creatine (J. Fam. Pract. 51: 945, 2002;
Am. J. Clin. Nutr. 72(S2): 607-S, 2000) and post-exercise
intake of protein or carbohydrate are now established (Can. J. Appl. Phys. 25: 254, 2000.) Creatine evidently makes the satellite cells divide (Int. J.
Sports Med. 21: 13, 2000). Early concerns about creatine producing
rhabdomyolysis seem to have come to nothing. Creatine is now being used
to prevent muscle wasting during, and restore muscle mass after, immobilization
(Diabetes 50: 18, 2001).
No offense to anybody, but eating meat (rather than just other animal or vegetable proteins)
helps too (Am. J. Clin. Nutr. 70: 1032, 1999).
While lifting weights, it's best to keep your glottis open, and not Valsalva. The more elaborate instructions about "when to breathe in, when to breathe out" are of course designed to make lifters keep their glottis open. Weightlifting
builds and strengthens older folks (60+). J. Ger. Mar. 1995;
Am. J. Phys. Med. Rehab. 81(S-11): S3, 2002).
Older diabetics: J. Ger. 58: 740, 2003.
* Weightlifting seems neither to help nor hurt myotonic dystrophy patients, while it apparently helps
some neuropathy patients (Arch. Phys. Med. Rehab. 76: 612, 1995). Synthetic anabolic steroids: ("breakfast of champions", etc.; review Clin. Sports Med. 18: 667, 1999;
South. Med. J. 98: 550, 2005 explains what "stacking" and "pyramiding" are)
Around one million Americans will take man-made anabolic steroids illicitly to bulk their muscles this year (see references below), often in doses up to 40 times what is recommended for therapeutic use (reversing negative nitrogen
balance, preventing angioedema). * The unfortunate man who didn't know what was really in his "protein health drink" prepared specially at the gym: Br. Med. J. 313: 100, 1996.
* Today, senior bodybuilders are much sought-after as supposedly possessing arcane knowledge about anabolic steroids, and there is a huge underground literature, much of which strikes me as dubious. Review (finally) in Sports Med.
32: 285, 2002, by the psychiatrists at Western Missouri.
Weightlifting and 'roids for the men with AIDS wasting (which can proceed even if you are on protease inhibitors): JAMA 281: 1282, 1999. 'Roids help the man on dialysis stay well-muscled and well-functioning: JAMA
281: 1275, 1999. For the women: Arch. Int. Med. 165: 578, 2005 (seems safe and
effective).
They work. Men (South. Med. J. 84: 552, 1991, and even women; see Am. J. Ob. Gyn. 165: 1385, 1991) can and do develop spectacular muscles using steroids, and the drugs also improve mood and increase aggressiveness
(JAMA 269: 2760, 1993 for the first placebo-controlled study; one guy in the subject group went crazy).
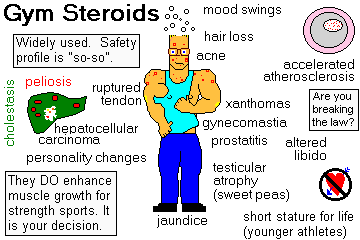
Users are willing to take the risks, which include:
All are probably common except for the tumors, the thromboemboli, the necrosis of the hips, the strokes, and the ruptured tendons. In addition, women are likely to grow thick hair on their faces and other un-feminine places, and
smell as bad as we men do because of the hypertrophy-hyperplasia of the apocrine glands. Pee-yoo! You have been warned.
Between 5% (Am. J. Dis. Child. 144: 99, 1990) and 11% (Pediatrics 83: 921, 1989) of high school athletes have used anabolic steroids. One recent study cites 7.6% of high-school males and 1.5% of high-school females
(!; Am. J. Dis. Child. 14: 823, 1992). Parents request them for their skinny, non-athletic sons (Pediatrics 84: 940, 1989). We won't talk about college, Olympic, or professional athletes. In a switch from
complete condemnation, the pediatricians (Pediatrics 99: 904, 1997)
now talk about moderate
steroid use as a personal choice for the young athlete (though of course it's probably
illegal and immoral). Today's common-sensical doctor is invited to review the risks
and remind Junior that the social benefits of jocking it up (i.e., excelling on team sports and looking a
lot better than most other boys nowadays) can be obtained about as easily
without using steroids. Common sense triumphant. I'd much
rather have my own son express an interest in trying steroids under supervision
than being a "party animal", smoking tobacco, or getting a motorcycle.
The politics of anabolic steroid use, and attempts at control: NEJM 321: 1042, 1989; the latter have historically
been a joke (older review
NEJM 322: 775, 1990; Olympics Nature 407: 124, 2000).
Despite the anecdotal evidence, there are no good studies correlating dosage, drug type, and effect. Physicians are finally getting up the courage to talk about supplementing older men with synthetic androgens, just as we've
supplementing older women with estrogens for decades to relieve menopausal problems
and control osteoporosis (Sci. Am. 272(2): 76, Feb. 1995). The "horror stories" seem to be mostly from people who took very high doses of these potent substances (Psych. Clin. N.A.
21: 829, 1998.) Life's a matter of weighing benefits (to yourself and those around you) against risks (to yourself and those around you). It's your body and your mind. At present, speaking
as a physician, your instructor recommends against you or your patients taking anabolic steroids to "stud up".
{14612} skeletal muscle, normal
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
Pathology Education Instructional Resource -- U. of Alabama; includes a digital library
Houston Pathology -- loads of great pictures for student doctors
Pathopic -- Swiss site; great resource for the truly hard-core
Syracuse -- pathology cases
Walter Reed -- surgical cases
Alabama's Interactive Pathology Lab
"Companion to Big Robbins" -- very little here yet
Alberta Pathology Images --hard-core!
Cornell
Image Collection -- great site
Bristol Biomedical
Image Archive
EMBBS Clinical Photo Library
Chilean Image Bank -- General Pathology -- en Español
Chilean Image Bank -- Systemic Pathology -- en Español
Connecticut
Virtual Pathology Museum
Australian
Interactive Pathology Museum
Semmelweis U., Budapest -- enormous pathology photo collection
Iowa Skin Pathology
Loyola
Dermatology
History of Medicine -- National Library of Medicine
KU Pathology Home
Page -- friends of mine
The Medical Algorithms Project -- not so much pathology, but worth a visit
National Museum of Health & Medicine -- Armed Forces Institute of Pathology
Telmeds -- brilliant site by the medical students of Panama (Spanish language)
U of Iowa Dermatology Images
U Wash Cytogenetics Image Gallery
Urbana Atlas of Pathology -- great site
Visible Human Project at NLM
WebPath: Internet Pathology
Laboratory -- great siteEd Lulo's Pathology Gallery
Bryan Lee's Pathology Museum
Dino Laporte: Pathology Museum
Tom Demark: Pathology Museum
Dan Hammoudi's Site
Claude Roofian's Site
Pathology Handout -- Korean student-generated site; I am pleased to permit their use of my cartoons
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
St.
Jude's Ranch for Children
I've spent time there and they are good. Write "Thanks
Ed" on your check.
PO Box 60100
Boulder City, NV 89006--0100
More of my notes
My medical students
Clinical Queries -- PubMed from the National Institutes of Health. Take your questions here first.
HealthWorld
Yahoo! Medline lists other sites that may work well for you

We comply with the
HONcode standard for health trust worthy
information:
verify
here.
 Musculoskeletal Pathology
Musculoskeletal Pathology
Virginia Commonwealth U.
Great pictures
 Musculoskeletal Disease
Musculoskeletal Disease
Mark W. Braun, M.D.
Photomicrographs
QUIZBANK Muscle & soft tissue (all except #'s 55-61)
{14614} skeletal muscle, histology
{20723} skeletal muscle, histology
{44101} skeletal muscle, ultrastructure
{44116} mitochondrion & sliding filaments
{44110} section of myofilaments
{18639}
{18643}
{18644}
{18665}

Grade I: Just stretched.
Grade II: Partly torn
Grade III: Fully torn
Grade I: Micro-tears, tender at muscle-tendon junction
Grade II: Partial tear, examiner can feel it
Grade III: Muscle separated from tendon
* They
stain dark with ATPase at acid pH, and dark with NADH (a mitochondria marker,
of course).
* They stain dark with
ATPase at alkaline pH, and light with NADH.
{14418} normal; ATPase stain with type I fibers dark, type II fibers light
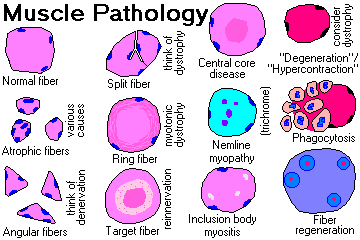
 Type II muscle atrophy
Type II muscle atrophy
Wash. U., St. Louis
Illustrated notes
 Duchenne's muscular dystrophy
Duchenne's muscular dystrophy
Autopsy view of calf
KU Collection
 Chronic partial denervation
Chronic partial denervation
Wash. U., St. Louis
Illustrated notes
 Neurogenic atrophy
Neurogenic atrophy
Tom Demark's Site
 Split fibers is a misnomer. Fibers are clefted, with nuclei along the cleft. What has probably happened is either that (1) some regenerating myoblasts have not fused, or (2) we have had longitudinal division of a muscle cell to make
two. That was supposed to be impossible, but ask Arnold Schwarzenegger....
Split fibers is a misnomer. Fibers are clefted, with nuclei along the cleft. What has probably happened is either that (1) some regenerating myoblasts have not fused, or (2) we have had longitudinal division of a muscle cell to make
two. That was supposed to be impossible, but ask Arnold Schwarzenegger....
 Myasthenia gravis
Myasthenia gravis
Wash. U., St. Louis
Illustrated notes
MUSCLE CHANGES IN PERIPHERAL NERVE DISEASE
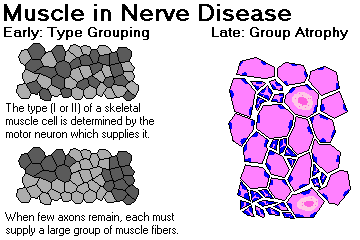
{14429} denervation-reinnervation pattern with type grouping; compare normal
{14418}
{14375} Werdnig-Hoffman disease
{14403} Werdnig-Hoffman disease
 Spinal muscular atrophy
Spinal muscular atrophy
Wash U, St. Louis
{14377} Kugelberg-Welander disease (Gower's sign like in Duchenne's; see below)
{14407} Charcot-Marie-Tooth disease, kid
{14429} type grouping, this was a case of Charcot- Marie-Tooth disease
{14446} Duchenne's, kid
{14449} Duchenne's; Gower's sign
{14408} Duchenne's, early, dark-staining fibers are dying
{14411} Duchenne's, classic histopathology
{09036} Duchenne's, biopsy; trichrome stain (i.e., muscle red,
fibrosis blue)
 Dystrophin and related proteins
Dystrophin and related proteins
Wash. U., St. Louis
Illustrated notes
 Duchenne's
Duchenne's
Wash U, St. Louis
{14467} Becker's (I think; pseudohypertrophy)
{14470} Becker's (I think; pseudohypertrophy)
 Becker's
Becker's
Wash U, St. Louis
{27274} Emery-Dreifuss
{27277} Emery-Dreifuss
{27280} Emery-Dreifuss
{27283} Emery-Dreifuss
{27352} Emery-Dreifuss
 Emery-Dreifuss
Emery-Dreifuss
Wash U, St. Louis
{14485} myotonic dystrophy
{14488} myotonic dystrophy
{14491} myotonic dystrophy
 Facioscapulohumeral dystrophy
Facioscapulohumeral dystrophy
Wash U, St. Louis
{14385} limb-girdle dystrophy, histology
 Fiber type disproportion / type 1 fiber atrophy
Fiber type disproportion / type 1 fiber atrophy
Wash U, St. Louis
 Centronuclear myopathy with vacuoles
Centronuclear myopathy with vacuoles
Electron micrographs
VCU Pathology
 Glycogen
Glycogen
Wash. U., St. Louis
Illustrated notes
* Pathologists today also stain for cytochrome oxidase; patchy areas with
deficient staining strongly suggest mitochondrial myopathy. Review Am. J. Clin. Path. 116:
326, 2001.
{14436} mitochondrial myopathy; mitochondrial clusters are dark b;ie
 Mitochondrial myopathy
Mitochondrial myopathy
Electron micrographs
VCU Pathology
* Future pathologists: Gomori trichrome accentuates the
red-purple staining. The "rods" are not exactly pathognomonic, but dominate the picture in this entity. See Hum. Path. 21: 77, 1990. One of the genes is tropomyosin 3, another is actin (Nat. Genet. 23: 208, 1999).
{14378} rod body ("nemaline") myopathy
{14379} rod body ("nemaline") myopathy, Gomori trichrome stain
 Nemaline myopathy
Nemaline myopathy
Wash U, St. Louis
{27331} central core disease; patient (no really diagnostic features visible)
{27352} central
core disease; patient (no really diagnostic features visible)
{27325} central core disease, patient
 Central Tubular Disease
Central Tubular Disease
Wash U, St. Louis
 Lovastatin / niacin rhabdomyolysis
Lovastatin / niacin rhabdomyolysis
Pittsburgh Pathology Cases
* This is probably the same disease as "progressive fibrodysplasia ossificans".
 Myositis ossificans
Myositis ossificans
Pittsburgh Pathology Cases
 Ipecac myopathy
Ipecac myopathy
Pittsburgh Pathology Cases
{08215} trichinosis
{08288} trichinosis
{15750} trichinosis
{24498} trichinosis
{05780} polymyositis, histology
{09039} polymyositis, histology
{14352} polymyositis, histology
{14356} polymyositis, histology; obvious perifascicular atrophy
{14358} polymyositis, histology; obvious perifascicular atrophy
{14433} polymyositis, really bad
inflammation
{29504} polymyositis, histology, showing regeneration
HIV-lipodystrophy syndrome is a well-known problem faced by patients on long-term
retroviral therapy. No one really knows how it happens. It features redistribution of
bodyfat from the subcutaneous tissues into the skeletal muscles, and development of
insulin resistance. The mainstay of therapy is intensive exercise, both aerobic and
resistance; metformin may be helpful.
 Childhood dermatomyositis
Childhood dermatomyositis
Wash U, St. Louis
 Adult dermatomyositis
Adult dermatomyositis
Wash. U., St. Louis
Illustrated notes
Thick filament myopathy: Myosin, but not actin, disappears (Neurology 55: 854, 2000). Patients
are usually on glucocorticoids and/or NJM blockers.
 Myosin loss
Myosin loss
Wash U, St. Louis
{14503} myotonia congenita, older patient with atrophy
{14506} myotonia congenita, older patient with atrophy
Patients may appear to have some other neuromuscular disease, or to have
fibromyalgia,
or to be "crocks", but they have palpable tender nodules / "trigger points" within their muscles.
You can feel a tautness in the muscle, which twitches on tweaking
and grows sore (local / referred)
on pressure.
* The problem was that the bacteria that produced
the tryptophan were genetically-engineered to make preposterously large amounts.
Common sense would suggest there would be unwholesome by-products.
Showa Denko, the Japenese chemical firm that had previously produced
the world's second-largest outbreak of deaths from mercury pollution,
didn't bother checking for or removing the impurities. For reasons
of political correctness, all tryptophan supplements were banned as a result,
and the anti-biotechnology community has made tremendous political capital
off the fiasco.
 Rhabdomyoma
Rhabdomyoma
Pittsburgh Illustrated Case
{09006} alveolar rhabdomyosarcoma; very undifferentiated tumor
{25305} sarcoma botryoides with cambium layer
 Rhabdomyosarcoma
Rhabdomyosarcoma
WebPath Photo
 Chondroitin sulfate C deficiency myopathy
Chondroitin sulfate C deficiency myopathy
Wash. U., St. Louis
Illustrated notes
 Anti-decorin (BJ) antibody
Anti-decorin (BJ) antibody
Wash. U., St. Louis
Illustrated notes
 Hemophagocytic lymphohistiocytosis
Hemophagocytic lymphohistiocytosis
Wash. U., St. Louis
Illustrated notes
 Inclusion Body Myositis
Inclusion Body Myositis
Wash. U., St. Louis
Illustrated notes
 Macrophage Myositis -- vaccine adjuvant?
Macrophage Myositis -- vaccine adjuvant?
Wash. U., St. Louis
Illustrated notes
 Mitochondrial dysfunction / cytochrome oxidase
Mitochondrial dysfunction / cytochrome oxidase
Wash. U., St. Louis
Illustrated notes
 Neonatal perifascicular myopathy
Neonatal perifascicular myopathy
Wash. U., St. Louis
Illustrated notes
 Paraneoplastic necrotizing myositis
Paraneoplastic necrotizing myositis
Wash. U., St. Louis
Illustrated notes
 Small-vessel muscle disease
Small-vessel muscle disease
Wash. U., St. Louis
Illustrated notes
 Medium-vessel muscle disease
Medium-vessel muscle disease
Wash. U., St. Louis
Illustrated notes
 Hypokalemic periodic paralysis
Hypokalemic periodic paralysis
Wash. U., St. Louis
Illustrated notes
 Internal NADH architecture
Internal NADH architecture
Wash. U., St. Louis
Illustrated notes
 Myofibrillar / desmin storage
Myofibrillar / desmin storage
Wash. U., St. Louis
Illustrated notes
 Phosphorylase deficiency
Phosphorylase deficiency
Wash. U., St. Louis
Illustrated notes
 Congenital muscular dystrophy
Congenital muscular dystrophy
Wash. U., St. Louis
Illustrated notes
 Autophagy in muscular dystrophy
Autophagy in muscular dystrophy
Wash. U., St. Louis
Illustrated notes
 Distal myopathy with vacuoles
Distal myopathy with vacuoles
Wash. U., St. Louis
Illustrated notes
 Oculopharyngeal muscular dystrophy
Oculopharyngeal muscular dystrophy
Wash. U., St. Louis
Illustrated notes

Action hero -- 1950's
Kirk Douglas as "Spartacus"

Action hero -- ContemporarySports do not build character. They reveal it.
-- Heywood Hale Broun, TV commentator
 Aerobic
training ("getting in shape") involves repetitively forcing the muscle to maximum metabolic demands. Aerobic exercise: Science 276: 1325, 1997.
Aerobic
training ("getting in shape") involves repetitively forcing the muscle to maximum metabolic demands. Aerobic exercise: Science 276: 1325, 1997.
* There will eventually be biotech products for bodybuilders and for reversing
cachexia, but first there will be a bunch of scams based on the above work.
* Of course, it was Virchow who demonstrated that muscles grow by hypertrophy rather than by hyperplasia.
* A new study confirms my impression that men who work-out think and act about the same as ordinary guys. There is a subset that the authors suggest calling "muscle dysmorphia", the guy who works out compulsively, is heavily-
muscled, but won't take his shirt off because he thinks people will say he's too small (Am. J. Psych. 157: 1291, 2000).
 Johnny Weissmuller as Tarzan
Johnny Weissmuller as Tarzan
BEFORE working out became popular
Weissmuller was also a real athlete.
 Mel Gibson, ~ age 50
Mel Gibson, ~ age 50
Cast as an ordinary guy, AFTER
working out became popular
 Douglas Fairbanks
Douglas Fairbanks
Cast as an action hero BEFORE
working out became popular
 Bruce Willis
Bruce Willis
Cast as a psychologist AFTER
working out became popular
 Eroll Flynn
Eroll Flynn
Cast as an action hero BEFORE
working out became popular
 Kirk Douglas
Kirk Douglas
Cast as a an action hero BEFORE
working out became popular
* In
one study, the blood pressure in a bodybuilder lifting his maximum with a closed glottis was reported to rise to an average of 311/284, and one muscle guy got it as high as 370/360. (I wonder about the measurement techniques...
Arch. Phys. Med. Rehab. 76: 457, 1995).
 Mr. Universe Contest, 1953
Mr. Universe Contest, 1953
Before the steroid era
Sean Connery is 4th from left
{14613} skeletal muscle, normal
{14614} skeletal muscle, normal
{14615} skeletal muscle (high power), normal
{14616} skeletal muscle cross section, normal
{14617} skeletal muscle cross section, normal
{14618}
smooth muscle, longitudinal section
{14619} smooth muscle, longitudinal section
{14620} smooth muscle, normal
{14621} smooth muscle (cross & longit. section)longitudinal and cross sections
{14622} cardiac muscle, normal
{14623} cardiac muscle, normal
{14624} cardiac muscle intercalated disks
{14625} cardiac muscle intercalated disks
{14955} tropomyosin, cell biology
{14956} tropomyosin, cell biology
{14957} myosin actin, cell biology
{14958} myosin actin, cell biology
{15110} muscle, cardiac
{15226} tongue, skeletal muscle
{15240} esophagus, skeletal muscle

{15263} duodenum, muscle
{15296} trachea, trachealis muscle
{20722} muscle, skeletal
{20723} muscle, skeletal
{20724} muscle, skeletal
{20725} muscle, skeletal
{20726} muscle, smooth
{20727} muscle, smooth
{20728} muscle, cardiac
{20729} muscle, cardiac
{20905} trachea, trachealis muscle
{20906} trachea, trachealis muscle
{21890} ocular muscle, NADH stain - normal
{35951} muscle spindle, normal
| Visitors to www.pathguy.com reset Jan. 30, 2005: |
Ed says, "This world would be a sorry place if
people like me who call ourselves Christians
didn't try to act as good as
other
good people
."
Prayer Request
 Teaching Pathology
Teaching Pathology
PathMax -- Shawn E. Cowper MD's
pathology education links
Ed's Autopsy Page
Notes for Good Lecturers
Small Group Teaching
Socratic
Teaching
Preventing "F"'s
Classroom Control
"I Hate Histology!"
Ed's Physiology Challenge
Pathology Identification
Keys ("Kansas City Field Guide to Pathology")
Ed's Basic Science
Trivia Quiz -- have a chuckle!
Rudolf
Virchow on Pathology Education -- humor
Curriculum Position Paper -- humor
The Pathology Blues
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |