Ed Friedlander, M.D., Pathologist
scalpel_blade@yahoo.com


Cyberfriends: The help you're looking for is probably here.
Welcome to Ed's Pathology Notes, placed here originally for the convenience of medical students at my school. You need to check the accuracy of any information, from any source, against other credible sources. I cannot diagnose or treat over the web, I cannot comment on the health care you have already received, and these notes cannot substitute for your own doctor's care. I am good at helping people find resources and answers. If you need me, send me an E-mail at scalpel_blade@yahoo.com Your confidentiality is completely respected.
 DoctorGeorge.com is a larger, full-time service.
There is also a fee site at myphysicians.com,
and another at www.afraidtoask.com.
DoctorGeorge.com is a larger, full-time service.
There is also a fee site at myphysicians.com,
and another at www.afraidtoask.com.
Translate this page automatically
 |
With one of four large boxes of "Pathguy" replies. |
 I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
I'm still doing my best to answer
everybody.
Sometimes I get backlogged,
sometimes my E-mail crashes, and sometimes my
literature search software crashes. If you've not heard
from me in a week, post me again. I send my most
challenging questions to the medical student pathology
interest group, minus the name, but with your E-mail
where you can receive a reply.
Numbers in {curly braces} are from the magnificent Slice of Life videodisk. No medical student should be without access to this wonderful resource. Someday you may be able to access these pictures directly from this page.
Also:
Medmark Pathology -- massive listing of pathology sites
Freely have you received, freely give. -- Matthew 10:8. My
site receives an enormous amount of traffic, and I'm
handling about 200 requests for information weekly, all
as a public service.
Pathology's modern founder,
Rudolf
Virchow M.D., left a legacy
of realism and social conscience for the discipline. I am
a mainstream Christian, a man of science, and a proponent of
common sense and common kindness. I am an outspoken enemy
of all the make-believe and bunk which interfere with
peoples' health, reasonable freedom, and happiness. I
talk and write straight, and without apology.
Throughout these notes, I am speaking only
for myself, and not for any employer, organization,
or associate.
Special thanks to my friend and colleague,
Charles Wheeler M.D.,
pathologist and former Kansas City mayor. Thanks also
to the real Patch
Adams M.D., who wrote me encouragement when we were both
beginning our unusual medical careers.
If you're a private individual who's
enjoyed this site, and want to say, "Thank you, Ed!", then
what I'd like best is a contribution to the Episcopalian home for
abandoned, neglected, and abused kids in Nevada:
My home page
Especially if you're looking for
information on a disease with a name
that you know, here are a couple of
great places for you to go right now
and use Medline, which will
allow you to find every relevant
current scientific publication.
You owe it to yourself to learn to
use this invaluable internet resource.
Not only will you find some information
immediately, but you'll have references
to journal articles which you can obtain
by interlibrary loan, plus the names of
the world's foremost experts and their
institutions.
Alternative (complementary) medicine has made real progress since my
generally-unfavorable 1983 review linked below. If you are
interested in complementary medicine, then I would urge you
to visit my new
Alternative Medicine page.
If you are looking for something on complementary
medicine, please go first to
the American
Association of Naturopathic Physicians.
And for your enjoyment... here are some of my old pathology
exams
for medical school undergraduates.
I cannot examine every claim which my correspondents
share with me. Sometimes the independent thinkers
prove to be correct, and paradigms shift as a result.
You also know that extraordinary claims require
extraordinary evidence. When a discovery proves to
square with the observable world, scientists make
reputations by confirming it, and corporations
are soon making profits from it. When a
decades-old claim by a "persecuted genius"
finds no acceptance from mainstream science,
it probably failed some basic experimental tests designed
to eliminate self-deception. If you ask me about
something like this, I will simply invite you to
do some tests yourself, perhaps as a high-school
science project. Who knows? Perhaps
it'll be you who makes the next great discovery!
Our world is full of people who have found peace, fulfillment, and friendship
by suspending their own reasoning and
simply accepting a single authority which seems wise and good.
I've learned that they leave the movements when, and only when, they
discover they have been maliciously deceived.
In the meantime, nothing that I can say or do will
convince such people that I am a decent human being. I no longer
answer my crank mail.
This site is my hobby, and I presently have no sponsor.
This page was last updated February 6, 2006.
During the ten years my site has been online, it's proved to be
one of the most popular of all internet sites for undergraduate
physician and allied-health education. It is so well-known
that I'm not worried about borrowers.
I never refuse requests from colleagues for permission to
adapt or duplicate it for their own courses... and many do.
So, fellow-teachers,
help yourselves. Don't sell it for a profit, don't use it for a bad purpose,
and at some time in your course, mention me as author and KCUMB as my institution. Drop me a note about
your successes. And special
thanks to everyone who's helped and encouraged me, and especially the
people at KCUMB
for making it possible, and my teaching assistants over the years.
Whatever you're looking for on the web, I hope you find it,
here or elsewhere. Health and friendship!
 I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
I am presently adding clickable links to
images in these notes. Let me know about good online
sources in addition to these:
Pathology Education Instructional Resource -- U. of Alabama; includes a digital library
Houston Pathology -- loads of great pictures for student doctors
Pathopic -- Swiss site; great resource for the truly hard-core
Syracuse -- pathology cases
Walter Reed -- surgical cases
Alabama's Interactive Pathology Lab
"Companion to Big Robbins" -- very little here yet
Alberta
Pathology Images --hard-core!
Cornell
Image Collection -- great site
Bristol Biomedical
Image Archive
EMBBS Clinical
Photo Library
Chilean Image Bank -- General Pathology -- en Español
Chilean Image Bank -- Systemic Pathology -- en Español
Connecticut
Virtual Pathology Museum
Australian
Interactive Pathology Museum
Semmelweis U.,
Budapest -- enormous pathology photo collection
Iowa Skin
Pathology
Loyola
Dermatology
History of Medicine -- National Library of Medicine
KU
Pathology Home
Page -- friends of mine
The Medical Algorithms Project -- not so much pathology, but worth a visit
National Museum of Health & Medicine -- Armed Forces Institute of Pathology
Telmeds -- brilliant site by the medical students of Panama (Spanish language)
U of
Iowa Dermatology Images
U Wash
Cytogenetics Image Gallery
Urbana
Atlas of Pathology -- great site
Visible
Human Project at NLM
WebPath:
Internet Pathology
Laboratory -- great siteEd Lulo's Pathology Gallery
Bryan Lee's Pathology Museum
Dino Laporte: Pathology Museum
Tom Demark: Pathology Museum
Dan Hammoudi's Site
Claude Roofian's Site
Pathology Handout -- Korean student-generated site; I am pleased to permit their use of my cartoons
Estimating the Time of Death -- computer program right on a webpage
Pathology Field Guide -- recognizing anatomic lesions, no pictures
St.
Jude's Ranch for Children
I've spent time there and they are good. Write "Thanks
Ed" on your check.
PO Box 60100
Boulder City, NV 89006--0100
More of my notes
My medical students
Clinical
Queries -- PubMed from the National Institutes of Health.
Take your questions here first.
HealthWorld
Yahoo! Medline lists other sites which may work well for you

We comply with the
HONcode standard for health trust worthy
information:
verify
here.
 Tulane Pathology Course
Tulane Pathology Course
Great for this unit
Exact links are always changing
 "Heme-Onc Pathology"
"Heme-Onc Pathology"
Virginia Commonwealth U.
Great pictures
Enough normoblasts not being made
Spherocytosis: Spherocytes on peripheral smear; Increased MCHC (hyperchromasia)
Paroxysmal nocturnal hemoglobinuria: Positive Ham test (acid hemolysis)
Enzyme deficiencies: Heinz bodies
Abnormal hemoglobins: Target cells
Sickle cell disease: Sickled cells (drepanocytes)
Hemoglobin C disease: Hemoglobin C crystals
Hemoglobin SC disease: Hemoglobin SC ("birds in flight") crystals
Immune hemolysis: Spherocytes; Positive direct Coombs' test. (Savvy labs now give you a free Coombs test if you're found to have unexplained elevated reticulocytes: Am. J. Clin. Path. 124: 129, 2005).
Some mechanical hemolysis (clostridia, burns, prosthetic heart valves, microangiopathy): Schistocytes and other fragments on peripheral smear
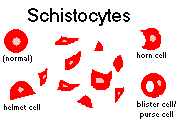
Acute hemorrhage: Increased reticulocytes
Enough hemoglobin not being made: Decreased MCV (microcytosis); Decreased MCHC (hypochromia)
Not enough usable iron: Decreased serum iron
Actual iron deficiency (none stored): Very low serum ferritin; Zero stainable marrow iron stores; Increased total iron binding capacity; *increased transferrin receptors (new serum marker for absolute iron deficiency which avoids some pitfalls of previous assays)
Free erythrocyte protoporphyrin: Screening tool for iron deficiency, best in kids. Why?
Anemia of inflammation / sideroblastic anemias: Increased serum ferritin; Normal total iron binding capacity
Sideroblastic anemia: Dimorphic population (some forms); Ringed sideroblasts in marrow
Lead poisoning: Coarse basophilic stippling
Thalassemias: Coarse basophilic stippling; Pancake cells
Enough normoblasts not being made: Decreased reticulocytes
Not enough nucleic acid being made: Increased MCV (macrocytosis); Hypersegmented PMN's
B12 deficiency: Low serum B12; Perform a Schilling test
Classic pernicious anemia: Schilling test becomes normal on addition of extrinsic factor
Folic acid deficiency: Low red cell folate
Infiltrative disease of bone marrow: Teardrop red cells
|
|
|
|
|
|
/ANK
Clinical Hematology ("Hematology Lab")
Blood Bank (if and only if we have a chance to cover transfusion medicine in this unit)
Blood & Lymph #'s 1-132, 140-177
INTRODUCTION

Workup of anemia in adults: Mayo Clin. Proc. 78: 1274, 2003. In the newborn: Ped. Clin. N.A. 51: 1087, 2004. What to do generally if there's a CBC abnormality: Mayo Clin. Proc. 80: 923, 2005.
Review the following terms:
Hemoglobin
Hematocrit
Red cell indices (mean corpuscular volume, mean corpuscular hemoglobin concentration, mean corpuscular hemoglobin)
Do you remember all those hemoglobins?
Hemoglobin is four globin chains plus four heme units (porphyrin plus iron):
2α + 2β = Hgb A
(α2 β2A) 96% in normal adults
2α + 2 δ = Hgb A2
(α2 δ2) 3% in normal adults
2α + 2 γ = Hgb F
(α2 γ2) 1% in normal adults
(Hgb F is the main hemoglobin in the fetus, and remains abundant until the child is two years old.)
Do you remember the hemoglobins seen only in disease?
Wrong ways of combining normal chains:
4β = Hgb H (β4)
4 γ = Hgb Bart's (γ4)
Mutations:
2α + 2βS = Hgb S (α2βS2)
2α + 2βC = Hgb C (α2βC2)
2α + 2 β-δ Lepore = Hgb Lepore(α2 β-δ2)
And about 300 other, less common, variants. (Some cause problems, some don't.)
ANEMIAS OVERSIMPLIFIED (see also Lancet 355: 1169 & 1260, 2000)
Anemia is any reduction below normal limits of the total circulating red cell mass.
All anemias except the anemia of acute blood loss are detected by your discovery of decreased hematocrit and/or decreased hemoglobin.
(Hemodilution from excess fluids can occasionally lower hemoglobin and hematocrit in the absence of anemia.)
Acute anemia (i.e., blood loss) produces shock. (Hemoglobin and hematocrit stay normal or near-normal until plasma volume is restored.)
Chronic anemia requires increased cardiac output and eventually may produce hypoxia, weakness, malaise, easy fatiguability, koilonychia, fatty change in myocardium.
ANEMIAS OF BLOOD LOSS
Acute blood loss:
Remember that hematocrit and hemoglobin will remain normal until plasma volume is restored (hours to days.)
The bone marrow can increase erythropoiesis to three times normal within a day or so.
Chronic blood loss:
Anemia usually develops only when iron stores run out, i.e., iron deficiency anemia results.
The bone marrow can increase erythropoiesis to eight times normal in the face of chronic bleeding or hemolysis.
Remember that hemorrhage is much commoner than hemolysis!
HEMOLYTIC ANEMIAS: INTRODUCTION
Many anemias are due, in whole or part, to premature destruction of red blood cells within blood vessels (intravascular hemolysis, as in DIC, or when RBC's are sensitized to complement or mechanically injured) or in the RE system (extravascular hemolysis, as when RBC's are too stiff or fragile or are altered immunologically). Easy update: Am. Fam. Phys. 69: 2599, 2004.
If the capacity of the erythroid (red-cell producing) bone marrow to produce red cells is exceeded (it can increase output up to eight times normal), anemia will result.
Regardless of cause, ongoing hemolysis will result in several pathophysiologic changes:
(the gut knows about the increased erythropoiesis and absorbs more iron; if hemolysis is the only problem, this is seldom serious)
(this is a measure of the percentage of very young red blood cells; do this FIRST in your workup of anemia. Savvy labs now do it for you on any patient without a known anemia: Am. J. Clin. Path. 124: 129, 2005.

(in children, this produces thickened diploe of the skull, with a "crewcut" pattern)
If RBC's are being destroyed in the spleen (the usual site of extravascular hemolysis), it will usually be large, and is often iron-loaded. All about spleens in the immune and non-immune hemolytic anemias: Mayo Clin. Proc. 68: 757, 1993.
HEREDITARY SPHEROCYTOSIS
This is a relatively common autosomal dominant hemolytic syndrome (1/5000 people of northern
European stock).
Anemia is moderately severe, with hemoglobin around 9.
Poor binding of protein 4.1 to spectrin results in a defective erythrocyte cytoskeleton. This produces
spherical RBC's which get destroyed in spleen.
Spherocytes are easy to identify on a smear of peripheral blood because they lack the central pallor
of biconcave RBC's.
In addition, the mean corpuscular hemoglobin (MCHC) is high in this disorder because the spleen
nibbles bits of membrane off the surfaces of RBC's that make it through.
The inadequate cytoskeleton allows the RBC's to rupture easily when placed in mildly hypotonic
solution (increased osmotic fragility). All but the youngest RBC's are destroyed while passing
through the splenic sinusoids.
Hereditary spherocytosis patients may have hemolytic and/or aplastic crises, like sickle-cell disease
patients.
Treatment is splenectomy, which results in a great subjective benefit and a normal hemoglobin
(though some hemolysis continues.)
In hereditary elliptocytosis
("hereditary ovalocytosis"), the mutation is different, the cells are oval, but
the picture is the same or milder.
* Variation on the theme: the rare "hereditary pyropoikilocytosis" is a hemolytic anemia with a
mutant spectrin which won't stick to itself and gets degraded too rapidly. The cells have bizarre
shapes, the anemia is obvious at birth, but the prognosis is excellent (Am. J. Dis. Child. 147: 93,
1993). The molecular biology: J. Clin. Invest. 89: 892, 1992; Blood 82: 1652,
1993, others.
HEMOLYTIC DISEASE DUE TO ERYTHROCYTE ENZYME DEFECTS (review: Blood 64:
583, 1984).
Inherited disorders of enzymes in the hexose monophosphate shunt or glutathione enzyme systems in
erythrocytes result in oxidative damage to RBC's.
Deficiencies of each enzyme may be mild or severe, the thus the clinical pictures are widely
variable.
RBC's cannot generate the reducing power (i.e., reduced glutathione) required to repair oxidative
damage to their hemoglobin and membranes.
Masses of oxidized, denatured hemoglobin form in the cells and are visible by special staining
procedures as "Heinz bodies".
* Heinz bodies, when numerous, produce "golf ball" red cells.
The spleen futilely pits these out, making "bite cells." These are excessively fragile and get
destroyed even more readily, making the anemia worse.
Glucose-6-phosphate dehydrogenase deficiency is the best known of these disorders.
This is X-linked and very common in certain populations. (Ten percent of US black men have it.)
In the commonest African variant, only the older RBC's are seriously deficient. In the commonest
Mediterranean variant, there is little good G6PD in any RBC.
Victims must avoid certain drugs (the basic "treatment", much better than trying to re-reduce the
patients' hemoglobin).
This was a serious problem for black servicemen taking antimalarials in Vietnam. Sulfas,
nitrofurantoin, and even aspirin can be hazardous for these people, depending on how badly deficient
they are.
(Susceptibility to fava beans requires a second inborn error of metabolism.)
If the patient also has Gilbert's, severe neonatal jaundice results
(Proc. Nat. Acad. Sci. 94: 12128, 1997).
Deficiency of pyruvate kinase (for anaerobic glycolysis) is a very common Amish autosomal
recessive birth defect. (Victims are of northern European ancestry.) There are other mutations as
well. Some molecular biology: Blood 82: 1652, 1993; Blood 89: 1793, 1997.
There is not enough energy to run the RBC membrane sodium pump, so the cells eventually
undergo osmotic lysis.
Because these people have so much 2,3-DPG in their erythrocytes, they tolerate their anemia very
well.
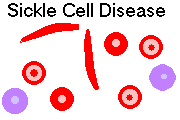
SICKLE CELL DISEASE (Am. J. Med. Sci. 3122: 166, 1996;
Ped. Clin. N.A. 49: 1193, 2002)
Sickle cell substitution of valine for glutamine at the sixth position of the β chain (βS). Two
α chains plus two βS chains makes HgbS.
Eight percent of blacks in the US are carriers, and 1 child in 600 is affected.
Deoxygenation results in tactoid formation ("crystallization", "gelation") of HgbS. This forms
sickle-shaped cells, and results in stasis (sludging), vaso-occlusive phenomena, and hemolysis.
Sickling of a cell is reversible until the tactoids wreck the cell membrane ("how" involves spectrin
tetramers dissociating and re-associating: Blood 81: 522, 1993). Then it's irreversible and the cell
eventually gets lysed. Life span is twenty days.
Dehydration increases MCHC and promotes sickling.
Hgb F effectively prevents sickling, so patients don't sickle until they are around two years old and
no longer have any Hgb F.
Hgb A inhibits sickling, so heterozygotes (Hgb AS) do not have much trouble with sickling at usual
oxygen tensions.
Hgb C does not inhibit sickling so well as Hgb A. Hgb SC mixed heterozygotes do sickle, though it
is not so severe as Hgb SS homozygotes, and the spleen is typically lost later in childhood (Blood
85: 2238, 1995).
When oxygen tensions are low, sickled cells tend to stick tight to one another. This doesn't help
things. Nobody really understands why this happens; some people think the sickled cells grow tiny
spikes and stick together like burrs (see Blood 81: 3138, 1993). Somehow
the cells also get a lot stickier to endothelium, probably accounting for a lot
of the strokes and other occlusive phenomena.
Decreased hemoglobin concentration helps prevent sickling. Concurrent iron deficiency anemia or
thalassemia relieves sickling.
Patients with sickle-cell anemia have many problems.
They have a severe, chronic hemolytic anemia with all the associated changes.
Vaso-occlusive complications include leg ulcers, strokes
(mechanisms: Blood 89: 4591, 1997; prevention and treatment Arch. Neuro. 58: 565, 2001), retinal infarctions, priapism (Am. J. Med.
94: 289, 1993), painful bone infarcts (necrosis of the femoral head, etc.), thrombi. One likely
contributing factor is double-stranded RNA, which glues sickled cells to endothelium, which
probably explains why viral infection precipitates these events (Blood 85: 2945, 1995). Handling
vaso-occlusive crisis in the emergency room: South. Med. J. 85: 808, 1992.
Sludging of cells in the spleen ruins it by age 6 ("autosplenectomy"). The major problem then is
vulnerability to pneumococcal infections.
Infections, notably Salmonella osteomyelitis
(and even sepsis: J. Ped. 130: 349, 1997), are common.
"Chest syndrome", with fever, chest pain, a lung infiltrate, and leukocytosis, is a poorly-understood
phenomenon (J. Ped. 123: 272, 1993; Br. Heart J. 69: 536, 1993; Am. J. Med. Sci. 305: 326,
1993; NEJM 342: 1855, 2000; morphine as a cause Clin. Pharm. Ther. 75: 140, 2004). Perhaps infection and fat embolization
both contribute. It's pretty much impossible to tell it from pneumococcal pneumonia or pulmonary infarct,
and it's treated as if it were pneumonia; it remain the leading cause of death
in sicklers.
Hemolytic crises are triggered by exertion, infection, etc., while aplastic crises can result from severe
infection (typically due to parvovirus B19 -- review Blood 103: 422, 2004) or (maybe) folic acid deficiency.
* Future pathologists and radiologists: For some reason, the walls of the
marrow arteries collagenize in sickle cell disease, getting progressively
more striking as the person grows older (Arch. Path. Lab. Med. 128: 634, 2004).
* Survival is improving; the chance of a child with sickle cell disease dying is a bit less than 1% per year
(Blood 103: 402, 2004); the rate of stroke is about the same.
These people often become addicted to opiates, and come to be despised by health-care providers as
"drug seekers" or worse. Stigmatization of sicklers is unfair and
scandalous (BMJ 318: 1585, 1999).
They present the same kind of pain management problems as do cancer
patients, only it is worse, since they live longer. Physicians are just now starting to get wise to this (Ped. Clin. N.A.
47: 699, 2000);
managing it appropriately seems to reduce hospitalization by about half (Ann. Int. Med. 116: 364,
1992; epidural fentanyl is eminently sensible Pediatrics 93: 310, 1994).
About half of sicklers survive to age forty. Other genes modify the severity of the disease, and are
the major influence on survival (NEJM 330: 1639, 1994.
Lately we've discovered zinc deficiency (urinary loss? impaired GI absorption?)
as a common, serious problem in these people, resulting in reversible drops
in some lymphocyte populations (J. Clin. Lab. Invest. 130: 116, 1997).
Sickle cell carriers (heterozygotes, "sickle cell trait", Hgb AS) trait have about 40% Hgb S. It is
asymptomatic unless the patient goes to a high altitude (i.e., un-pressurized aircraft, too little oxygen
in the anesthetic mixture, etc.), undergoes intensive physical training
when out of shape or in the heat or whatever (Am. Fam. Phys. 54:
237, 1997; both the above are potential causes of sudden death), or develops hematuria.
As you recall, heterozygotes are relatively protected against falciparum malaria, which is probably
why hemoglobin S is so common in Africa. However, the protection is by no means absolute,
and malaria remains a major killer of children with sickle-cell disease in Africa: Arch. Dis. Child. 89:
572, 2004.
You will learn cost-effective screening procedures for sickle cell disease and trait later in your
career.
Screening newborns for sickle cell disease allows early administration of pneumococcal vaccine, a
potentially life-saving intervention. For black newborns, the extra cost is only $3100 more per life
saved than not screening (J. Ped. 118: 546, 1991).
* Because anyone can check the wrong box, we screen all newborns. There's a fallacy in the above
article ("$450 billion per life saved screening low-prevalence non-black populations").
* Diagnosing sickle cell disease in the unborn at 10 weeks using PCR on Mom's blood rather than
amniocentesis: Nature Genetics 14: 264, 1996.
Therapy for the hemoglobinopathies is so-so nowadays.
Cord-blood allografts from HLA-identical newborn sibs
followed by administration of growth factors
have cured sickle cell disease (J. Ped. 128: 241, 1997).
It is now routine when there is a matched sibling
(Lancet 360: 629, 2002).
Gene therapy is rapidly approaching (West. J. Med. 157: 631, 1992; Proc. Nat. Acad. Sci. 92:
3014, 1995). Treating sickle cell: Med. Clin. N.A. 76: 669, 1992.
Hydroxyurea (Blood 79: 2555, 1992; Medicine 75: 300,
1996) enhances the fetal hemoglobin response and diminishes the
ability of red cells to sickle. The effect can be augmented nicely by erythropoietin (NEJM 328: 73,
1993). * Watch for inhibitors of the gardos channel, which modules
entry of water into the cell; these might well prevent sickling itself.
Chelators seem to be a safe way to prevent iron-overloading in heavily-transfused patients (J.
Lab. Clin. Med. 122: 48, 1993).
* In the early 1990's, Illinois's 1183 sickle cell patients had a median
of 3 hospital admissions yearly and consumed $59,000,000 in two years,
or about $30,000 per patient per year; national numbers
are similar (Pub. Health. Rep. 112:
38 & 44, 1997; they talk about strategies to improve out-of-hospital compliance,
doctors' efficiency).
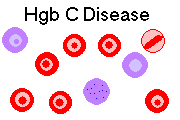
HEMOGLOBIN C DISEASE
Hemoglobin C is another black hemoglobin, almost as common as Hgb S.
People with Hgb CC disease have a mild hemolytic anemia, while people with Hgb SC disease have
a sickle cell disease.
The diagnosis is often obvious from the peripheral smear.
Any patient with Hgb C, even a carrier, will have many target cells on peripheral smear.
Patients with Hgb CC disease have rod-shaped hemoglobin crystals in their red cells (see at low pH),
while patients with Hgb SC disease have irregularly-shaped crystals ("birds in flight," etc.)
HEMOGLOBIN E DISEASE
A Southeast Asian hemoglobin that produces a mild hemolytic disease in homozygotes.
THE THALASSEMIAS ("Cooley's anemia", "Mediterranean blood", etc.)
Disorders with decreased synthesis of a structurally normal globin chain.
The other chain is made in normal quantities. Aggregates of this chain accumulate in the
normoblasts and cause intramedullary hemolysis. (Beta chains are worse than α chains in this
respect.)
I will resist the temptation to talk about the molecular genetics of the thalassemias except in the most
basic terms. Those seeking an appreciation of the range of defects may begin with
Mayo Clin. Proc. 76: 285, 2001; Clin. Chem. 46: 1284, 2000.
The thalassemias, like sickle cell disease, hemoglobin C, hemoglobin E, and G6PD deficiency,
bestow resistance to falciparum malaria on their carriers
(update Am. J. Hum. Genet. 77: 171, 2005).
α-thalassemia: Asian and African genes. Usually the genes are deleted.
There are two genes for the α chain per chromosome, or four genes total. In the various α
thalassemias, one or more are hurt.
One gene hurt ("silent carrier"): No health problem; 3% Hgb Bart's
(four γ chains) at birth, no
Hgb H (four beta chains) as adult.
Two genes hurt ("α thalassemia minor" or "trait"): Red blood cells tend to be small (MCV 82 or
so) but anemia is unusual; 5-10% Hgb Bart's at birth, trace of Hgb H as adult. Seldom noticed.
Three genes hurt ("Hgb H disease"): Hemolytic anemia throughout life; 25% Hgb Bart's at birth;
25% Hgb H as adult. (Hgb H is unstable and these patients have mostly a "bite cell" anemia, Heinz
bodies and all that.)
Four genes hurt ("hydrops fetalis"): Fetus dies as it has only Hgb Bart's, which has an excessive
oxygen affinity. Death is due to congestive heart failure due to anemia, so the fetus dies extremely
edematous. (The other common causes of such a severe anemia
are parvo 19 and Rh incompatibility.)
* The crew at Brown, your lecturer's alma mater, brings a fetus with Bart's hydrops to term and are
going to bone-marrow-transplant.... (Ob. Gyn. 85: 876, 1995). Your lecturer sees this as a prime
example of the "law of inverse care"; you may disagree.
NOTE: It's desirable for a person with sickle cell disease or trait to have deletions of an α gene
or two (why?) See J. Clin. Invest. 88: 1963, 1991.
Beta-thalassemia: Mediterranean genes, mostly
There is one gene for the β chain per chromosome, or two genes total. In the various beta
thalassemias, there is a problem with the mRNA and enough β chains do not get produced.
(Alleles: β0 -- no chains produced; beta+ -- some chains produced, but not enough)
Heterozygotes ("beta thalassemia minor" or "trait"): minimal or no anemia; hypochromia and
microcytosis, target cells, teardrops and basophilic stippling, sometimes with mild anemia. You
may not be able to appreciate either the hypochromia or the microcytosis on smear, because the cells
tend to assume a pancake shape, without central pallor. Increased Hgb F and usually increased Hgb
A2 ("because these have no beta chains").
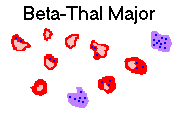
Homozygotes ("beta thalassemia major"): severe anemia beginning in infancy as the baby switches
from Hgb F production. Patients have the stigmata of chronic hemolysis ("crewcut" skull x-ray,
etc.), and little or no Hgb A, with extra Hgb A2 and Hgb F. As they must be transfused repeatedly
and over-absorb iron, they have classically died of iron overload in their teens. The new iron
chelators (deferiprone, desferrioxamine,
others) have been a great help, and now these
people will probably live out a normal lifespan of good quality.
The current major problems with the chelators (especially
deferiprone) have been joint damage,
agranulocytosis and zinc deficiency;
(no surprise): Blood 80: 593, 1992; NEJM 332: 918 & 953, 1995; Br. Heart. J. 73: 486,
1995; Blood 90: 994, 1997. Marrow transplant: Arch. Dis. Child. 66: 517, 1991.
Improved long-term results without bone marrow transplant: Blood 104: 34, 2004.
* "Beta thalassemia intermedia" can result from homozygosity for two not-so-bad beta+ genes. It is a
bad disease (genetic screening Arch. Dis. Child. 72: 408, 1995).
Don't worry about such arcana as "hereditary persistence of fetal hemoglobin",
"δ-thal", etc., etc.
Blood 80: 1582, 1992.
Every once in a while, one or more globin genes can be lost in the myelodysplastic
syndrome, producing an acquired thalassemia (Blood 103: 1518, 2004).
* Mainland China's pathologists develop and begin implementing "preventing
genetics" to eliminate the devastating thalassemias: J. Clin. Path. 57: 517, 2004.
This isn't the place to talk about the "ethical" and "human rights" implications;
the mere fact that we in the United States can do so is a real privilege.
You'll frequently need to distinguish the two great microcytic anemias: thalassemia and iron
deficiency. A variety of formulas exist to give you the first guess. All are based on the fact that
thalassemia cells tend to be smaller with a higher hemoglobin concentration, and iron-deficiency
cells tend to be larger with a lower hemoglobin concentration (Arch. Path. Lab. Med. 116: 84,
1992).
The formulas don't factor hemoglobin E into the picture, since they were developed before our
country was enriched by the Southeast Asian immigration. Easy to remember: Mild microcytic
anemia with near-normal RBC count: Thal minor or hemoglobin E.
PAROXYSMAL NOCTURNAL HEMOGLOBINURIA ("PNH")
Abnormal sensitivity of RBC's to complement-mediated lysis, especially at low pH (i.e., while you're
asleep).
The mechanism has recently become clear. The cells have lost the gene (PIG-A) to make an
inositol-based anchor for a group of surface proteins, including those that confer resistance to lysis
by the body's own complement (NEJM 330: 249, 1994; J. Clin. Invest. 96: 201, 1995; Blood 85:
1640, 1995).
This disease also affects myeloid cells and megakaryocytes, proving it's a stem cell problem. (In
addition, it sometimes turns into aplastic anemia, i.e., it's a
Nowell's law hit. How this happens:
Ann. Int. Med. 136: 534, 2002.
* PNH also pops up quite often
in the setting of prior aplastic anemia, i.e.,
the mutant clone has the growth advantage and fails to undergo apoptosis
like the other red cell precursors; Semin. Hem. 35: 149, 1998.
Additional problems include loss of iron into the urine (eventually producing iron deficiency) and
thromboses in liver and brain veins.
Diagnose it using the "Ham Test" if you can find a lab to do it (newer diagnostic
procedures Am. J. Clin. Path. 114: 798, 2000). Live with it, treat the symptoms, and
hope it remits (i.e., your internal milieu changes somehow and there's selection against the bad
clone, which is fairly common: NEJM 333: 1253, 1995).
AUTOIMMUNE HEMOLYTIC ANEMIAS
Warm antibody AHA:
Extravascular hemolysis resulting from sensitization of RBC's to the patient's own IgG (sometimes
IgA).
A specific cause is found in about one third of cases.
Check for cancers (especially lymphoma-leukemia), systemic lupus (lupus autoimmune hemolysis
Am. J. Med. 108: 198, 2000), drugs.
Mononuclear phagocytes and splenic macrophages first nibble at the sensitized membrane, turning
the RBC's into spherocytes. Eventually the cells are destroyed.
Drug hemolysis mechanisms in warm autoantibody disease:
hapten mechanism (high-dose penicillin type): the patient makes an antibody against drug-red cell
membrane complex
immune complex mechanism (quinine-quinidine type): drug-antibody complexes get absorbed to
innocent bystander RBC's, which are then lysed by complement. Phenacetin and cephalosporin are
also frequently implicated in this type of hemolysis.
autoantibody mechanism ("Aldomet" type): the drug somehow causes one to make antibodies
against one's own Rh antigens (everybody has some Rh antigens, even though Rh negative).
Cold agglutinin AHA
Due to IgM antibodies, which work best below 30.
These monoclonal auto-antibodies appear mysteriously in mycoplasma pneumonia (* anti-I),
infectious mono (* anti-i), others. The anemia, if any, is self-limited and seldom detected.
Chronic cold agglutinin disease is fairly common in lymphoma, or may be idiopathic. (These people
should dress warmly.) Curiously, hemolysis occurs in the liver, not the spleen, in these patients.
Cold hemolysin AHA
The usual disease is paroxysmal cold hemoglobinuria and the auto-antibody is * Donath-Landsteiner
auto-antibody.
The patient goes skiing and falls in the snow; the next time the patient voids, the urine is dark
brown.
Once a famous sign of syphilis, paroxysmal cold hemoglobinuria now it most often follows the flu or
arises mysteriously.
Surprisingly, in today's era of body cooling during cardiopulmonary bypass, the disease
seldom turns up. One case: Ann. Thoracic Surg. 75: 579, 2003.
HEMOLYTIC ANEMIA RESULTING FROM TRAUMA TO RED CELLS
This can result from:
Fragmented RBC's on the peripheral smear (helmet cells, burr cells, triangle cells, target cells,
schistocytes)
These hemolytic anemias seldom last long, but indicate serious disease.
* "March hemoglobinuria" is another cause of intravascular hemolysis from trauma; it is well
tolerated.
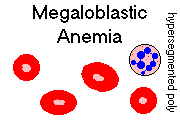
MEGALOBLASTIC ANEMIAS
This is a broad term for all problems in which the normoblasts (and, often, the other cells in the
body) cannot synthesize DNA fast enough to keep up with the growth of their cytoplasm.
("Nuclear-cytoplasmic asynchrony". This is easily the most plausible explanation; remember you
also need B12 to do methionine and methyl-malonic acid). Although patients will be anemic, the
baby cells (-"blast") end up big ("megalo-"), and a good pathologist can immediately recognize a
"megaloblastic marrow smear" by the big, blue cells with lots of cytoplasm and immature-looking
nuclei. (Polys and their precursors are big, too. You'll see pictures; I won't ask you to make the
distinction on an exam.)
Regardless of the cause, expect to see:
Rule: Count one hundred neutrophils. Separate segments are defined to be masses separated by a
thread composed entirely of heterochromatin. If you see one neutrophil with six segments, or five
with five segments, you have established the diagnosis of megaloblastic anemia. I think a three-lobed eosinophil does
it, too.
Pernicious anemia ("true pernicious anemia", "addisonian pernicious anemia", etc.)
This is extremely common, especially
in older folks; one group argues that there must be 800,000
undiagnosed cases (Arch. Int. Med. 156: 1097, 1996).
Once dreaded and very lethal ("pernicious"), the available of injectable B12 (in the old days, a pound
of raw liver per day by mouth, or liver injections) has now rendered this common problem almost
innocuous.
The basic problems is chronic atrophic (usually autoimmune; most (>90%) of these patients have
antibodies against the parietal cell canaliculi) gastritis with destruction of the parietal cells and
failure of intrinsic factor production.
Often (maybe 40% of the time) there is some antibody that sticks to intrinsic factor as well,
preventing its binding to B12 ("blocking antibody", * type I's). There's also likely to be antibodies
against receptors in the ileum where the complex must be absorbed ("binding antibody", * type II's).
Assay J. Clin. Path. 46: 45, 1993 (* contrary to older sources, either can be present without the
other).
* While we are ordering unnecessary lab tests, most of these patients have elevated serum gastrin
levels, too (why?).
In addition to the problem making good blood cells, B12 deficiency (from whatever cause) is noxious
to the brain and cord, probably because of increased levels of methyl-malonic acid and propionic acid.
Demyelinization of the posterior columns of the spinal cord happens early and causes loss of
proprioception and some paresthesias, as in tabes dorsalis. Eventually, dementia occurs. These
problems may precede the anemia (Postgrad. Med. 91: 231, 1992; Postgrad. Med. 88: 147, 1990).
In the 1980's, I had the rare privilege of autopsying a "virgin" pernicious anemia patient, a
gentleman who was institutionalized for five years with "Alzheimer's disease". His physicians drew
blood from time to time, but never noticed the anemia, the MCV of 140, or the hypersegmented
neutrophils reported by the lab. Bad care. I noted each of the following "classic" changes:
NOTE: Often the lateral columns are affected, too, though less dramatically. This is called "subacute combined degeneration
of the cord", typical of B12 deficiency.
To make the diagnosis, physicians who practice good medicine perform the two-part Schilling test.
Give the patient an injection of normal B12 first (why?)
Then administer radioactive B12 by mouth. A healthy person will excrete the radioactivity in the
urine. If your patient, for any reason, cannot absorb B12 via the gut, the urine will not be
radioactive.
If your patient cannot absorb B12 via the gut, then give him or her a dose of radioactive B12
with
intrinsic factor. If this causes the radioactivity to appear in the urine, you know the patient lacks
intrinsic factor. If the radioactivity still fails to appear, you know there's some problem with
absorption (i.e., one of those antibodies and/or some disease of the gut).
It's common knowledge that patients with autoimmune gastritis, whether or not they have pernicious
anemia, are at substantial risk for gastric cancer (carcinoma, carcinoid; see for example Cancer 71:
745, 1993 and Arch. Path. Lab. Med. 113: 399, 1989). It's ironic that, while the Japanese
endoscope almost everybody (and often finding the highly-curable early gastric cancer lesions),
we're just now getting used to the idea of endoscoping pernicious anemia patients regularly. For
some better-late-than-never common-sense see Gut 34: 28, 1993; endoscopy every five years, more
often if dysplasia is found, seems reasonable (Gut 31: 1105, 1990; Bill and Hillary take notice).
Classic "addisonian" pernicious anemia is primarily a disease of people of northern European
ancestry, though any race can be affected. The sex ratio is about equal, which is unusual for an
autoimmune disease.
"Juvenile pernicious anemia" mimics the adult disease in its hematologic and nervous system
manifestations. These patients don't usually have autoimmunity, but instead are born without good
intrinsic factor, or without receptors for the complex. Tip: Check the urine for methyl-malonic acid
(why?)
Other causes of B12 deficiency
"Inadequate diet" must be extreme. "Vegans", who will take no food of animal origin,
get B12 deficiency after a few five years unless they supplement.
B12 deficiency is common in today's "amateur" vegans, many of whom are
teens (Am. J. Clin. Nutr. 76: 100, 2002).
If your whole stomach is gone after some big operation, you'll need B12 supplementation, of course.
But this isn't true pernicious anemia.
If you have malabsorption (sprue, Whipple's, lymphoma, scleroderma, others), or if you have the
fish tapeworm on board, or if you have a blind loop (post-surgery, duodenal diverticula) full of
bacteria, or if your ileum is messed up badly by Crohn's disease, you may need B12.
* "Big Robbins" cites "increased need for B12" in carcinomatosis, hyperthyroidism, and pregnancy.
I've never seen this as a clinical problem, and because the vitamin is so available, I doubt its
seriousness.
There's a good serum assay for B12. It's expensive, but perhaps an occasional
screen is worthwhile, more for the mental problems that the deficiency causes
especially in the elderly. I'd prefer you start your anemia workup with a
reticulocyte count first.
* Hey Doc! Want to keep your poorly-educated patients happy and coming back ($$)? Some
physicians diagnose "pernicious anemia" wantonly, and prescribe monthly B12 shots, which are red
(ooh, pretty), painless, inexpensive, and harmless. Further, once you start doing this,
it'll be hard to prove the patient didn't originally need the treatment and doesn't
need to continue. However happy this common practice may make
people, I have a ninth commandment problem with it. I hope YOU do, too.
Folic acid deficiency (ever know someone who called it "vitamin P"? "folic" means "from (green)
leaves")
This is disturbingly common in the U.S., and not just in the alcoholics, oldsters, and babies cited in
"Big Robbins". Contrary to your text, the deficiency need not be "gross". You need some
vegetables in your diet every once in a while, and many Americans don't like them. (In the poor
nations, many people can't afford them.) If you lack folic acid, you can't shuttle your one-carbon
units (i.e., methyl and formyl groups) around.
In pregnancy, the fetus leeches out Mom's folic acid, which may already be in short supply.
Likewise, in hemolytic disease and in carcinomatosis, folic acid supplies often drop, a "relative folic
acid deficiency" is unmasked, and a superimposed megaloblastic state develops.
Phenytoin and the birth control pill are infamous for interfering with the absorption of folic acid. Of
course, so can other malabsorption problems. Hemodialysis takes the vitamin out of the body, too.
A blood assays for folic acid is available. Again, it's expensive. I'd prefer you not order these for all
your microcytic anemia patients at the onset of your workup. Tip: You can also detect folate
deficiency by assaying the urine for formimino-glutamic acid (FIGlu), a breakdown product of
histidine which requires folate for further processing.
BEWARE. Supplementing a patient with pernicious anemia with big doses of folic acid will
improve the hematologic picture (nobody knows why) and exacerbate the brain disease (nobody
knows why). This is the main reason that only small amounts of folic acid are put in over-the-counter not-for-pregnancy
vitamins.
B12 and folate-unresponsive megaloblastic anemia
Obviously, anti-DNA chemotherapy will produce megaloblastic changes.
Occasional megaloblastic anemias respond well to vitamin B1 (thiamine) or vitamin B6
(pyridoxine).
These are usually acquired, and probably reflect Nowell's law hits (i.e., there is an increased
leukemia risk.)
Note: Heavy alcohol drinking, and sometimes liver disease (maybe) and hypothyroidism (maybe),
will raise the MCV to maybe 110 fL. Nobody knows why.
IRON DEFICIENCY ANEMIAS
You already know that iron is absorbed (in limited, regulated quantities) in the duodenum, shuttled
around on transferrin, used in hemoglobin, myoglobin, and cytochromes, and the storage supply
found to ferritin as the invisible short-term form ferritin and the copper-penny, Prussian-blue-stainable long-term form
hemosiderin.
A person may become iron-deficient by:
Poor diet is seldom the sole cause in U.S. adults. However U.S. kids can and do
become iron deficient, despite "Big Robbins"). There is very little iron in
breast milk, and children do become deficiency as a result. No one knows the "best"
amounts and timing for supplementation (Ped. Clin. N.A. 48: 401, 2001).
Doc: If you find iron deficiency, you MUST find the cause. It is cancer of the GI or GU system
until proven otherwise.
Around 10% each of toddlers, teenaged girls, and moms are iron deficient,
and of these, around half are anemic (JAMA 277: 973, 1997).
More numbers: Almost 20% of kids are iron-deficient, with 5% anemic (Clin. Ped. 44:
333, 2005); easy to diagnose, but these kids are still not beingfollowed up.
Of
course this is deplorable. An attempt by the English to alter the
junk-food habits of their underclass through "education"
was an expensive, complete failure (Arch. Dis. Child. 76: 144,
1997).
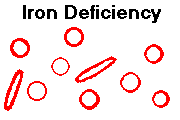
Regardless of the cause, the iron-deficient patient develops a hypochromic, microcytic (why?)
anemia, which can be very severe.
You'll be impressed the first time you see tiny red cells with broad central pallor.
For some reason, elongated "pencil RBC's" are common in iron deficiency, and the platelet count
tends to rise.
Textbooks describe a variety of additional physical findings that are supposed to be more or less
specific for iron deficiency. This includes koilonychia (spoon-shaped nails), beefy glossitis,
intestinal malabsorption, and upper esophageal webs ("Plummer-Vinson"; the link to iron deficiency
is almost certainly a myth, and I have my doubts about the others, since they make no sense
physiologically).
Plasma ferritin levels usually closely correlate with total body iron, provided that the liver isn't
acutely damaged. More about iron testing when we cover lab testing.
* Tip: Allied health professionals often refer to both hemoglobin and hematocrit as "serum iron". I've
given up trying to explain.
ANEMIA OF INFLAMMATION ("Anemia of Chronic
Disease", Ped. Clin. N.A. 43: 623, 1997;
Am. J. Med. Sci. 307: 353, 1994)
Here, there's plenty of iron in the body, but it isn't available to the normoblasts, but stays in the big
fixed macrophage in the center of the erythroid island.
This unfortunate effect is mediated by increased body levels of interleukin 1 (* and probably other
cytokines too), i.e., the macrophages are phagocytosing somewhere in the body, and the "acute phase
reaction" has been going on long enough to cause lowering of the hematocrit.
* The primacy of the iron problem is confirmed by the use of zinc protoporphyrin (i.e., free
porphyrin) levels as marker for anemia of chronic disease: Blood 81: 1200, 1993.
* There may also be a component of hemolysis (by those hungry macrophages) though I haven't seen
increased reticulocyte counts in these folks. Or the kidney may not be making enough
erythropoietin.
This is a common, often-overlooked / undertreated problem in AIDS (J. Inf. Dis. 185(S2): S-105 & S-110, 2002);
perhaps the availability of newer erythropoietin-like medications will result in this being
treated more effectively.
Patients have a hypochromic-microcytic (why?) anemia with a hemoglobin of around 8-10 gm/dL.
Bone marrow iron stores are increased.
In the U.S., the usual causes are rheumatoid arthritis, osteomyelitis, TB, and huge bedsores.
(Remember these also cause amyloidosis A; same underlying problem.) Treat the underlying cause,
Doc.
* If you want to diagnose and monitor the disease, try serial zinc protoporphyrins (Blood 81: 1200,
1993; why does it work?)
* For tough cases, you can try erythropoietin.
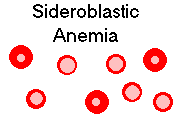
SIDEROBLASTIC ANEMIA
Once again, there's plenty of iron in the body, and this time, it's even in the normoblasts. But in this
relatively uncommon problem, patients have difficulty placing the iron into their heme rings.
Instead, it remains in the mitochondria, which light up as Prussian-blue positive chunks in their
ordinary position around the normoblast nucleus (hence the cute term "ringed sideroblasts").
Commonly, only some of the red cell precursors are affected (i.e., Nowell's law has been operating;
these patients are probably at increased risk for leukemia.) Alcoholism and isoniazid therapy also
get cited.
* In the X-linked hereditary sideroblastic anemia, the problem is with
δ-amino levulinic acid
synthetase (NEJM 330 675, 1994; Blood 90: 872, 1997;
Blood 93: 1757, 1999). Some cases respond to big doses of pyridoxine, and
in these
cases, the pyridoxine binding site on the protein is what was hit by the mutation (of course).
More on this: Blood 93: 1757, 1999.
PURE RED CELL APLASIA
In babies, congenital difficulty with erythropoiesis is the Blackfan-Diamond syndrome
and variants. * Another variant (autosomal dominant
dyskeratosis congenita) lacks the ability to restore telomeres to
the endlessly-dividing marrow stem cells (Lancet 359: 2168, 2002; Blood 102: 916, 2003).
In the Fanconi C variant, the red cells are oversensitive
to signals from γ-interferon (and surely other stuff)
to undergo apoptosis (Blood 90: 974 & 1047,
1997; Blood 88: 2298, 1996), etc., etc. There are at least
8 Fanconi anemia (red cell underproduction, fragile chromosomes) loci,
all autosomal recessive (Am. J. Hum. Genet. 61: 940, 1997.
* Hypoplastic anemia and an extra joint in the thumb: Aase syndrome! In the chronic hemolytic disorders (notoriously sickle-cell disease, less often spherocytosis or
hemoglobin C disease), the production of normoblasts can simply shut down, even when there's
enough folic acid around. Parvovirus
19 is now known to be the usual cause.
This is called aplastic crisis.
Patients with thymoma / thymic hyperplasia often develop a red-cell aplasia, probably because T-cells
attack
the normoblasts in the bone marrow. Removing the thymoma often solves the problem
(Am. J. Clin. Path. 103: 346, 1995).
Patients who take chloramphenicol can all expect some temporary suppression of erythropoiesis, and
in 1 case in about 25,000 this is severe and permanent.
In kidney disease, there's often a lack of erythropoietin, and patients receive injections of the stuff,
which helps.
FINISHING UP: Thankfully, hemoglobins with excessively high
oxygen affinity ("Chesapeake" and many others) are uncommon.
As you'd expect, these render the patient polycythemic.
* Red-cell substitutes have been a disappointment. A bovine hemoglobin
preparation delivers the goods but only lasts for a day in the bloodstream; it is now in use in some nations.
The older perfluorocarbon emulsions ("Fluosol", others) required patients to breathe 100% oxygen
which was deadly to the lungs. Review Am. J. Clin. Path. 118 S: S-71, 2002.
We'll do polycythemia vera,
other secondary polycythemias,
acquired aplastic anemia, and the myelodysplastic syndrome under
"White Cells". Enjoy these pictures:
{13856} red cell, normal blood. (If platelets
stick to polys, it's EDTA anticoagulant effect ("satellitism"). Some folks have a gene to
make this happen.)
JEHOVAH'S WITNESSES AND BLOOD TRANSFUSION
Ask a spokesperson for the details. "Many Jehovah's Witnesses
feel that accepting a blood transfusion will lead them to eternal
damnation" (Ob. Gyn. 102: 173, 2003).
Here are some references which
will help you in your thinking.
On the one hand...
On the other hand...
{13858} red cell, normal marrow, unusual stain
 Spherocytosis
Spherocytosis
Spleen
WebPath Photo

 Hereditary ovalocytosis
Hereditary ovalocytosis
Nice smears
Rockford Case of the Month
There's also sickle-cell disease among Sicilian whites; for some
reason it is much milder (Arch. Ped. Adol. Med. 150: 170, 1996).
And there are some affected areas in East Asia.
 Sickle cell spleen
Sickle cell spleen
Photo and mini-review
Brown U.
 Sickle cell disease
Sickle cell disease
Autosplenectomy
WebPath Photo
* Pathology of pulmonary hypertension in sickle cell disease: Hum. Path. 33:
1037, 2002.
 Sickle cell lung
Sickle cell lung
Big case; follow the arrows
Dr. Warnock's Collection
 Hemoglobin C
Hemoglobin C
WebPath Photo

 Hydrops fetalis
Hydrops fetalis
Intrauterine death from Rh disease
KU Collection

 α thal major
α thal major
WebPath Case of the Week
* Despite older reports of
transformation into leukemia, nowadays PNH doesn't seem to do this much, nobody knows why
(NEJM 333: 1253, 1995).
Since red cells have no class I HLA antigens, T-cells
do not attack them.
 Schistocytes
Schistocytes
WebPath Photo
* Anemias induced by chemotherapy tend to be undertreated, probably
because they are difficult to treat.
Perhaps the new, more-effective erythropoietin-like drug darbepoietin will
prove helpful (Cancer 95: 613, 2002).
Iron deficiency (mechanism still mysterious Am. J. Clin. Nutr. 72(S2):
549-S, 2000, may include GI and GU loss), hemolysis from pavement-pounding
("footstrike hemolysis"), and hemodilution by an expanded plasma volume (physiologic, to reduce
whole blood viscosity for the best oxygen delivery) all contribute
to "runner's anemia" (Ped. Clin. N.A. 49: 553, June 2002; JAMA
case conference 286: 714, 2001).
 bad diet (there's not much iron in twinkies, fries, or diet pepsi;
half of adults in the poor nations are iron deficient).
bad diet (there's not much iron in twinkies, fries, or diet pepsi;
half of adults in the poor nations are iron deficient).
Heme iron is much better absorbed
than iron from beans. Especially, there is disappointingly little usable iron in
spinach; what's there is oxalate-bound and unavailable
The
problem in common Blackfan-Diamond that the normoblasts undergo apoptosis unless they are awash with erythropoietin
(Blood
83: 645, 1994; Blood 87: 2568, 1996; further complexities Blood 105:
838 & 4620, 2005).
* The gene is ribosomal protein S19: Nat. Genet. 21:
169, 1999.
 Future pathologists wishing to spot "parvo":
You will see no normoblasts beyond the basophilic stage,
and the basophilic normoblasts have the nuclear chromatin
pushed to the edge by the viral inclusion.
Future pathologists wishing to spot "parvo":
You will see no normoblasts beyond the basophilic stage,
and the basophilic normoblasts have the nuclear chromatin
pushed to the edge by the viral inclusion.
* Some kidney patients treated with recombinant erythropoietin
develop anti-erythropoietin antibodies and a severe aplastic anemia: NEJM 346:
469, 2002; responds to treatment Lancet 363: 1768, 2004.
Sooner or later, you will run into the issue of blood for Jehovah's Witnesses.
The group is authoritarian, tightly-controlled,
and forbids blood transfusions for its members.
{13976} red cell, normal blood (two orthochromatic normoblasts)
{20780} red cell, normal blood
{46538} red cell, normal blood
{26161} basophilic normoblast (prorubricyte)
{26162} basophilic normoblast (prorubricyte)
{26197} basophilic normoblast (prorubricyte)
{26198} basophilic normoblast (prorubricyte)
{26223} polychromatophilic normoblast (rubricyte)
{26224} polychromatophilic normoblast (rubricyte)
{18690} orthochromatophilic normoblast (metarubricyte)
{10127}red cell, even staining for hemoglobin
{10130} Heinz bodies
{10418} nucleated red cells in hemolytic disease of the newborn
{21113} hemolytic disease of the newborn
{13898} polychromasia (the purple, large red cells are "reticulocytes")
{14722} reticulocytes, normal
{14723} reticulocytes, too many
{39616} erythroid hyperplasia
{39617} erythroid hyperplasia
{27434} plasmodium vivax
{13880} cold agglutinins in the blood
{12299} hereditary spherocytosis
{16172} spherocytes
{11547} hereditary elliptocytosis (spherocytosis variant)
{13892} hereditary elliptocytosis (spherocytosis variant)
{12305} spur cells ("acanthocytes"' E.T.-finger cells); abetalipoproteinemia case
{13871} abetalipoproteinemia smear (lymphocyte in upper right)
{20128} abetalipoproteinemia smear
{17419} sickle cell disease
{13907} target cells
{16167} target cells
{16177} target cells
{16169} stomatocytes (flattened uniconcave RBC's typical of acute drunkenness, liver disease and
various rarities, everyone's allowed a few)
{12308} schistocytes
{13895} schistocyte
{16178} schistocytes
{17137} DIC
{20149} thalassemia
{13877} basophilic stippling
{10430} "megaloblasts" (i.e., the red cell precursors in pernicious anemia)
{13751} megaloblastic blood smear
{13754} megaloblastic marrow
{13757} megaloblastic marrow
{13889} macro-ovalocytes (i.e., megaloblastic anemia)
{12302} teardrops

{14013} sideroblastic blood (dimorphic RBC population)
{27342} ringed sideroblasts, iron stain (not the greatest photo)
{09054} iron in mitochondria
{14025} Pappenheimer body (retained iron-loaded mitochondrion, i.e., you have sideroblastic
anemia and/or have had a splenectomy; you need a Prussian blue stain to see them well)
{16168} Pappenheimer bodies
{13854} polycythemia vera blood
{13976} rouleaux
{14028} multinucleated red cell (DiGuglielmo's?)
{23920} myelodysplastic syndrome
{13883} Howell-Jolly bodies (stray chromosomes not extruded; usually mean the patient has had a
splenectomy and they were not removed)
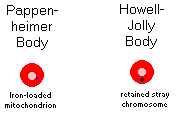
{16170} Howell-Jolly bodies
{13904} post-splenectomy
{29011} blood bank
 Howell-Jolly bodies and nucleated red
Howell-Jolly bodies and nucleated red
WebPath Photo
Let the young sing songs of death. They are stupid. The finest
thing under the sun and the moon is the human soul. I marvel
at the small miracles of kindness that pass between humans.
I marvel at the growth of conscience, at the persistence of
reason in the face of all superstition and despair. I
marvel at human endurance.
-- Anne Rice, Pandora ("The
Vampire Chronicles")
| Visitors to www.pathguy.com reset Jan. 30, 2005: |
Ed says, "This world would be a sorry place if
people like me who call ourselves Christians
didn't try to act as good as
other
good people
."
Prayer Request
 Teaching Pathology
Teaching Pathology
PathMax -- Shawn E. Cowper MD's
pathology education links
Ed's Autopsy Page
Notes for Good Lecturers
Small Group Teaching
Socratic
Teaching
Preventing "F"'s
Classroom Control
"I Hate Histology!"
Ed's Physiology Challenge
Pathology Identification
Keys ("Kansas City Field Guide to Pathology")
Ed's Basic Science
Trivia Quiz -- have a chuckle!
Rudolf
Virchow on Pathology Education -- humor
Curriculum Position Paper -- humor
The Pathology Blues
 Ed's Pathology Review for USMLE I
Ed's Pathology Review for USMLE I
 | Pathological Chess |
 |
Taser Video 83.4 MB 7:26 min |